





|
STUDENT DIGITAL NEWSLETTER ALAGAPPA INSTITUTIONS |

|
Stephen A. Boorjian, MD, FACS
Efforts should be made to prevent the development of bacterial endocarditis in children with cardiac anomalies (see Chapter 12) rheumatoid arthritis ribbon color 16 mg medrol for sale. The diagnosis should be suspected in any child with a significant cardiac murmur and a prolonged fever arthritis relief at your fingertips medrol 4 mg low cost. An age exception is premature infants with an indwelling catheter who can become infected with a fungus arthritis medications common cheap medrol 4 mg otc. A change in murmur intensity is not necessarily an indication of endocarditis arthritis in old dogs home remedies buy medrol 16mg without a prescription, since cardiac output and murmur loudness increase normally with fever arthritis in the fingers pictures buy 4 mg medrol with mastercard. Signs of recurrent pneumonia or a pleuritic type of pain may indicate embolization of infected material to the lungs rheumatoid arthritis vs gout quality 16 mg medrol. Signs of systemic embolization, such as splenomegaly, hematuria, splinter hemorrhages, and central nervous system signs, should be sought in any febrile patient with a cardiac anomaly. Laboratory findings the diagnosis is confirmed by obtaining the organisms from a blood culture. At least six blood cultures should be taken within the first 12 or 24 hours that endocarditis is suspected. It is not necessary to wait for a fever spike, since the chance of obtaining a positive culture depends primarily upon the volume of blood drawn. It is important that blood cultures of ample volume be obtained prior to antibiotics otherwise the chance of recovering an organism is reduced by an estimated 40%. Echocardiography is not usually helpful in making a diagnosis, because the absence of valve changes or vegetations does not exclude endocarditis. Echocardiography can be helpful by confirming acute changes in valve function suspected clinically. When vegetations are seen, they may persist long after successful antibiotic treatment is concluded. Endocarditis is a clinical and a laboratory diagnosis, not necessarily an echocardiographic diagnosis. Treatment If the patient is very ill or if the clinical findings are typical, antibiotic treatment can be initiated immediately after the cultures have been obtained and before the results of cultures are available. If the diagnosis is questionable, initiation of therapy should await the results of the blood cultures. The general principles of treatment are that antibiotics must be parenteral (usually intravenously administered), bactericidal, and that treatment must be prolonged. The exact treatment depends on the organism isolated and its antibiotic sensitivities. Initial empiric treatment varies according to the clinical situation, for example, whether the patient has been treated with antibiotics prior to cultures, whether prosthetic valves, material, or devices such as pacing leads are present, and whether the presentation is acute (and more likely to be staphylococcal) or subacute. Other considerations are patient allergy to particular drugs and the knowledge of local antibiotic resistance patterns. Low-dose gentamicin, rifampin, or other antibiotics are often added for synergistic effect. During and following completion of therapy, blood cultures should be obtained to verify eradication of the infection. Despite the availability of antimicrobials, endocarditis can lead to major complications, such as valvar damage or permanent sequelae resulting from embolization; occasionally, the disease is fatal. Marfan syndrome patients are typically tall and thin, showing a high incidence of kyphoscoliosis, pectus carinatum or excavatum, arachnodactyly, high-arched palate, and loose joints. Cardiac anomalies occur in almost all patients and lead to premature death, although death rarely occurs in childhood. Aneurysmal dilation of the ascending aorta and aortic sinuses occurs and leads to aortic regurgitation, which may become severe. Mitral valve prolapse and regurgitation are common, resulting from elongated chordae tendinae and redundant valve leaflets. Criteria for diagnosis are available, most recently published as the article "The revised Ghent nosology for the Marfan syndrome" (see Additional reading). Cardiac auscultation may be normal, or a systolic ejection click may result from aortic root dilation. If aortic regurgitation is present, an early diastolic murmur may or may not be audible. Mitral valve prolapse, if present, creates sounds as described in the next main section Mitral Valve Prolapse. Chest X-ray the chest X-ray may be normal or can show dilation of the ascending aorta. Echocardiogram An echocardiogram is useful for the screening and diagnosis of patients suspected of Marfan syndrome (Figure 9. For patients diagnosed with a connective tissue disorder, periodic echocardiography is indicated to detect progressive aortic dilation and valve regurgitation. Additional references for health professionals and diagnostic aids, including z-score calculators, are available from the National Marfan Foundation at. Aortic surgery is performed prophylactically to reduce the risk of sudden death by aortic dissection. The timing of aortic surgery depends on family history and individual patient findings, such as the presence of aortic dissection, important valvar regurgitation, rapid enlargement of the aortic root, and absolute size of the aorta. Replacement of the aortic valve is often combined with replacement of the ascending aorta with a prosthetic graft or homograft to prevent dissecting aneurysm. In some patients, the aortic root is replaced with prosthetic material, leaving the native aortic valve in place. The long-term prognosis following these operations is good, but other segments of the aorta may remain at risk for aneurysm and dissection. Usually first recognized in adolescence, it is rare in childhood; thus, it may represent an acquired condition or a congenital condition with late presentation, analogous to connective tissue disorders. When a child is diagnosed with mitral valve prolapse, subtle congenital anomalies, such as mitral cleft or anomalous coronary artery, must be ruled out, in addition to acquired disorders such as hyperthyroidism or cardiac inflammatory diseases. A positive family history may exist, but the etiology and pathology are largely unknown. Because of its seeming ubiquitous nature in young adults and the lack of consensus about what constitutes prolapse, controversy persists about the true incidence. Various symptoms are often attributed to mitral valve prolapse, including chest pain, palpitations, near-syncope, syncope, and "panic attacks. The symptoms may represent a mild form of autonomic nervous system dysfunction, for which mitral prolapse is a weak marker. At the apex a mid- or late-systolic murmur exists that often begins with one or multiple mid-systolic to late-systolic clicks. Any maneuver that decreases left ventricular diastolic volume, such as a Valsalva maneuver, standing, or inhalation of amyl nitrate, causes the murmur to begin earlier and last longer. The click occurs earlier with standing and later with squatting or in the supine position. Laboratory findings the electrocardiogram and chest X-ray are usually normal in the absence of significant regurgitation. Echocardiography may show either one or both mitral valve leaflets prolapsing into the left atrium. The prolapse occurs maximally in mid-systole and may be associated with mitral regurgitation beginning in mid- or late systole. Current equipment is sufficiently sensitive that "physiologic" trace mitral regurgitation is commonly seen in normal individuals without prolapse. There is very little risk of sudden death, provided that mitral regurgitation is not severe and that mitral prolapse is not related to another condition, such as intrinsic cardiomyopathy, systemic disorder, or myocardial ischemic problem. Embolic stroke is so rare that the association with mitral prolapse remains controversial. Endocarditis is rare in individuals with mitral valve prolapse, and the indications for prophylactic antibiotics are controversial; the American Heart Association no longer recommends routine prophylaxis. Some with marked mitral regurgitation and/or myxomatous valve leaflets may be at greater risk and the decision to provide prophylaxis is individualized. The most common in our experience are (a) idiopathic, presumed viral; (b) purulent; (c) juvenile rheumatoid arthritis or systemic lupus erythematosus; (d) uremia; (e) neoplastic diseases; and (f) postoperative (postpericardiotomy