





|
STUDENT DIGITAL NEWSLETTER ALAGAPPA INSTITUTIONS |

|
Victor Mor-Avi, PhD
Atlantoaxial subluxation (C1 on C2) can be seen radiographically in up to 30% of cases medications xyzal 20mg celexa sale. Spinal cord compression with neurologic manifestations occurs infrequently Figure 286-6 Arthrogram with a radiocontrast agent injected into the knee treatment 5cm ovarian cyst cheap celexa 20 mg overnight delivery. The body of C2 and its odontoid process are outlined by broken lines 714x treatment buy cheap celexa 40mg on line, and the posterior aspect of the anterior segment of C1 is indicated by a solid line medications an 627 purchase celexa 20 mg on-line. The space between C1 and the odontoid of C2 is markedly increased medicine 4212 buy 20 mg celexa fast delivery, indicative of subluxation of C1 on C2 medications to avoid during pregnancy buy 10 mg celexa. At a lower level, C3 is also displaced anteriorly because of rheumatoid erosion of articular and ligamentous structures. Occipital and/or frontal headache is a common premonitory sign of weakness in the extremities, bladder or bowel incontinence, or frank quadriplegia. Vertebral arteries may also be compressed and lead to vertebrobasilar insufficiency with vertigo or syncope, especially on downward gaze. Proliferative synovitis in the elbow often causes flexion contractures, even early in the disease. Supination of the hand may be impaired, especially if shoulder motion is concomitantly decreased. Limited motion and tenderness just below and lateral to the coracoid process are typical symptoms. Noticeable swelling is rare; however, large synovial cysts may occur (see Color Plate 3 D). Joint destruction usually involves rupture of the joint capsule and subluxation of the humerus. Pain in the groin, lateral aspect of the buttock, or lower part of the back may indicate hip involvement. Because the hip joint capsule has poor distensibility, severe pain can result if a large effusion occurs. Arthrocentesis should be done to relieve pain and exclude infection in such cases. Rarely, extreme hip destruction results in protrusion of the femur into the pelvis. Synovitis of the cricoarytenoid joints may result in dysphagia, hoarseness, or anterior neck pain. Prompt administration of intra-articular or parenteral corticosteroids and/or tracheostomy may be necessary. All the extra-articular complications occur almost exclusively in seropositive patients. They occur most commonly in periarticular structures and areas subject to pressure, such as the elbows, extensor and flexor tendons of the hands and feet, Achilles tendons, and less commonly, the occipital and sacral areas. Palmar erythema and fragility of the skin resulting in easy bruising are common manifestations. The 1st is manifested by small, splinter-shaped brown infarcts in the nail folds and digital pulp, often also present over subcutaneous nodules (see Color Plate 3 E). Histologic examination may reveal leukocytoclastic vasculitis or a mild venulitis. This process is benign in most patients and does not indicate serious systemic vasculitis. The 2nd form is a severe necrotizing vasculitis of small and medium arteries indistinguishable from periarteritis nodosa. Digital infarcts, mononeuritis multiplex, fever, and other manifestations of systemic disease should prompt aggressive therapy. Evidence of pericardial involvement with old fibrinous lesions is found in approximately 40% of patients at autopsy. Constrictive pericarditis is somewhat more common and is typically manifested as dyspnea, right-sided heart failure, and peripheral edema. Pericardial fluid characteristics include a low glucose concentration, increased level of lactate dehydrogenase, elevated immunoglobulin levels, and low complement activity. Rheumatoid nodules may occasionally develop in the myocardium or heart valves, and vasculitis may involve the coronary arteries. Conduction abnormalities, valvular incompetence or stenosis, and myocardial infarction are all rare clinical sequelae of rheumatoid heart disease. Rheumatoid pleural disease, although frequently found at autopsy, is most commonly asymptomatic. Typically the pleural fluid is exudative, and white cell counts vary greatly but are generally less than 5000 per microliter. Although usually asymptomatic, they may become infected and cavitate or rupture into the pleural space and produce a pneumothorax. Finally, a diffuse interstitial fibrosis with pneumonitis may progress to a honeycomb appearance on the radiograph, bronchiectasis, chronic cough, and progressive dyspnea. Pulmonary function tests show diminished compliance and a restrictive ventilatory pattern. An irreversible combination of Figure 286-8 Chest radiograph demonstrating discrete rheumatoid nodules in both the right and left lower lobes of the lungs. Peripheral neuropathies can be produced by proliferating synovium causing compression of nerves. Carpal tunnel syndrome (median neuropathy) (see under Articular Manifestations) is common, and a similar entrapment of the anterior tibial nerve (tarsal tunnel syndrome) can result in paresthesias with footdrop. Rheumatoid vasculitis may cause a mononeuritis multiplex condition with patchy sensory loss in one or more extremities, often in association with wristdrop or footdrop. Cervical myelopathy can result from atlantoaxial subluxation (see under Articular Manifestations). The central nervous system is usually spared, although cerebral vasculitis and rheumatoid nodules in the meninges have been described. Episcleritis is a self-limited condition associated with redness of the eye and only mild pain. If this condition progresses to thinning of the tissue allowing the dark blue color of the choroid below to show through, it is termed "scleromalacia perforans. The syndrome typically appears late in the course of a seropositive, destructive arthritis, often after joint disease is believed to be "burnt out. Hypersplenism and immune-mediated destruction of white blood cells are believed to cause the neutropenia. Splenectomy may correct the neutropenia and prevent further infections in some patients, but many do not improve. Splenectomy should not be performed for this disorder because it may hasten the onset of malignancy. A chronic normocytic, normochromic anemia with hematocrit values from 30 to 35% is usual. The anemia does not respond to administration of iron, but erythropoietin may be effective when the anemia is severe. The white blood cell count and differential are typically normal, but eosinophilia may occur in severe systemic disease. The erythrocyte sedimentation rate is elevated in most patients but only roughly parallels disease activity. The presence of rheumatoid factor is detected in more than 80% of cases and is useful in clinical diagnosis. Antinuclear antibodies detected by immunofluorescence, usually in low titer, can be found in 30 to 40% of cases. Synovial fluid analysis usually shows a poor mucin clot test and white cell counts in the range of 5000 to 20,000 per cubic millimeter, with 50 to 70% as polymorphonuclear leukocytes (Table 286-4). The synovial fluid glucose concentration is usually normal, but very low values occur occasionally, even in the absence of a superimposed infectious arthritis. Approximately 20% of patients will improve spontaneously or even achieve remission, especially in the 1st year of disease; however, chronic disease progression and functional deterioration occur in the majority. A higher mortality rate also correlates with the degree of disability and results from infections, systemic manifestations, and gastrointestinal bleeding or perforation. Objectives of management include (1) relief of pain and stiffness, (2) reduction of inflammation, (3) minimization of undesirable drug side effects, (4) preservation of muscle strength and joint function, and (5) maintenance of as normal a lifestyle as possible. The basic initial program that achieves these objectives for the great majority of patients consists of (1) adequate rest, (2) adequate anti-inflammatory therapy, and (3) physical measures to maintain joint function. An additional objective, (6) to attempt to modify the disease course with early, aggressive drug therapies, has recently been advocated because of prognosis studies and the findings that rheumatoid pannus invades and irreversibly damages articular cartilage within 1 to 2 years of disease onset. Moreover, it is unclear that the current armamentarium of disease-modifying drugs can achieve this goal. Any confusion arising from the complementary requirements of rest and exercise should be promptly dispelled. Bed rest tends to decrease the general systemic inflammatory response, and most patients soon learn that their midafternoon fatigue is significantly reduced by a period of rest. During acute attacks, longer rest periods and perhaps even remaining in bed for the duration of the attack may be required to treat the inflammation. At the same time, full range of joint motion should be maintained, which can usually be accomplished by the patient through graded exercise programs. However, during acute attacks, passive range-of-motion exercises by a physical therapist or instructed layperson may be indicated. Exercise, as well as heat treatments such as showers, baths, warm pools, paraffin baths, or hot packs, should be used to loosen the joints and relieve stiffness. Exercise following the heat treatment maintains the motion of affected joints and prevents muscle atrophy. The patient needs to understand that a larger dose is required than would be used for analgesia alone. A constant blood level of 20 to 30 mg/dL is needed, which for most patients requires between 3 and 6 g of aspirin per day. All patients should be monitored for toxic levels by blood tests and should be alerted to report deafness, ringing in the ears, or gastrointestinal intolerance. With the availability of buffered and coated aspirin, a suitable salicylate preparation can be found for almost any patient. Clinical experience suggests an occasional need to change from one to another of these drugs to minimize side effects and to give maximal symptomatic benefit to individual patients. Overt gastrointestinal tract hemorrhage or ulceration is infrequent, but when it occurs it dictates discontinuation of the drug. Because of its side effects, long-term corticosteroid therapy should be reserved for patients with unresponsive and aggressive joint disease whose ability to function is threatened. Higher doses are necessary for patients with neuropathy, vasculitis, pleuritis, pericarditis, scleritis, and related conditions. The more slowly acting drugs include antimalarials, methotrexate, gold, penicillamine, sulfasalazine, and minocycline. Antimalarials are usually given as hydroxychloroquine (Plaquenil), 200 mg once or twice daily. This drug, or chloroquine, may cause retinal lesions and loss of vision; therefore, the patient should be examined by an ophthalmologist at least twice a year. Side effects include hepatotoxicity and possibly cirrhosis, bone marrow suppression, oral ulcers, and a potential life-threatening pneumonitis. Methotrexate may also cause a leukocytoclastic vasculitis and may promote the formation of rheumatoid nodules, including systemic nodulosis. Concomitant treatment with folic acid, 1 mg/day, reduces toxicity from methotrexate without impairing efficacy. The drug given with an oral loading dose of 100 mg for each of 3 days, followed by 20 mg daily thereafter, has shown considerable efficacy and little toxicity, although liver function tests require regular monitoring. Sulfasalazine given in a dose of 2 to 3 g daily may be effective in some patients. Gold salts, especially weekly intramuscular injections, produce remission in many cases. An oral gold salt, auranofin, appears to be therapeutically effective and to have less toxicity than do intramuscular injections. Severe manifestations include bone marrow suppression, usually leukopenia or thrombocytopenia, renal damage with proteinuria, and rarely a nephrotic syndrome. Therefore, frequent urinalysis and blood counts must be performed, especially during the early phases of treatment. Penicillamine is also effective in inducing improvements and sometimes even remissions. Like gold, however, its effects are slow in coming, and it may affect both the bone marrow and the kidneys, so careful monitoring for toxicity is required. Short-term clinical trials have shown it to be quickly, highly effective in a majority of patients. Other disadvantages include high cost and need for bi-weekly subcutaneous injections. The likelihood of serious side effects is significantly increased, however, and close consultation with a rheumatologist is strongly recommended. Prosthetic devices for hip and knee joints have given excellent results, and devices for ankle, elbow, and shoulder replacement are improving. A chronic arthritis beginning in childhood and for which no underlying cause is apparent has been termed juvenile rheumatoid arthritis. Several subgroups of juvenile chronic arthritis are recognized on the basis of modes of onset, other clinical features, and immunogenetic differences. Clinical characteristics include high, spiking daily fevers; an evanescent, salmon-colored rash usually appearing with fever; lymphadenopathy; hepatosplenomegaly; polyserositis; leukocytosis; thrombocytosis; and anemia. Although the disease is rarely life threatening, it can be confused with leukemia or infection. Disease with a pauciarticular onset accounts for the remaining 40% of patients with juvenile chronic arthritis. The serum is usually positive for antinuclear antibodies but not rheumatoid factor. Patients in this subgroup are at risk for chronic iridocyclitis, which may progress to blindness.