syndrome). The symptoms that result from pericardial fluid depend on the status of the myocardium and the volume and the speed at which the fluid accumulates. A slow accumulation of a large volume is better tolerated than the rapid accumulation of a small volume. Cardiac tamponade can develop because of fluid accumulation within the pericardial sac. The pericardial fluid can compress the heart and interfere with ventricular filling. Three mechanisms compensate for the tamponade: (a) elevation of atrial and ventricular end-diastolic pressures; (b) tachycardia to compensate for lowered stroke volume; and (c) increased diastolic blood pressure from peripheral vasoconstriction to compensate for diminished cardiac output. Clinical and laboratory findings are related to (a) inflammation of the pericardium, (b) cardiac tamponade, and (c) etiologic factors. History and physical examination Pericarditis is accompanied by pain in about half of patients. It is located in the left thorax, neck, or shoulder and is improved when the patient is sitting. A pericardial friction rub, a rough scratchy sound, may be present over the precordium. It is louder when the patient is sitting, or when the stethoscope is pressed firmly against the chest wall. No relationship between the amount of pericardial fluid and the presence of a rub has been found, but with a large effusion a rub is often not heard. As the stroke volume falls because of the tamponade and limited ventricular filling, the heart rate increases to maintain cardiac output. Peripheral pulses diminish as systemic vasoconstriction heightens and the pulse pressure narrows. Central pulses diminish because of the narrow pulse pressure and decreased stroke volume. Excess pulsus paradoxus, a decrease in pulse pressure of more than 20 mmHg with inspiration (normal is less than 10 mmHg), is also highly diagnostic of tamponade and can often be identified by palpation of the radial pulse. Certain viral agents, such as Coxsackie B, have been identified as causative agents for pericarditis. In these patients, frequently a history of a preceding respiratory infection is found. Among patients with purulent pericarditis, Hemophilus influenzae, pneumococcus, and staphylococcus are the most common organisms. Purulent pericarditis usually occurs in infancy and may follow or be associated with infection at another site, such as pneumonia or osteomyelitis. An important clue in some infants and toddlers may be grunting respirations in the absence of auscultatory or radiographic evidence of pneumonia. Pericarditis can develop secondary to juvenile rheumatoid arthritis and may occur before other manifestations of this disease. Chest X-ray the chest X-ray may be normal, but the cardiac silhouette enlarges proportionately with accumulation of pericardial fluid. Echocardiogram Pericardial effusion can be recognized fairly accurately by echocardiography, and this technique may be helpful in diagnosing suspicious cases. Often the fluid can be characterized as purulent rather than serous because leukocytes are more echogenic (giving an echo-bright cloudy or smoky appearance) than fluid alone (which appears black by 2D echocardiography). Left ventricular diastolic diameter may be reduced because of inability of the ventricle to fill properly. Tamponade is accompanied by dilation of the hepatic veins, vena cavae, and early diastolic "collapse" of the right atrium and right ventricle. In patients with purulent pericarditis, pericardiocentesis is indicated, since reaching an etiologic diagnosis is imperative so that appropriate antibiotic therapy can be initiated. Other than in patients with neoplasm and purulent pericarditis, the analysis of the fluid rarely yields a diagnosis. Pericardiocentesis is often indicated as an emergency procedure to treat the significant cardiac tamponade by removing fluid, thereby allowing adequate cardiac filling. At times, particularly with recurrent tamponade, a thoracotomy with creation of a pericardial window is indicated to decompress the pericardial sac. Pericardiectomy, removal of a large panel of the parietal pericardium, is sometimes performed, especially in purulent pericarditis, in the hopes of avoiding late restrictive pericarditis as the sac scars and contracts. Digoxin and diuretics are contraindicated because they slow the heart rate and reduce the filling pressure, contrary to the normal compensatory mechanisms for tamponade. High doses of antibiotics are indicated in purulent pericarditis, the type to be determined by antibiotic sensitivities, and open or closed drainage may be necessary. Appropriate cultures for mycobacteria and fungus should be performed, especially in immunocompromised patients. Skin tests for mycobacterial and fungus infection, with appropriate controls, may be helpful, especially if cultures prove negative. In patients with a primary inflammatory disorder, such as lupus, effective treatment of the underlying disorder with appropriate agents, such as steroids and other immunosuppressants, usually results in resolution of the pericarditis and effusion. Chapter 10 Abnormalities of heart rate and conduction in children Alterations in cardiac rate Atrial and atrioventricular arrhythmias Junctional arrhythmias Ventricular arrhythmias Conduction disturbances Shortened atrioventricular conduction (pre-excitation syndromes) Prolonged atrioventricular conduction General principles of tachyarrhythmia diagnosis and management Initial clinical assessment Differential diagnosis and management in stable patients Long-term management Additional reading 291 292 298 299 302 302 304 307 307 308 313 313 Disturbance of cardiac rate and conduction occur in children with no history of preceding cardiac disease, as a manifestation of congenital or acquired cardiac disease, as a complication of drug therapy, particularly digoxin therapy, or as a manifestation of metabolic, particularly electrolyte, abnormalities. Cardiac arrhythmias can be generally classified as (1) alterations in cardiac rate or (2) abnormalities of cardiac conduction.
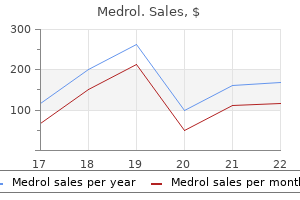
An occasional patient not adequately controlled by (or intolerant to) a dose given at 12-hour intervals may be dosed at eight-hour intervals arthritis neck inflammation generic medrol 4mg online. Once adequate control of the arrhythmia has been achieved arthritis in neck bones cheap 4mg medrol with mastercard, it may be possible in some patients to reduce the dose as necessary to minimize side effects or effects on conduction arthritis pain under knee cap order 4mg medrol amex. Any use of flecainide in children should be directly supervised by a cardiologist skilled in the treatment of arrhythmias in children arthritis back chiropractic 16mg medrol otc. Because of the evolving nature of information in this area arthritis queensland ceo purchase 4mg medrol overnight delivery, specialized literature should be consulted arthritis pain worse when it rains cheap medrol 16 mg on line. Under six months of age, the initial starting dose of flecainide in children is approximately 50 mg/M2 body surface area daily, divided into two or three equally spaced doses. Over six months of age, the initial starting dose maybe increased to 100 mg/M2 per day. In some children on higher doses, despite previously low plasma levels, the level has increased rapidly to far above therapeutic values while taking the same dose. Small changes in dose may also lead to disproportionate increases in plasma levels. Plasma trough (less than one hour pre-dose) flecainide levels and electrocardiograms should be obtained at presumed steady state (after at least five doses) either after initiation or change in flecainide dose, whether the dose was increased for lack of effectiveness, or increased growth of the patient. For the first year on therapy, whenever the patient is seen for reasons of clinical follow-up, it is suggested that a 12-lead electrocardiogram and plasma trough flecainide level are obtained. In patients with less severe renal disease, the initial dosage should be 100 mg every 12 hours; plasma level monitoring may also be useful in these patients during dosage adjustment. In both groups of patients, dosage increases should be made very cautiously when plasma levels have plateaued (after more than four days), observing the patient closely for signs of adverse cardiac effects or other toxicity. It should be borne in mind that in these patients it may take longer than four days before a new steady-state plasma level is reached following a dosage change. Based on theoretical considerations, rather than experimental data, the following suggestion is