Patients may present with claudication of the foot medications 101 buy 20 mg celexa with visa, legs symptoms 6 days post embryo transfer buy 40mg celexa amex, and occasionally the arms and hands treatment 4 water buy celexa 40 mg on line. Foot or arch claudication may be the presenting manifestation and is often mistaken for an orthopedic problem symptoms vaginitis order 20 mg celexa overnight delivery. Two or more limbs are almost always involved medicine abbreviations order celexa 10mg without a prescription, and angiographic abnormalities are consistently found in limbs that are not yet clinically involved medications or therapy buy cheap celexa 40 mg on-line. In this test, the physician simultaneously occludes both the radial and ulnar arteries. When pressure is released from either artery, there should be prompt filling from that artery with the return of color to the hand. A positive test result is indicated when color does not return to the blanched hand. On arteriography, the proximal arteries are normal, and the disease is most often infrapopliteal in the lower extremities and distal to the brachial artery in the upper extremities. However, these other diseases can usually be established or excluded by other tests. The cornerstone of therapy for thromboangiitis obliterans is the complete discontinuation of cigarette smoking or the use of tobacco in any form. Quitters will almost always avoid amputations, whereas 40% or more of patients who continue tobacco use will progress to one or more amputations. All other forms of therapy (calcium channel blockers, antibiotics, anticoagulants, sympathectomy) are palliative. In a prospective, randomized trial, intravenous iloprost was superior to aspirin at 28 days in relieving rest pain and healing of all trophic change. At 6 months, 88% of patients receiving iloprost responded to therapy, compared with 21% in the aspirin group, and only 6% underwent amputation in the iloprost group, compared with 18% in the aspirin group. In a recently reported double-blind, placebo-controlled, randomized trial, oral iloprost was slightly more effective than placebo in relieving rest pain but not in healing ischemic ulcerations. Surgical bypass is not a viable option in most patients because there may not be a distal target vessel with which to bypass. These patients have small vessel occlusive disease that may lead to digital pitting or ulceration and eventual amputation. Continued use of vibratory tools can lead to a chronic occlusive small vessel vascular disease. Trauma to the distal ulnar artery (several centimeters distal to the wrist) may occur with activities such as pounding with the palm of the hand, karate, or other activities that traumatize the hypothenar eminence and lead to an aneurysm or pseudoaneurysm of the distal ulnar artery. Thrombus within the aneurysm may then embolize to the fingers, or the distal ulnar artery may thrombose. At this point there is total cessation of blood flow and the digits are often numb. As the arterial vasoconstriction becomes less severe, postcapillary venule constriction causes the blood in the capillaries and veins to become deoxygenated, thus producing the cyanotic appearance. When rewarming occurs, there is a markedly increased blood flow producing reactive hyperemia to the digits (red color). Exposure to the cold is the typical precipitating factor, but emotional lability may also cause or exacerbate attacks in some patients. Vasospastic attacks usually occur only in the fingers, but vasospasm can occur in the toes, nose, ears, lips, and other body parts. An abnormal result of the Allen test on physical examination indicates fixed arterial obstruction. The non-invasive vascular laboratory (pulse volume recordings) is useful in identifying the degree of digital arterial occlusive disease (fixed ischemia) and predicting whether ischemic ulcerations on the digits will heal. In patients with mild vasospastic attacks, reassurance about the benign nature of the disease and instructions on how to prevent attacks are often all that is needed. Patients should limit the amount of exposure to the cold and should dress warmly and protect not only their extremities but also their entire body. Conditioning techniques or biofeedback are sometimes helpful in controlling vasospastic episodes. When vasospasm occurs more frequently, the extended-release preparations of nifedipine (30-90 mg daily), amlodipine (2. The alpha1 -adrenergic receptor antagonists such as prasozin or terazosin can also decrease the severity, frequency, and duration of vasospastic attacks in patients. Nitroglycerin can be used topically in patients, whereas prostacyclin can be given intravenously. The angiotensin-converting enzyme inhibitor captopril has shown some benefit in uncontrolled trials, but other vasodilators such as niacin and papavarine are not beneficial. Although sympathectomy may be beneficial in the short term, with about a 50% improvement rate, the vasospastic attacks may recur after a period of 6 months to 2 years. Pernio (Chilblains) Pernio (a Latin word that literally means frostbite; however, its synonym chilblains is an Anglo-Saxon term that means cold sore) are localized inflammatory lesions of the skin as a result of abnormal response to the cold. Pernio is now less common but is still seen in the temperate, humid climates of northwestern Europe and in the northern United States. The pathologic changes include edema of the papillodermis, vasculitis characterized by perivascular infiltration (with lymphocytes) of the arterioles and venules of the dermis, thickening and edema of the blood vessel walls, fat necrosis, and chronic inflammatory reaction with giant cell formation. Pernio most commonly occurs in young women between the ages of 15 and 30 but may occur in older individuals or in children. Single or multiple erythematous, purplish, edematous lesions appear accompanied by intense itching or burning. These lesions may have a yellowish or brownish discoloration and may be associated with some flaking. The lesions of acute pernio are usually self-limited, although they may lead to recurrent disease. The arterial circulation is normal on physical examination and in the non-invasive vascular laboratory. Characteristically, the lesions begin in the fall or winter and disappear in the spring or early summer. In advanced cases, the seasonal variation may disappear and chronic occlusive vascular disease may develop. In