made: when transferring patients from another antiarrhythmic drug to flecainide allow at least two to four plasma half-lives to elapse for the drug being discontinued before starting flecainide at the usual dosage. In patients where withdrawal of a previous antiarrhythmic agent is likely to produce life-threatening arrhythmias, the physician should consider hospitalizing the patient. When flecainide is given in the presence of amiodarone, reduce the usual flecainide dose by 50% and monitor the patient closely for adverse effects. Plasma level monitoring is strongly recommended to guide dosage with such combination therapy (see below). Plasma Level Monitoring the large majority of patients successfully treated with flecainide were found to have trough plasma levels between 0. The probability of adverse experiences, especially cardiac, may increase with higher trough plasma levels, especially when these exceed 1 mcg/mL. Plasma level monitoring is required in patients with severe renal failure or severe hepatic disease, since elimination of flecainide from plasma may be markedly slower. The 50 mg tablets are plain on one side and debossed with "54 024" on the other side. The 100 mg tablets are scored on one side and debossed with "54 070" on the other side. The 150 mg tablets are scored on one side and debossed with "54 150" on the other side. It is especially appropriate for this essay to review and take stock of where we have been, where we are, and where we hope to be in the future. Lewis and his colleagues were the first to investigate the mechanism of this arrhythmia. This important finding suggests that the true circuit may have included the cavotricuspid isthmus. Atrial flutter occurrence compared with atrial fibrillation Authors Doliopoulos et al36 Makinson et al37 Katz and Pick38 Patients 3780 9458 50,000 Atrial fibrillation (%) 24. Furthermore, cryosurgical ablation of this critical region and its surrounding tissue prevented short-term recurrences of the arrhythmia. Gersh: this is an interesting account of the history of atrial flutter and provides a perspective ranging from the initial recognition of this distinctive electrophysiologic entity to an understanding of the anatomic characteristics of the circuit, which in turn have led to the therapeutic applications of radiofrequency ablation. Cannon "a" waves due to atrial contraction against a closed tricuspid valve may be observed. Cardiac auscultation may reveal a first heart sound of variable intensity: constant if the association of the atrial and ventricular contractions is maintained, and variable if it is not. An electrogram obtained with an esophageal electrode can also be used to make the diagnosis. This is well clarified by the authors in the subsequent discussion of mechanisms and the classification utilizing Table 3. Mechanisms, Nomenclature Atrial flutter is a condition in which, as has recently been shown, the contraction wave follows a circular and never ending path in the auricle, the circuits being completed a rate of from 240 to 350 per minute in different subjects. Its activation pattern can usually be determined by detailed, intracardiac mapping studies. Fig 7 shows a diagram of catheter arrangement in the right atrium frequently used in our electrophysiology laboratory to study flutter. The inferior isthmus is the target of radiofrequency ablation in most electrophysiology laboratories. Anteriorly, the circuit is bounded by the tricuspid orifice, while posteriorly, it is bounded by the anatomic barriers of the vena cavae orifices and eustachian ridge and the functional barrier of the crista terminalis. Schematic of catheter arrangement in the right atrium for flutter detection and ablation. Scars in the posterolateral and inferolateral right atrium have been found to be involved in flutter circuits. Patients who had prior surgery for congenital heart disease are a notoriously difficult and complex group of patients that are often difficult to treat with antiarrhythmic drugs. The lower schematic illustrates the reentrant circuit in the upper part of the right atrium. Mapping studies have revealed zones of slowed conduction or block and electrically silent regions serving as substrates for macro-reentry. Moreover, in some patients, atrial flutter may be the initial arrhythmia which degenerates into atrial fibrillation, and in this subset, the flutter circuit may be the primary target. Scar- and Pulmonary Vein-Related Atrial Flutter (Fig 14) Macro-reentrant circuits can rotate around one or more pulmonary veins or a scar in the posterior wall of the left atrium. The peri-pulmonary vein circuits can be cured with ablation by creating a lesion from a pulmonary vein to the mitral annulus or to the contralateral pulmonary vein. Interestingly, these patients had no prior surgery but low-voltage areas were found in the posterior wall and roof of the left atrium. The authors hypothesized that the atrial conduction slowing was due to antiarrhythmic agents (amiodarone, sotalol) or atrial myopathy (dilatation). Definitions for class categorization: Class I: Conditions for which there is evidence and/or general agreement that a given procedure or treatment is useful and effective. Conversion to sinus rhythm can be achieved with relatively low energy levels, usually less than 50 joules with monophasic shocks. Avoid in patients with structural heart disease, myocardial ischemia, significant sinus node, or conduction system dysfunction. Recently, Ermis et al95 compared monophasic shocks with biphasic shocks for cardioversion and found that biphasic shocks have a higher success rate and require less energy. External, electrical cardioversion generally requires anesthesia, which may not be an acceptable option in patients with tenuous respiratory status or who have eaten recently. In post-cardiac surgery patients, epicardial wires are usually in place and rapid atrial pacing to terminate the tachyarrhythmia can be easily carried out. When conventional atrial overdrive pacing techniques fail, high-frequency atrial pacing (50 Hz) or delivery of an atrial pacing train followed by extrastimuli can be effective. In addition, Class Ia and Ic drugs should be avoided in those with structural heart disease or myocardial ischemia. It may be useful, however, as an adjunctive to other agents, for example, beta- and calcium blockers. Atrial Flutter after Cardiothoracic Surgery Atrial tachyarrhythmias are frequently seen in the first two to three days after cardiothoracic surgery. They prolong the stay in the intensive care unit and increase perioperative morbidity and potentially mortality. Prophylaxis against atrial tachyarrhythmias after cardiac surgery has been studied, and a recent meta-analysis has found that both sotalol and amiodarone are equally effective, though amiodarone had fewer side effects requiring drug termination. Gersh: I would add the caveat that is important for serum electrolytes to be checked, since ibutilide and dofetilide can precipitate torsade de pointes. Oral dofetilide has been studied in two clinical trials126,127 and has an efficacy of about 70% in preventing flutter recurrences over a period of almost one year. Atrial flutter with 1:1 conduction is a very unpleasant complication in that the rapid rates can result in quite dramatic hemodynamic decompensation. Adequate rate control is difficult to achieve, and the arrhythmia is difficult to suppress. In addition, the toxicity, including proarrhythmia potential, associated with long-term antiarrhythmic drug therapy may outweigh its benefits. Gersh: this is not a frequent circumstance, but when it occurs, it provides a novel approach to the prevention of atrial fibrillation by ablating the drug-induced flutter circuit. A popular catheter arrangement is placement of a steerable 20-pole "halo" catheter close to the tricuspid annulus as shown in Fig 7. Successful ablation requires complete isthmus interruption by demonstrating bidirectional conduction block. However, such a pacing and mapping protocol may not be stringent enough to differentiate very slow conduction from conduction block as up to a 15% recurrence rate has been reported. Isthmus ablation can be performed during flutter until there is interruption of the tachycardia. But even after ablation, isthmus conduction, though significantly slowed, can still occur. To ensure a low recurrence rate, complete bidirectional block must persist for 25-30 minutes after ablation. Detailed atrial activation and entrainment mapping reveal areas of low voltage and conduction block that serve as anatomic obstacles for a macro-reentrant circuit. A review of Curr Probl Cardiol, March 2005 151 the operative report can sometimes provide important information about the atriotomy site and provide clues to the location of the circuit. Studies have shown that atrial septal defect repair is the most common cause of incisional reentry in adults. Circuits involving the mitral annulus,87,88 scars located around the pulmonary veins or in the posterior wall of the left atrium,87,88 coronary sinus,91 and left septum92 have been reported. As is the case with atrial fibrillation, the history of hypertension is a powerful risk factor for stroke in patients with atrial flutter. The lessons to be learned from studies on patients with atrial fibrillation is that asymptomatic recurrences are frequent and are a powerful risk factor for stroke. If this proves to be true in humans, then we envision a true continuum between these two arrhythmias with the clinical expression (ie, typical flutter, coarse flutter, fibrillation) being dependent on the number and course of one or more atrial rotors. The same holds true for the stereotactic electrophysiology laboratories which promise to revolutionize catheter manipulation. Observations upon a curious, not uncommon form of extreme acceleration of the auricle. Circus movement in the canine atrium around the tricuspid ring during experimental atrial flutter and during reentry in vitro. Intra-atrial reentry as a mechanism for atrial flutter induced by acetylcholine in rapid pacing in the dog. Role of abnormal atrial pathways, slow conduction, nonuniform refractory period distribution and premature beats. The effects on atrial electrophysiology and structure of surgically induced right atrial enlargement in dogs. Identification of reentry circuit sites during catheter mapping and radiofrequency ablation of ventricular tachycardia late after myocardial infarction. Demonstration of macroreentry and feasibility of operative therapy in the common type of atrial flutter. Radiofrequency ablation of the inferior vena cava-tricuspid valve isthmus in common atrial flutter. Hospitalization for arrhythmias in the United States: Importance of atrial fibrillation. Mapping and radiofrequency ablation of intraatrial reentrant tachycardia after the Senning or Mustard procedure for transposition ofthe great arteries. Fatkin D, MacRae C, Sasaki T, et al: Missense mutations in the rod domain of the lamin A/C gene as causes of dilated cardiomyopathy and conduction-system disease. Saoudi N, Cosio F, Waldo A, et al: A classification of atrial flutter and regular atrial tachycardia according to electrophysiological mechanisms and anatomical bases; a Statement from a Joint Expert Group from the Working Group of Arrhythmias of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Variable electrocardiographic characteristics of isthmus-dependent atrial flutter. Importance of atrial flutter isthmus in postoperative intra-atrial reentrant tachycardia. Nakagawa H, Lazzara R, Khastgir T, et al: Role of the tricuspid annulus and the eustachian valve/ridge on atrial flutter. Activation and entrainment mapping defines the tricuspid annulus as the anterior barrier in typical atrial flutter. The upper link of human common atrial flutter circuit: definition by multiple endocardial recordings during entrainment. Reversal of reentry and acceleration due to double-wave reentry: two mechanisms for failure to terminate tachycardias by rapid pacing. Brugada J, Boersma L, Kirchhof C, et al: Double-wave reeentry as a mechanism of acceleration of ventricular tachycardia.
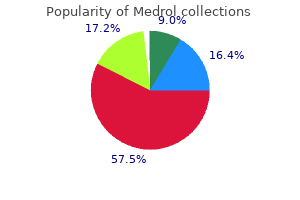
Asymptomatic patients benefit only when there is a reasonably high probability of underlying structural heart disease arthritis in back and hip pain medrol 16 mg on line. Such patients also benefit from additional echocardiography when there is a subsequent change in symptoms and signs arthritis in knee synvisc buy 16mg medrol visa, including pregnancy arthritis foundation diet order medrol 16 mg without a prescription. The timing and followup of interventions in patients with valvular heart disease is arthritis in back painful order medrol 4mg line, including prosthetic valves arthritis knee exam purchase 16mg medrol free shipping, can be guided by the parameters obtained by echocardiography arthritis in neck forum trusted 16mg medrol. Detection and characterization of vegetations and perivalvular structures is made possible by echocardiography (Table 12; Chapter 15). Hemodynamic findings suggesting intermittent obstruction to intracardiac flow Evaluation of clinical syndromes and events suggestive of underlying cardiac mass (I) Evaluation of underlying cardiac disease known to predispose to mass formation for whom a therapeutic decision regarding surgery or anticoagulation will depend on the results of echocardiography (I) Follow-up or surveillance studies after surgical removal or with masses known to have a likelihood of recurrence. Recommendations vary among institutions and the clinical scenario-critically injured patients have highly differing clinical circumstances. American College of Cardiology; American Heart Association; American Society of Echocardiography. American College of Cardiology; American Heart Association; American College of Physicians; American Society of Internal Medicine Task Force on Clinical Competence. However, if the findings do nothing to aid management, as in the terminally ill patient, there is no justifiable clinical role for echocardiography. Echocardiography in Adult Congenital Heart Disease Echocardiography plays an invaluable role in the management of adult congenital heart disease. Doppler echocardiography has largely obviated the need for invasive pre-operative assessment of shunts and gradients in this patient population (Table 15; Chapter 21 and 22). Two years previously, he underwent placement of an implantable cardioverter defibrillator with biventricular pacing following episodes of ventricular tachycardia. His additional medical problems included hypertension, dyslipidemia, chronic obstructive pulmonary disease, and chronic renal impairment. His jugular venous pressure was elevated and inspiratory crackles were heard halfway up both lung fields posteriorly. This is a fundamental part of the standard echocardiographic examination, but is especially important in patients with heart failure and post-myocardial infarction. Right ventricular size was not enlarged and right ventricular systolic function was preserved. In patients with chronic stable coronary artery disease, there is a consistent relationship between heart size and outcomes. It is simple, reproducible, accurate (when properly applied), and provides excellent endocardial border definition (owing to high frame rate). The epicardium lies just anterior to the highly echo-reflective parietal pericardium (see Chapter 3. An exponential relationship exists between ventricular diameters and ventricular volumes. Specifically, in patients with myocardial infarction involving the apex, M-mode measurements, which are obtained at the base of the heart, will underestimate ventricular size and overestimate ventricular function. One geometric model used to calculate left ventricular volumes from on M-mode measurements assumes an elliposoid shape for the left ventricle. It is a common source of error in left ventricular quantification in two-dimensional echocardiography. Accurate assessment of ventricular wall movements during the cardiac cycle is dependent on image quality. Failure to accurately visualize the endocardial border introduces uncertainty into 2D measurements. Ventricular segment scores are assigned based on two qualitative measures of ventricular wall behavior during systole: (1) wall movement (contraction) and (2) wall thickening. A segment that shows noticeable reduction in contractility is hypokinetic and assigned a score of 2. Even with suboptimal imaging (left panel, parasternal short axis view of the left ventricle) tissue harmonic imaging markedly improves endocardial definition. The segmental numerical model can be matched to the more practical anatomical descriptive terminology as shown in. Endocardial border definition deteriorates when still frames are acquired from digital video files. Angulation of the transducer during acquisition of short-axis views may misrepresent true segmental 98 Bulwer et al. A biphasic response on dobutamine stress echocardiography, however, can be a good predictor of improvement in patients scheduled to undergo coronary revascularization procedures. The limitations and assumptions of 2D and M-mode echocardiography are overcome by both real-time and off-line reconstructive 3D echocardiography. Strain-a