the typical form, the patient develops violet or yellow-brown blisters and shallow ulcers on the toes that burn and itch. The differential diagnosis of pernio includes recurrent, erythematous, nodular, and ulcerative lesions such as erythema induratum, nodular vasculitis, erythema nodosum, and cold panniculitis. The skin lesions of pernio may look similar to atheromatous embolization (see earlier), and an arteriogram may sometimes be required. In a randomized trial, nifedipine reduced the pain and facilitated the healing process. The severe itching may be treated with a local application of an antipruritic agent. Acrocyanosis Acrocyanosis, which is a persistent blue or cyanotic discoloration of the digits, occurs most commonly in the hands and may worsen with exposure to cold and improve with rewarming. The primary form is a benign cosmetic condition, but it may also be seen in patients with connective tissue diseases, thromboangiitis obliterans, and diseases associated with central cyanosis. The exact pathophysiologic abnormality is not clear but may be vasospasm in the cutaneous arteries and arterioles with compensatory dilatation in the postcapillary venules. Drugs such as alpha-adrenergic blocking agents or calcium channel blockers may be helpful. It may occur in above-freezing temperatures under circumstances such as wetness, strong wind, or high altitude. Heat loss is reduced by peripheral vasoconstriction caused by sympathetic stimulation and catecholamine release. Maintenance or augmentation of body heat is accomplished by muscular activity such as shivering. However, the heat production from shivering cannot be sustained for more than a few hours because of the depletion of glycogen, which is the source of heat during shivering. The extremities are also protected by the "hunting reaction," which consists of irregular, 5- to 10-minute cycles of alternating periods of vasoconstriction and vasodilatation that protect the extremities against excessive sustained vasoconstriction at minimal loss of internal body temperature. However, when the body is exposed to cold of a magnitude or duration so as to threaten the internal body temperature, this mechanism fails. Because the disruption of core temperature is more deleterious to the body than peripheral vasoconstriction, conservation of core temperature takes precedence over rewarming of the extremities, and the hunting response is replaced by continuous and more intense vasoconstriction that promotes frostbite by means of ice crystal formation, cellular dehydration, and thrombosis of the microvasculature. Soon after exposure to the cold, pain develops and gradually progresses to numbness; the frozen part turns white because of intense vasoconstriction. With rewarming or thawing, the circulation is restored and the affected parts become hyperemic. Blisters appear within the first 24 hours and are reabsorbed within 1 to 2 weeks, after which a black eschar may persist. Overactivity of the sympathetic nervous system is manifested by hyperhidrosis or a burning sensation. Seventy per cent of victims develop chronic sequelae including cold sensitivity, pain, and sensory disturbances, often resembling a reflex sympathetic dystrophy. It is important to establish the depth of the frostbite and determine if the tissue is viable, which may not be obvious on initial clinical examination but is usually determined weeks or months after the cold injury when the demarcation zone appears and the dead tissue is sloughed. In mild cases of frostbite, the only necessary treatment may be daily whirlpool baths with bed rest. However, treatment of deep frostbite should be considered a medical emergency because the early institution of medical therapy may reduce the amount of subsequent tissue loss. Thawing, the mainstay of therapy, should not be implemented if the patient may be re-exposed to cold because refreezing of thawed tissue promotes further tissue damage. Walking on a frozen limb produces substantially less damage than walking on a thawed limb. After thawing, reappearance of normal color signifies the re-establishment of blood flow. Thawing is often a very painful process and may require the administration of narcotics. A frostbite protocol consisting of debridement of clear blisters with a topical application of aloe vera, oral ibuprofen, and daily hydrotherapy is highly effective. An important principle is to avoid early debridement or amputation, which is indicated only when infected gangrene or generalized sepsis occurs. It may be classified as the primary or idiopathic category, which may be non-familial or familial. The secondary category is associated with other diseases, the most common being myeloproliferative disorders such as polycythemia vera and essential thrombocythemia. Other diseases associated with secondary erythromelalgia include hypertension, diabetes, rheumatoid arthritis, gout, spinal cord disease, multiple sclerosis, systemic lupus erythematosus, cutaneous vasculitis, and viral infection; and it may also result from therapy with various drugs. Erythromelalgia is characterized by the clinical triad of erythema, burning pain, and increased temperature usually of the extremities. The peripheral pulses are generally normal in the primary type and variable in secondary erythromelalgia. The symptoms may occur in "attacks" that last for minutes to hours and occasionally days and are precipitated by a warm environment. Patients seek relief by exposing the affected extremity to a cooler environment, such as placing the extremity in cold water, walking on a cold floor barefoot, or running the air conditioner even in the winter. Erythromelalgia may precede the clinical appearance of a myeloproliferative disorder by several years, so patients older than age 30 should be monitored periodically with blood cell counts. In secondary erythromelalgia, treatment of the underlying disease (phlebotomy in patients with polycythemia vera and normalization of the platelet count in patients with thrombocythemia) may relieve the symptoms. Aspirin is the most effective modality available particularly for patients with erythromelalgia secondary to myeloproliferative disorders. Other therapies with variable success include methysergide, ephedrine, non-steroidal anti-inflammatory drugs, phenoxybenzamine, nitroglycerine, sodium nitroprusside, corticosteroids, and surgical sympathectomy. Popliteal Artery Entrapment Syndrome In the popliteal artery