dimensionless quantity, measures deformation produced by the application of stress. A biphasic response on dobutamine stress echocardiography may be a candidate for coronary artery revascularization procedures. Pressure overload conditions, such as aortic stenosis, severe hypertension, or coarctation, usually lead to hypertrophy, although ventricular dilatation and dysfunction can occur late in the course of disease. Occasionally, hypertrophic cardiomyopathy can ultimately lead to ventricular dilatation and dysfunction (socalled "burnt-out" hypertrophic cardiomyopathy). The use of contrast dates back to 1968 when Gramiak and Shah first used injected saline to enhance the signals from the blood pool. The agent should have strong echogenic interaction in response to incident ultrasound waves. The sonographer is often the first person to recognize the need for contrast, but the physician is ultimately responsible for prescribing its use, which should be done on a case-bycase basis. A registered nurse or physician usually administers the injection or infusion of the contrast agent while the sonographer acquires the images. There are three main patterns of scattering produced by microbubbles, depending on the peak pressure of the incident sound field. This is the principle utilized for enhancing spectral Doppler such as in pulmonary venous flow signals. The concept of "harmonic imaging" emerged from the observation that "nonlinear" oscillations of the microbubbles results in the generation of "second harmonics. To overcome this, "contrast specific" methods are required for assessment of myocardial perfusion by enhancing contrast harmonics while suppressing tissue harmonics. By sending two pulses (one inverted) in rapid succession toward the tissue, summation occurs and results in a strong harmonic signal that is exclusively from the microbubbles. The disadvantage is that wall motion (which produces a Doppler shift), is also detected and this potentially interferes with image quality. The echoes from the bubbles are well separated from those of tissues, thereby providing better characterization of "realtime" myocardial perfusion. Many studies have shown the incremental value of using contrast agents to improve image quality, the percentage of wall segments visualized, and the confidence of interpretation of resting and stress echocardiography images (Chapter 8. Contrast agents in stress echocardiography should be used whenever resting image quality is suboptimal. The use of contrast agents permits almost 90% of initially nondiagnostic images to become diagnostic. Echocardiographic contrast agents that traverse the pulmonary circulation should not be used to diagnose intracardiac shunts. The safety of contrast echocardiography: report of the Committee on Contrast Echocardiography for the American Society of Echocardiography. Myocardial systolic synchrony measured by Doppler tissue imaging as a role of predictor of left ventricular ejection fraction improvement in severe congestive heart failure. Myocardial contrast echocardiography accurately reflects transmurality of myocardial necrosis and predicts contractile reserve after acute myocardial infarction. Current contrast agents have an excellent safety profile, and complications are rare. However, in patients with intracardiac or intrapulmonary right-to-left shunts, the potential for adverse events are slightly greater. Left ventricular dyssynchrony predicts benefit of cardiac resynchronization therapy in patients with end-stage heart failure before pacemaker implantation. Predictors of cardiac events after major vascular surgery: role of clinical characteristics, dobutamine echocardiography, and beta-blocker therapy. Accuracy of dipyridamole myocardial contrast echocardiography for the detection of residual stenosis of the infarct related artery and multivessel disease early after acute myocardial infarction. Correspondence of left ventricular ejection fraction determinations from twodimensional echocardiography, radionuclide angiography and contrast cineangiography. Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study Investigators. Recommendations regarding quantitation in M-mode echocardiography: results of a survey of echocardiographic measurements. American Society of Echocardiography Committee on Standards, Subcommittee on Quantitation of Two-Dimensional Echocardiograms. Improved endocardial visualization with second harmonic imaging compared with fundamental two-dimensional echocardiographic imaging. Problems in echocardiographic volume determinations: echocardiographicangiographic correlations in the presence of absence of asynergy. Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. Right ventricular dysfunction and risk of heart failure and mortality after myocardial infarction. The normal ventricle relaxes quite vigorously leading to rapid pressure decline early in diastole. Physical examination is notable for poorly controlled blood pressure, elevation of central venous pressures, a fourth heart sound and murmur compatible with mitral regurgitation, and mild lower extremity edema. Ventricular stiffness or compliance is another critical determinant of proper diastolic function. The normal ventricle is relatively compliant so that small changes in volume are accompanied by proportionally small changes in pressure. The atria act as reservoir, conduit, and pump during the cardiac cycle, therefore, processes that disrupt normal Chapter 6 / Assessment of Diastolic Function 121. In some instances, intracardiac filling pressures may be normal at rest, but rise precipitously with exercise. Table 2 lists different causes of diastolic dysfunction as well as conditions that may mimic it. Despite these limitations, because transmitral Doppler flow is easy to acquire and well described, characterization of these waveforms remains the basis for categorizing patterns of diastolic function. There are two major components of normal transmitral flow: the rapid early filling phase, designated the E-wave, and filling associated with atrial contraction, designated the A-wave. The limitation of relying on transmitral flow patterns alone for the assessment of diastolic function is that a normal E:Awave ratio can occur in patients with impaired relaxation and elevated filling pressure (right column). Impaired relaxation and increased preload states of diastolic dysfunction are both associated with reduced Ea velocities. Transmitral Doppler flow patterns showing normal filling, impaired relaxation (A-wave > E-wave), pseudonormal filling and restrictive filling (E-wave > A-wave; increased E-wave velocity and shortened E-wave deceleration time). Note the typical S < D pattern in children and young adults and the typical S > D pattern in older adulthood. This is accomplished by bypassing the high pass filter (to pick up strong signal reflections from the myocardium) and using low gain amplification (to eliminate weaker blood flow signals). Abnormal pulmonary venous flow is characterized by blunting of the systolic wave and increased atrial reversal velocity and/or duration. Doppler tissue imaging technique (see Technical Issues in Performing Doppler Tissue Imaging section for explanation). Spectral waveforms from pulse wave tissue Doppler are used to measure peak myocardial velocities. The sample volume is typically placed in the ventricular myocardium immediately adjacent to the mitral annulus to minimize contamination from the translational and rotational motion of the heart and to maximize the longitudinal excursion of the annulus as it descends toward the apex in systole and ascends away from the Chapter 6 / Assessment of Diastolic Function 129. Pulsed wave tissue Doppler imaging spectral waveforms with simultaneous standard Doppler mitral valve inflow. In contrast to standard mitral flow inflow patterns, Ea velocities tend to remain consistently reduced through all phases of diastolic dysfunction. In contrast, Ea velocities in restrictive cardiomyopathy are typically reduced (see Chapter 9. It can be clinically challenging to discriminate the physiologic hypertrophy that results from intense athletic conditioning from pathological hypertrophy. If the Vp slope appears quite blunted, this indicates impaired diastolic function. Assessment of diastolic function by tissue Doppler echocardiography: comparison with standard transmitral and pulmonary venous flow. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. Canadian consensus recommendations for the measurement and reporting of diastolic dysfunction by echocardiography: from the Investigators of Consensus on Diastolic Dysfunction by Echocardiography.