entrapment syndrome there is compression of the popliteal artery due to a congenital anatomic abnormality or 367 an abnormal muscle or fibrous band. The most frequent abnormality is when the medial head of the gastrocnemius muscle compresses the popliteal artery causing medial deviation of the popliteal artery. The clinical presentation is in a healthy, "athletic type" male complaining of typical claudication symptoms in the absence of premature atherosclerosis. Disappearance of the pulse with passive dorsiflexion of the foot or active plantar foot flexion against resistance may suggest the diagnosis. Other diseases that can cause midpopliteal occlusion include cystic adventitial disease, thrombosed popliteal artery aneurysm, and atherosclerosis of the superficial femoral and popliteal arteries. Cystic Adventitial Disease In cystic adventitial disease, gelatinous fluid accumulates in an arterial wall cyst and then the cyst encroaches on the vessel lumen, resulting in stenosis or occlusion. The cyst arises in the outer portion of the media or subadventitial layer, most commonly in the popliteal artery. Cystic adventitial disease is an isolated lesion not associated with a systemic process, and the precise pathophysiologic mechanism is unknown. The disease predominates in men with an approximate ratio of 5:1, and the mean age at diagnosis is about 45 years. Pulse volume recordings may show the characteristic drop in blood pressure and change in waveform configuration in the affected limb. If arterial occlusion has occurred, catheter-directed thrombolytic therapy and/or surgical resection is indicated. Fibromuscular Dysplasia of the Extremities Although fibromuscular dysplasia (in particular, medial fibroplasia) is most common in the renal and carotid arteries (see Chapter 112), it may also occur in peripheral arteries of the extremity (iliac, superficial femoral, popliteal, tibial, subclavian, axillary, radial, and ulnar). These lesions may be asymptomatic or may produce a difference in blood pressure between the two limbs with paresthesias, claudication, or critical limb ischemia. The typical arteriographic appearance of "a string of beads" is virtually pathognomonic of medial fibroplasia.
High-dose H2 -antagonists or medicine zalim lotion celexa 10 mg low cost, preferably medicine cabinets with lights discount celexa 10 mg online, proton-pump inhibitors and dilation of the stricture can lead to healing of the mucosa and less need for repeated stricture dilation mueller sports medicine 10 mg celexa visa. Patients who do not tolerate dilation or require vigorous dilation every 3 to 4 weeks need a definitive antireflux operation symptoms celiac disease buy celexa 20mg amex, following which the stricture may regress medications bad for kidneys discount celexa 10 mg amex. If strictures persist after antireflux surgery medications 4 less canada discount celexa 10 mg on line, esophageal replacement by colon, jejunum, or stomach is a surgical maneuver of last resort associated with a relatively high morbidity and mortality. Patients afflicted by strictures may have significant lung and cardiovascular disease that makes them unsuitable operative candidates. Adequate antireflux therapy with high-dose H2 -antagonists or with a proton-pump inhibitor causes regression of columnar epithelium in some patients. The persistence of confirmed high-grade dysplasia is an indication for esophagectomy, because high-grade dysplasia may progress to carcinoma and because coexistent carcinoma may be undetected on biopsy. If low-grade dysplasia is present, the patient is treated medically with proton-pump inhibitors and undergoes biopsy every 6 to 12 months. Experimental endoscopic ablation therapies using photodynamic therapy, laser, or multipolar electrocoagulation are being tried to remove the columnar epithelium with the hope of subsequent growth of the normal squamous epithelium, primarily in patients with low-grade dysplasia or in patients with high-grade dysplasia who are not surgical candidates. Treatment of the pulmonary complications of reflux in adults relies on improved night posture, gastric acid suppressants, and 663 prokinetic agents. Caution is advised before recommending esophageal surgery in patients with reflux and predominant pulmonary problems, because the cause-and-effect relationship may be uncertain in individual patients. Failure of any or all of these components results in an esophageal motor disorder. The pathogenesis of motor abnormalities of the esophageal body is less well understood. The striated muscle that constitutes the upper to one-third of the body can be affected by primary muscle disease, such as myotonic dystrophy, or by metabolic disease affecting muscle function, such as hypothyroidism. The motor disorders of the body of the esophagus have historically been classified as achalasia or diffuse spasm (Table 124-2). Diffuse spasm may cause esophageal chest pain, dysphagia, or both; segmental contractions are seen on radiography, and the manometric picture is of peristaltic waves interspersed with periods of simultaneous esophageal contractions. Many variations of these "classic" diseases occur; diffuse spasm can progress to achalasia, and many nonspecific motor disorders do not fit either of these syndromes. For example, a common manometric abnormality is high-amplitude, long-duration waves that are peristaltic and can be associated with either esophageal chest pain or dysphagia or both (nutcracker esophagus). Occasionally the nonspecific motor abnormalities may be secondary manifestations of gastroesophogeal reflux. Weakness of the oropharyngeal musculature may cause transfer dysphagia-the inability to propel a solid or liquid bolus from the pharynx to the esophagus. Palatal weakness may lead to nasal regurgitation of fluids or to laryngeal aspiration because of muscular failure to seal off the larynx. This transport dysphagia may be intermittent or continuous, and it may occur with both solids and liquids. It is rare for the arrested material to be regurgitated; often, assuming a particular posture. Chest pain is the other major clinical presentation of esophageal motor disorders. The pain is usually substernal, described as a feeling of pressure or aching, which radiates to the back as well as to the neck, jaw, and arms. It can range in intensity from a transient discomfort to an overwhelming, agonizing pain similar to that of a major myocardial infarction or dissecting aortic aneurysm. The differentiation between angina pectoris and esophageal chest pain may be impossible on clinical grounds; both may be related to exercise, have the same intensity and distribution, and respond to sublingual nitroglycerin. In some patients with esophageal spasm, microvascular coronary spasms may contribute to chest pain and make it difficult to separate cardiac from esophageal etiologies (see Chapter 38). If the sphincter fails to relax on deglutition (as occurs in achalasia), dysphagia occurs, and contents are retained in the body of the esophagus. This failure, coupled with loss of peristalsis (achalasia), leads to marked esophageal retention, regurgitation, and overflow of esophageal contents into the tracheobronchial tree. A careful history is essential in choosing the correct diagnostic tools for evaluating esophageal motor disorders. Air double-contrast examinations of the pharynx can elucidate an unsuspected hypopharyngeal carcinoma or a diverticulum or prominence of the cricopharyngeal muscle. Radiology of the esophageal body offers the best chance of diagnosis when motor disorders are associated with relatively static changes. In achalasia, the body of the esophagus commonly dilates with retention of food, secretions, and barium. Special attention can be paid to the terminal end of the esophagus, which has a smooth, tapering beak. Any irregularity of this beak should lead to a vigorous search for an infiltrating neoplasm of the cardia, which can mimic achalasia clinically and radiologically. If the esophageal muscle is atonic, as is seen in far-advanced scleroderma (see Chapter 290), barium and even air are retained for long periods of time when the patient is in the supine position. Assuming the upright position rapidly clears the barium from the esophagus and leaves a double-contrast view of a dilated esophagus. When the motor abnormality is more intermittent, simultaneous contractions can be occasionally detected fluoroscopically. Such a radiologic appearance is not always evidence for a clinically important motor disorder; elderly patients often show similar radiologic findings and yet are totally asymptomatic (presbyesophagus). Normally, a swallow causes a peristaltic wave to be detected sequentially by pressure detectors spaced along the esophagus. Aperistalsis (no peristaltic response to a swallow), simultaneous single or multiple contractions, prolonged contractions of high amplitude and low velocity, and spontaneous activity not related to swallowing can be recorded. Manometric examination is especially helpful to evaluate chest pain when the patient has an attack during the examination. If the chest pain is simultaneously accompanied by abnormal motor activity, the diagnosis of an esophageal origin of chest pain is established. Similarly, if pH is being simultaneously monitored and the episodes of chest pain correlate closely with drops in intraesophageal 664 Figure 124-2 Diagnostic evaluation of patients with dysphagia. Conversely, if typical chest pain occurs but no change in motor activity or pH is seen, an esophageal cause of pain is unlikely. Unfortunately, such definitive statements can be made only for a small minority of the patients examined. Pharmacologic stimulation of the esophagus with short-acting edrophonium (Tensilon) is safe and can provoke chest pain and simultaneous esophageal contractions; such testing is sometimes helpful in patients with normal baseline esophageal manometry. Prolonged esophageal pH monitoring and pH/motility monitoring may help correlate symptoms of dysphagia or chest pain to reflux episodes or motility abnormalities. Endoscopy is useful for evaluating motor disorders, for inspecting the cardia with a retroflexed view from the stomach (to exclude an infiltrating carcinoma), and for excluding inflammatory disorders. Therapeutic trials with a proton-pump inhibitor may also help establish gastroesophageal reflux as a cause of chest pain. Achalasia is the most treatable esophageal motor disorder; all forms of therapy are directed at relieving obstruction. Short-term improvement in clinical symptoms and in scintigraphic esophageal emptying may occur with isosorbide dinitrate or nifedipine, but pharmacologic treatment usually is not successful for long-term management. Dilation with a pneumatic bag under radiographic control is the preferable initial therapy for almost all patients. It should be performed by an expert, because perforation, even in good hands, may occur in about 5% of patients. Surgery is reserved for patients in whom bag dilation fails or for patients who do not wish to be exposed to the risk of perforation. A, the normal swallow consists of a progressive wave with a wave of short duration and rapid rise time in the striated upper esophagus. B, In achalasia, the striated muscle sometimes, but not always, produces a typical wave. The smooth muscle portion of the esophagus has a simultaneous low-amplitude contraction that follows the striated muscle contraction. C, Diffuse spasm shows an elevation of the baseline after swallowing, on top of which are superimposed repetitive simultaneous contractions. Striated muscle contraction is normal, but the amplitude of contraction in the smooth muscle is reduced, or contraction may be absent. It is used in patients at high risk for complications during dilation or surgery; its role in idiopathic achalasia is controversial owing to the incomplete and short-lived responses it evinces. Patients with diffuse spasm can be given nitroglycerin, anticholinergics, or calcium-channel antagonists. Treatment of other nonspecific motor disorders, such as nutcracker esophagus associated with chest pain, can be equally frustrating. Sublingual nitroglycerin may help and may predict the success of long-acting nitrate therapy. Calcium-channel antagonists reduce the force of the esophageal contractions and may relieve pain. Meperidine (Demerol) has been useful but is not a good long-term solution to the problem. Some patients respond to gastric acid suppression, indicating that some of these nonspecific motility disorders may be caused by gastroesophageal reflux. The treatment of scleroderma and other conditions marked by aperistalsis revolves mostly around the associated reflux. If no obstruction exists at the lower end of the esophagus-either as a result of malfunctioning sphincter or as a result of organic narrowing-aperistalsis is amazingly well tolerated, usually