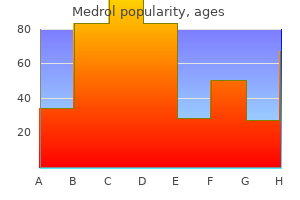
The 95% confidence intervals used in the report are based on the Poisson distribution rheumatoid arthritis essential oils medrol 4mg lowest price. Assignment of Race/Ethnicity the Center follows the recommendation of the National Center for Health Statistics of classifying births according to the self-reported race/ethnicity of the mother arthritis definition medical dictionary purchase 4mg medrol overnight delivery. Race/ethnicity is a selfreported item and is subject to the usual limitations of this type of information rheumatoid arthritis quantitative test buy generic medrol 16 mg online. Plurality the number of births to a woman produced in the same gestational period arthritis in young horses neck discount medrol 4mg without prescription. A singleton is the birth of one infant; twins represent the births of two infants rheumatoid arthritis order medrol 16 mg on-line, etc arthritis pain equate buy cheap medrol 4mg on line. Resident Birth the birth of an infant whose mother reports that her usual place of residence is in Massachusetts. In Massachusetts, a resident is a person with a permanent address in one of the 351 cities or towns. Stillbirth A stillbirth is the birth of a fetus at greater than or equal to 20 weeks gestation, or with a weight of at least 350 grams. Exclude mild or transient hydrocephaly due to intraventricular hemorrhage; ventriculomegaly. Exclude long eyelashes, small palpebal fissures, tear duct cysts, blocked tear ducts; eyelid, lacrimal system and orbit anomalies. Include if >=37 weeks and >=6 wks when last noted or <6 wks if treated with indocin or surgery or associated with other codable defect. Gastrointestinal Biliary Atresia Esophageal Atresia/Tracheoesophageal Fistula Hirschsprung Disease Rectal and Large Intestinal Atresia/Stenosis Small Intestinal Atresia Other Gastrointestinal3 751. Genitourinary Bladder Exstrophy Cloacal Exstrophy Hypospadias, 2nd or 3rd Degree Obstructive Genitourinary Defect3 Renal Agenesis/Hypoplasia Other Genitourinary3 753. Include primary diagnosis with surgical intervention and secondary diagnosis with postnatal confirmation. Exclude deformational plagiocephaly and other abnormal head shape w/o craniosynostosis. Musculoskeletal Clubfoot Craniosynostosis Diaphragmatic Hernia Gastroschisis Omphalocele Polydactyly/Syndactyly Reduction Deformity, Lower Limbs Reduction Deformity, Upper Limbs Skeletal Dysplasia Other Musculoskeletal3 Chromosomal and Other Syndromes Klinefelter Syndrome Trisomy 13 Trisomy 18 Trisomy 21 (Down Syndrome) Turner Syndrome Other Chromosomal Syndromes/Other Syndromes Other Amniotic Bands Skin Anomalies3 Exclude other specified, unspecified congenital anomalies of the integument. Exclude skin tags, urticaria pigmentosa, nevus not elsewhere classified (port wine, nevus flammeus, stork bite), specified anomalies of hair or nails, hypoplastic breast/nipple, absent nipple, small nipple. Exclude hypoplasia and other specified or unspecified anomalies of the adrenal gland. Excludes: megalocornea (use 743220) Eyelids: Coloboma Iris: Coloboma Optic disc: Specified anomalies / hypoplastic optic nerve / coloboma of the optic disc Retina: Specified anomalies / congenital retinal aneurysm. Use 746995 if artery or valve is not specified Pulmonary artery: other specified / pulmonary artery hypoplasia Pulmonary artery: stenosis. Includes: one or more flexion contractures of individual joints Cleidocranial dysostosis Infantile cortical hyperostosis / Caffey syndrome Osteogenesis imperfecta Osteopetrosis / Albers-Schonberg syndrome / marble bones Other specified chondrodystrophy. Excludes: aplasia of or absent lower limb Lower limb: other specified anomalies / hyperextended legs / shortening of legs Other absent or hypoplastic muscle / absent pectoralis major. Excludes: widely spaced first and second toes (use 755600) 754780 Other specified deformity of hands (see 755. Excludes: aplasia or absent upper limb (see 7552) Upper limb: Other specified anomalies / hyperextensibility of upper limb / shortening of upper limb Sacral agenesis Skull and face bone: Other specified anomalies / localized skull defects / mid-facial hypoplasia / prominent maxilla/hypotelorism / flatTocciput / prominent occiput Spine: Kyphosis / kyphoscoliosis Split-Foot, Left Split-Foot, Right Split-Hand, Bilateral Split-Hand, Left Split-Hand, Right Syndactyly: Unspecified, laterality not spec. Excludes: with Turner phenotype (758610) Nail-patella syndrome Other craniofacial syndromes / Hallermann-Streiff syndrome Other specified acrocephalosyndactylies Sex chromosome: Other specified anomaly / fragile X Specified syndromes, not elsewhere classified, involving skin anomalies Treacher-Collins syndrome / Mandibulofacial dysostosis Triploidy Trisomy 13: Patau syndrome Trisomy 13: translocation trisomy with duplication of a 13q Trisomy 18: Edwards syndrome Trisomy 18: Translocation trisomy with duplication of 18q Trisomy, partial / 8/02 "partial trisomy" = "duplication". Syndromes/limbs: Baller-Gerold/ Carpenter / caudal regression /Fryns/ Holt-Oram / Klippel-Trenaunay-Webe/ LimbBodyWall 759840 /Roberts/ Rubinstein-Taybi / sirenomelia / thrombocytopenia-absent radius Malf. Syndromes/metabolic: Alagille /Alport / Beckwith-Wiedemann / Johansen-Blizzard/ leprechaunism / Lowe/ Menkes(kinky hair) /Prader-Willi/ Zellweger 759870 Malf. For specified anomalies of nails 757580 Spleen: Absence / asplenia Spleen: Accessory / 8/02 Use for polysplenia, though not exactly the same Spleen: Hypoplasia Thyroglossal duct anomalies / thyroglossal cyst 757340 757330 757190 658800 759240 757800 759000 759040 759010 759220 1 2 1 10 3 3 3 4 1 2 110 Glossary of Selected Birth Defects Terms1 Agenesis, aplasia: Congenital absence of a body part or organ, implying that the structure never formed. Agenesis corpus callosum: Congenital absence of the part of the brain which connects the two cerebral hemispheres. Amniotic band sequence: Highly variable group of defects (or single defect) due to encirclement (strangulation) of a body part by strands of a fragmented amniotic sac. Anophthalmia: Congenital complete (or essentially complete) absence of the eye globe. Aortic valve stenosis: Congenital heart defect characterized by aortic valve narrowing reducing the flow of blood. Atresia / Imperforation: Congenital absence or closure of a normal opening (valve or lumen). Atresia or stenosis of large intestine, rectum and anus: Congenital absence, closure or constriction of the large intestine, rectum or anus (commonly known as imperforate anus). Atresia or stenosis of small intestine: Congenital absence, closure or constriction of the small intestine (duodenal, jejunal, ileal atresia/stenosis). Birth defect: Congenital abnormalities of structure, function or metabolism present before birth. Bladder exstrophy: Congenital exposure of the bladder mucosa caused by incomplete closure of the anterior bladder wall and the abdominal cavity. Branchial cleft, fistula, tag, cyst: Congenital abnormality of the neck or area just below the collarbone (clavicle). Choanal atresia, choanal stenosis: Congenital absence (or narrowing) of the passageway between the nose and pharynx due to a thick bone or thin "membranous" bone. Cleft lip: Congenital defect of the upper lip in which there is incomplete closure. Cleft palate: Congenital defect in the closure of the palate; the structure which separates the nasal cavities and the back of the mouth. Coarctation of the aorta: Congenital heart defect characterized by narrowing of the descending aorta. Usually occurs as an indentation at a specific location, less commonly diffuse narrowing. Includes defects detected prenatally and those not recognized until after the newborn period. Includes defects detected prenatally, and those recognized after the newborn period. Craniosynostosis: Congenital abnormality of skull shape due to premature fusion of the sutures between the skull bones. Dandy-Walker malformation: Congenital defect of the cerebellum involving a small cerebellar vermis and cystic dilation of the fourth ventricle. Diaphragmatic hernia: Congenital defect of the muscular diaphragm resulting in herniation of the abdominal contents into the chest. Down syndrome (Trisomy 21): Distinctive and common chromosome abnormality syndrome caused by an extra copy of chromosome 21. Can be complete (Trisomy 21), attached to another chromosome (translocation), or mixed with cells containing normal chromosomes (mosaic). Ebstein anomaly: Congenital heart defect characterized by downward displacement of the tricuspid valve into