with only mild dysphagia for solids. Antireflux surgery should be offered with caution to patients with scleroderma, as a tight fundoplication without any peristalsis in the body of the esophagus leads to severe dysphagia. Additionally, fundoplication has poor results because the disease progresses to severe muscle atrophy and collagen deposition in the esophageal wall. Carcinoma of the esophageal epithelium, both squamous cell and adenocarcinoma, is by far the most common and important tumor of the esophagus. Benign neoplasms (leiomyoma, papilloma, and fibrovascular polyps) are rarer and are usually discovered incidentally. Squamous cell cancer has an incidence of 5 per 100,000 in men in the United States, rising to 130 per 100,000 in North China. Esophageal cancer occurs more commonly in patients with squamous cancers of the head and neck, in those with lye strictures, and in patients with untreated or inadequately treated achalasia. The actual incidence of adenocarcinoma in a patient with columnar epithelium is probably less than the original estimate of 10 to 15%, but the tumor still represents a significant problem. The incidence of esophageal adenocarcinoma has been increasing in frequency over the last several decades. In Western countries, the most common clinical symptom of carcinoma is progressive dysphagia over a several-month period until only liquids can be taken. The obstruction reflects circumferential involvement of the esophageal wall by tumor and does not occur until the cancer is biologically far advanced. The dysphagia may be accompanied by a steady, boring pain, which often signals mediastinal involvement and inoperability. Unexplained persistent chest pain should always be investigated by a careful double-contrast radiographic view of the esophagus or by endoscopy. Coughing after drinking fluid may be caused either by nearly complete esophageal lumen obstruction, with overspill into the larynx, or by the development of a tracheoesophageal fistula. Hoarseness from involvement of the recurrent laryngeal nerve by tumor and hematemesis are unusual symptoms. Because dysphagia is the most common presenting symptom of neoplasm of the esophagus, the physician must be sure that cancer is not the cause of dysphagia. The clinical suspicion of cancer of the esophagus should lead immediately to an esophagogram, possibly with double-contrast techniques. Any irregularity, especially if it narrows the lumen, mandates further evaluation. If dysphagia is present, the radiologist should give a bolus of barium-soaked bread or marshmallow to discover any possible sites of arrest. In the presence of suspicious symptoms and normal barium swallow results, endoscopy with biopsy and brushing of any suspicious lesion is indicated. The endoscopist should always obtain a good retroflexed view of the cardia from below, to make certain 666 that an adenocarcinoma of the gastroesophageal junction has not been overlooked (Color Plate 3 C). If narrowing has been seen by barium swallow, endoscopy with biopsy and cytologic brushings of the involved area is required. Biopsy of visible tissue may reveal only inflammation; as many as six to nine deep biopsy specimens should be obtained. Once a tumor is identified, evaluation for local tumor spread, mediastinal nodal involvement, and liver metastases is essential for staging before a therapeutic decision is reached. For upper and mid-esophageal tumors, bronchoscopy is indicated to evaluate for asymptomatic invasion of the tracheobronchial tree. Endoscopic ultrasound is useful to detect the level of invasion and presence of mediastinal lymph node abnormalities and is becoming the favored test to determine if a lesion is resectable. The ideal treatment of esophageal cancer, either for cure or for palliation, has not yet been developed. Choice of therapy depends on the location and size of the lesion, presence or absence of spread, and cell type. No studies have carefully staged patients with the best noninvasive methods available and then randomized them to different treatment modalities. Until an adequate randomized trial after adequate staging is performed, choice of treatment modality will continue to be a matter of preference.
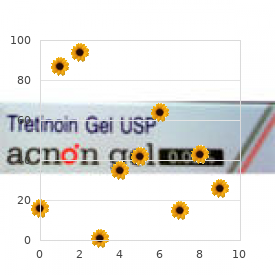
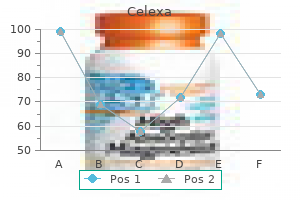
Granulocyte-colony stimulating factor production has been observed in a number of malignancies (malignant fibrous histiocytoma treatment kidney failure generic celexa 10mg on line, nasopharyngeal carcinoma medicine 44175 discount 40 mg celexa mastercard, transitional cell carcinoma of the urinary bladder) and is probably the cause of paraneoplastic leukemoid reaction symptoms job disease skin infections buy celexa 10 mg line. Clinically treatment plan goals and objectives generic 20mg celexa with mastercard, the diagnosis of paraneoplastic leukemoid reaction is made by exclusion of a primary hematologic malignancy such as chronic myelogenous leukemia (see Chapter 176) symptoms yellow fever buy celexa 40mg with visa, which is associated with splenomegaly medications for osteoporosis buy 40mg celexa amex, basophilia, and a left shift of the white blood cells with an increase in all early myeloid progenitors. Treatment of paraneoplastic leukemoid reaction involves therapy directed at the underlying malignancy. Pheochromocytomas, uterine fibroids, sarcomas, and aldosterone-secreting tumors are also associated with cancer-associated erythrocytosis. This paraneoplastic syndrome is associated with increased levels of endogenous erythropoietin in 50% or fewer of patients; in some cases, cancer-associated erythrocytosis may be secondary to the overproduction of androgens, prostaglandins, and other, yet unidentified substances. Treatment of the underlying tumor will result in beneficial effects on the cancer-associated erythrocytosis. This condition must be differentiated from a primary hematologic disorder such as a myeloproliferative disorder (chronic myelogenous leukemia or primary thrombocythemia) or a secondary cause (chronic inflammation, severe iron deficiency, acute bleeding, or post-splenectomy status). Treatment of the malignancy will generally result in a decrease in the platelet count. Despite the elevated platelet count, secondary thrombocytosis is not generally associated with clinical evidence of thrombotic or bleeding disorders. Paraneoplastic nephrotic syndrome usually improves dramatically when the underlying malignancy is