the right ventricle, associated with tricuspid valve regurgitation. Encephalocele: Congenital defect of the skull resulting in herniation (protrusion) of the brain. Fistula: Abnormal connection between an internal organ and the body surface, or between two internal organs or structures. Gastroschisis: Congenital opening of the abdominal wall with protrusion of the abdominal contents. Can be distinguished from omphalocele by location usually to the right of the umbilicus. Heterotaxy (situs anomalies): Congenital malposition of the abdominal organs often associated with a congenital heart defect. Hirschsprung disease: Congenital aganglionic megacolon (enlarged colon) due to absent nerves in the wall of the colon. Holoprosencephaly: Spectrum of congenital defects of the forebrain due to failure of the brain to develop into two equal halves. Hydronephrosis: Enlargement of the urine-filled chambers (pelves, calyces) of the kidney Hyperplasia: Overgrowth due to an increase in the number of cells of tissue. Classically, aortic valve/mitral valve atresia or marked hypoplasia, ascending aorta and left ventricle hypoplasia. Limb deficiency, upper (arms) / lower (legs): Congenital absence of a portion or entire limb. Types include transverse (resembling an amputation), longitudinal (missing ray) and intercalary (missing bone in-between). Microtia: Congenital smallness or maldevelopment of the external ear, with or without absence or narrowing of the external auditory canal. Omphalocele: Congenital opening of the abdominal wall with protrusion of the abdominal contents. Polydactyly: Extra fingers or toes which may be medial (pre-axial) or lateral (postaxial). Pulmonary atresia: Congenital heart defect characterized by absence of the pulmonary valve or pulmonary artery itself. Spina bifida: Neural tube defect with protrusion of the spinal cord and/or meninges. Includes myelomeningocele (involving both spinal cord and meninges) and meningocele (involving just the meninges). Stenosis: Narrowing or constriction of the diameter of a bodily passage or orifice. Translocation: Chromosome rearrangement in which a piece of genetic material is transferred from one segment to another. May be balanced (no chromosome material gained or lost), or unbalanced (material has been gained or lost). Tricuspid atresia: Congenital heart defect characterized by the absence of the tricuspid valve. Truncus arteriosus: Congenital heart defect characterized by a single great arterial trunk, instead of a separate aorta and pulmonary artery. Improved National Prevalence Estimates for 18 Selected Major Birth Defects-United States, 1999-2001. Spina Bifida and Anencephaly Before and After Folic Acid Mandate- United States, 1995-1996 and 1999-2000. Impact of prenatal diagnosis and elective termination on the prevalence of selected birth defects in Hawaii. Bureau of Health Statistics, Research and Evaluation, Bureau of Family Health and Nutrition, Massachusetts Department of Public Health. Trends in Congenital Malformations, 1974-1999: effect of prenatal diagnosis and elective termination. Teratology and the epidemiology of birth defects: Occupational and environmental perspectives. Impact of including induced pregnancy terminations before 20 weeks gestation on birth defect rates. An L-looped right ventricle is "left handed" because the left hand will fit in the right ventricle. The connecting segments and ventriculo-arterial connections are described separately. If the right atrium connects to the right ventricle, and the left atrium connects to the left ventricle, this is described as atrioventricular concordance. Femoral pulses should be part of every exam, particularly in neonates o Assess distal perfusion by the warmth of the digits and capillary refill time. Assume the oxygen consumption is 150mL/min and pulmonary venous saturations are 100%. Assume the oxygen consumption is 120mL/min/m2 and pulmonary venous saturations are 100%. Nontraumatic chest pain in children and adolescents: Approach and initial management. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents, National Heart, Lung, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. There is usually a bimodal distribution, with peaks in the <1 year period, and again during adolescence. His breathing is unlabored, there is no hepatomegaly or splenomegaly, and the distal pulses are excellent. A 4 week old, ex-term infant ate well and gained weight for the first 3 weeks of life. His mother reports that for the last week, he appears hungry, but fatigues with feeds and he now takes twice as long to complete a feeding as he did 1 week ago. Chapter 5: Initial Evaluation of the Newborn with Suspected Cardiovascular Disease; p. The increased oxygen content of blood flowing through the ductus promotes vasoconstriction of the smooth muscle and closure of the ductus. This leads to a spectrum of tricuspid valve regurgitation and a dysfunctional, "atrialized" right ventricle. Next most common is fusion of right and noncoronary cusp o this type has higher incidence of aortic valvar stenosis and/or regurgitation. The pulmonary valve now acts as the aortic valve and is called the "neo-aortic valve.
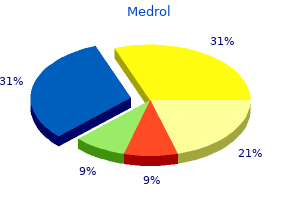
Tympanic membrane perforation resulting in deafness which may complicate the evaluation of their mental status and their ability to follow commands 6 arthritis in neck what to do generic 4mg medrol with amex. Primary transport to a trauma or burn center is preferable arthritis in feet x ray generic medrol 4 mg on line, whenever possible Pertinent Assessment Findings 1 rheumatoid arthritis markers purchase medrol 16 mg free shipping. Revision Date September 8 rheumatoid arthritis toes buy generic medrol 16mg online, 2017 193 Burns Aliases None noted Patient Care Goals Minimize tissue damage and patient morbidity from burns Patient Presentation 1 arthritis mayo clinic order medrol 16 mg mastercard. Transport to most appropriate trauma center when there is airway or respiratory involvement rheumatoid arthritis lung disease purchase medrol 16 mg amex, or when significant trauma or blast injury is suspected 2. Consider air ambulance transportation for long transport times or airway management needs beyond the scope of the responding ground medic 3. Proper protective attire including breathing apparatus may be required Patient Management Assessment 1. High flow supplemental oxygen for all burn patients rescued from an enclosed space 5. For pediatric patients weighing less than 40 kg, use length-based tape for weight estimate and follow c. For persons over 40 kg, the initial fluid rate can also be calculated using the "Rule of 10": i. Prevent systemic heat loss and keep the patient warm Special Treatment Considerations 1. Airway burns can rapidly lead to upper airway obstruction and respiratory failure 3. Particularly in enclosed-space fires, carbon monoxide toxicity is a consideration and pulse oximetry may not be accurate [see Carbon Monoxide Poisoning guideline] 5. For specific chemical exposures (cyanide, hydrofluoric acid, other acids and alkali) [see Topical Chemical Burn guideline] 6. Consider decontamination and notification of receiving facility of potentially contaminated patient. Onset of stridor and change in voice are sentinel signs of potentially significant airway burns, which may rapidly lead to airway obstruction or respiratory failure 2. Simple derivation of the initial fluid rate for the resuscitation of severely burned adult combat casualties: in Silico validation of the rule of ten. Revision Date September 8, 2017 197 Crush Injury Aliases Crush, compartment syndrome Patient Care Goals 1. Minimize systemic effects of the crush syndrome Patient Presentation Inclusion criteria Traumatic crush mechanism of injury Exclusion criteria Non-crush injuries Patient Management Assessment 1. The treatment of crushed casualties should begin as soon as they are discovered 2. If severe hemorrhage is present, see Extremity Trauma/External Hemorrhage Management guideline 3. Intravenous access should be established with normal saline initial bolus of 10-15 ml/kg (prior to extrication if possible) 5. Carefully monitor for dysrhythmias or signs of hypokalemia before and immediately after release of pressure and during transport. Continued resuscitation with normal saline (500-1000 cc/hr for adults, 10 cc/kg/hr for children) b. Rapid extrication and evacuation to a definitive care facility (trauma center preferred) 2. A patient with a crush injury may initially present with very few signs and symptoms Therefore, maintain a high index of suspicion for any patient with a compressive mechanism of injury 3. Continue fluid resuscitation through extrication and transfer to hospital Pertinent Assessment Findings 1. Evaluation for fractures and potential compartment syndrome development (neurovascular status of injured extremity) 3. Revision Date September 8, 2017 200 Extremity Trauma/External Hemorrhage Management Aliases None noted Patient Care Goals 1. Minimize pain and further injury as a result of potential fractures or dislocations Patient Presentation Inclusion Criteria 1. Potential extremity fractures or dislocations Exclusion Criteria No recommendations Patient Management Assessment 1. Degree of bleeding/blood loss with assessment of the color of the blood (venous or arterial) and whether it is pulsatile or not Treatments and Interventions (also, see protocol diagram below) 1. If the bleeding site is amenable to tourniquet placement, apply tourniquet to extremity 1. Tourniquet should be placed 2-3 cm proximal to wound, not over a joint, and tightened until bleeding stops and distal pulse is eliminated. For thigh wounds, consider placement of two tourniquets, side-byside, and tighten sequentially to eliminate distal pulse ii. If still bleeding, pack wound tightly with hemostatic gauze and apply direct pressure iii. Pain management should be strongly considered for patients with suspected fractures b. If tourniquet placed, an alert patient will likely require pain medication to manage tourniquet pain 3. Strongly consider pain management before attempting to move a suspected fracture b. If distal vascular function is compromised, gently attempt to restore normal anatomic position c. Elevate extremity fractures above heart level whenever possible to limit swelling. Apply ice/cool packs to limit swelling in suspected fractures or soft tissue injury - do not apply ice directly to skin f. Reassess distal neurovascular status after any manipulation or splinting of fractures/dislocations Patient Safety Considerations 1. Ensure that it is sufficiently tight to occlude the distal pulse, in order to avoid compartment syndrome b. Ensure that it is well marked and visible and that all subsequent providers are aware of the presence of the tourniquet c. If pressure dressing or tourniquet used, frequently re-check to determine if bleeding has restarted. Check for blood soaking through the dressing or continued bleeding distal to the tourniquet. Do not remove tourniquet or dressing in order to assess bleeding Notes/Educational Pearls Key Considerations 1. If tourniquet is replaced with pressure dressing, leave loose tourniquet in place so it may be retightened if bleeding resumes 3. Commercial/properly tested tourniquets are preferred over improvised tourniquets 5. If hemostatic gauze is not available, plain gauze tightly packed into a wound has been shown to be effective 202 6. Amputated body parts should be transported with patient for possible re-implantation a. Recognizing that pain is undertreated in injured patients, it is important to assess whether a patient is experiencing pain o Trauma-04: Trauma patients transported to trauma center. An evidence-based prehospital guideline for external hemorrhage control: American College of Surgeons Committee on Trauma. Prehospital control of life-threatening truncal and junctional haemorrhage is the ultimate challenge in optimizing trauma care: a review of treatment options and their applicability in the civilian trauma setting. A multi-institutional study of hemostatic gauze and tourniquets in rural civilian trauma. A systematic review of the use of tourniquets and topical haemostatic agents in conflicts in Afghantistan and Iraq. Advanced hemostatic dressings are not superior to gauze for care under fire scenarios. Revision Date September 8, 2017 205 Facial/Dental Trauma Aliases None noted Patient Care Goals 1. Preservation of dentition Patient Presentation Inclusion Criteria Isolated facial injury, including trauma to the eyes, nose, ears, midface, mandible, dentition Exclusion Criteria 1. Stable dentition (poorly anchored teeth require vigilance for possible aspiration) 3. Mental status assessment for possible traumatic brain injury [see Head Injury guideline] 6. Specific re-examination geared toward airway and ability to ventilate adequately Treatment and Interventions 1. Alternatively, an alert and cooperative patient can hold tooth in mouth using own saliva as storage medium 5. Expect patient cannot spit/swallow effectively and have suction readily available b. Preferentially transport sitting up with emesis basin/suction available (in the absence of a suspected spinal injury, see Spinal Care guideline) 7. Epistaxis - squeeze nose (or have patient do so) for 10-15 minutes continuously 8. Transport with tissue wrapped in dry sterile gauze in a plastic bag placed on ice c. Severe ear and nose lacerations can be addressed with a protective moist sterile dressing Patient Safety Considerations 1. Maintenance of a patent airway is the highest priority; therefore, conduct cervical spine assessment for field clearance (per Spinal Care guideline) to enable transport sitting up for difficulty with bleeding, swallowing, or handling secretions Notes/Educational Pearls Key Considerations 1. After nasal fractures, epistaxis may be posterior and may not respond to direct pressure over the nares with bleeding running down posterior pharynx, potentially compromising airway 3. Avulsed teeth may be successfully re-implanted if done so in a very short period after injury b. Revision Date September 8, 2017 208 Head Injury Aliases None noted Patient Care Goals 1. Administer oxygen as appropriate with a target of achieving 94-98% saturation 209 2. If patient unable to maintain airway, consider oral airway (nasal airway should not be used with significant facial injury or possible basilar skull fracture) c. Assume concomitant cervical spine injury in patients with moderate/severe head injury 3. Geriatric Consideration: Elderly patients with ankylosing spondylitis or severe kyphosis should be padded and immobilized in a position of comfort and may not tolerate a cervical collar Notes/Educational Pearls Key Considerations 1. If endotracheal intubation or invasive airways are used, continuous waveform capnography is required to document proper tube placement and assure proper ventilation rate 4. Prognostic factors in civilian gunshot wounds to the head: a series of 110 surgical patients and brief literature review. Influence of prehospital treatment on the outcome of patients with severe blunt traumatic brain injury: a single-centre study. The relationship between out-of-hospital airway management and outcome among trauma patients with Glasgow Coma Scale scores of 8 or less. Inappropriate prehospital ventilation in severe traumatic brain injury increases in-hospital mortality. Effect of secondary prehospital risk factors on outcome in severe traumatic brain injury in the context of fast access to trauma care. Prehospital intravenous fluid administration is associated with higher mortality in trauma patients: a National Trauma Data Bank analysis. Clinical policy: neuroimaging and decision making in adult mild traumatic brain injury in the acute setting. Part 14: pediatric advanced life support: 2010 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Adult Trauma Clinical Practice Guidelines: Initial Management of Closed Head Injury in Adults: 2nd Edition. Warm Zone/Indirect Threat Zone: an area within the inner perimeter where security and safety measures are in place. Prioritization for extraction is based on resources available and the situation. Encourage patients to provide self-first aid or instruct aid from uninjured bystander g. Tourniquet application is the primary "medical" intervention to be considered in Hot Zone/Direct Threat ii. Consider instructing patient to apply direct pressure to the wound if no tourniquet available (or application is not feasible) iii. Consider quickly placing or directing patient to be placed in position to protect airway, if not immediately moving patient 2. Ensure safety of both responders and patients by rendering equipment and environment safe (firearms, vehicle ignition) c. Conduct primary survey, per the General Trauma Management guideline, and initiate appropriate life-saving interventions i. Do not delay patient extraction and evacuation for non-life-saving interventions. Consider establishing a casualty collection point if multiple patients are encountered f.
Discount medrol 16 mg mastercard. RA Flares: What Triggers a Rheumatoid Arthritis Flare?.
References