successfully treated. Deposition of tumor-associated antigen-antibody complexes can cause membranous glomerulonephritis. Patients often have fever and weight loss, in addition to hepatomegaly, elevated aminotransferase levels, and poor liver synthesizing ability (indicated by an elevated prothrombin time). A liver biopsy may reveal Kupffer cell hyperplasia with fairly non-specific inflammatory changes. In the presence of non-metastatic hypernephroma, treatment directed at the primary lesion generally results in resolution of the syndrome. Surgical resection of the primary tumor has also been reported to reverse the liver abnormalities. If signs or symptoms persist, an evaluation for metastatic disease should be initiated. Pulmonary osteoarthropathy consists of symmetrical clubbing of the nails, active synovitis, and periosteal inflammation of the long bones (often manifested as "arthritis" of the elbows, wrists, knees, or ankles). Pulmonary osteoarthropathy can precede the diagnosis of cancer by months; it is generally observed with lung carcinoma (non-small cell lung histology) but has also been described with metastatic lung lesions, non-pulmonary malignancies, and a number of non-malignant conditions. The development of pulmonary osteoarthropathy may be based on two components: a neurogenic vascular component and a humorally mediated osteogenic element. Vagotomy will partially reverse some symptoms, thus supporting the neurogenic vascular etiology. Other possible etiologies include an immune-mediated response or release of growth factor(s) by the tumor. The classic triad of clubbing, synovitis, and periostitis may appear at different times in the clinical course. Although the joints of the lower extremities may be painful, red, and swollen, physical examination may reveal that the "arthritis" is discomfort caused by pain in the adjacent long bone, especially the distal ends of the radius/ulna and tibia/fibula. Bone scans appear to be more sensitive than plain radiographs and may confirm the diagnosis. Pulmonary osteoarthropathy can be differentiated from metastatic bone disease or rheumatoid arthritis by the symmetrical bilateral findings and the absence of rheumatoid factor. Because pulmonary osteoarthropathy is not life threatening, treatment is often palliative. Arthritic symptoms may be treated with aspirin and/or non-steroidal anti-inflammatory drugs. Surgery of the primary malignancy may improve the articular complaints, sometimes within hours. Review of recent advances in the pathophysiology of paraneoplastic nervous system disorders. Salmon the development of effective anticancer drugs has progressively integrated medical management with surgery and radiation therapy in the multimodal treatment of cancer. The development of new cytotoxic and endocrine agents and the introduction of biologic therapy based on recombinant synthesis of interferons and cytokines have expanded medical management, as has the treatment of the complications of cancer. The physician also must be familiar with palliative aspects of cancer care, including management of pain (see Chapter 27) and treatment of life-threatening complications (see Chapter 199). Although current systemic therapy can cure few forms of metastatic cancer, it is now increasingly effective as a component of multimodal management of apparently localized cancers known to have a high frequency of occult micrometastatic spread. This approach is predicated on the availability of specific systemic agents with antitumor activity in advanced cancers of the same histopathology. Not all patients are candidates for attempts at cancer therapy because of limitations in available drugs or co-morbidity from other medical problems. To a significant extent, cancer is a disease of the elderly, and treatment for many types of cancer in patients older than the age of 65 remains difficult because of the reduced host tolerance to the toxicities of many cancer chemotherapeutic agents. Patients and families must be fully informed about the nature of planned treatment, whether curative or palliative in intent. Inasmuch as prognosis for individual patients is currently based on statistical estimates, the physician must evaluate each patient individually in relation to relevant prognostic factors in attempting to develop a treatment plan. Accurate histologic diagnosis and staging critically influence treatment selection. Increasingly, immunohistochemical analysis helps in subtyping lymphomas and distinguishing among various morphologically "undifferentiated" neoplasms (see Chapter 200). Tumors of diverse histogenesis can have markedly different prognosis and treatment. Electron microscopy sometimes can help by identifying specific morphologic features such as melanosomes (in melanoma) or desmosomes (in carcinomas) that permit more specific classification. Cellular proto-oncogene amplification and expression have been linked to the pathogenesis of various neoplasms (see Chapter 191). Determination of the status of the products of the p53 and retinoblastoma genes is becoming increasingly important in assessing tumor biology and prognosis, because tumors with mutant or null p53 and lacking a functional retinoblastoma protein may have a poor prognosis. In the leukemias and lymphomas, such information can prove important for selecting appropriate treatment approaches. For example, the approach to treatment of T-cell or B-cell lymphomas differs as a function of cell lineage, which often cannot be identified with standard histologic approaches. Specialized studies can in some instances provide evidence for a treatable or curable form of cancer that might otherwise go unrecognized. Assessment of the body burden and spread of cancer by clinical means (staging) is important in developing the treatment plan. Most staging systems assess the size of the primary tumor and define regional lymph node involvement as well as the presence or absence of distant metastatic disease. It is important to distinguish between clinical and pathologic staging and to recognize that pathologic staging employing surgical biopsy is generally more accurate. In the diagnostic evaluation of specific forms of cancer, such as breast or prostate cancer, bone scans can be useful to evaluate advanced disease but have minimal use in early localized disease unless the patient has skeletal symptoms. It is important to focus on the benefit-to-risk ratio of invasive procedures such as staging laparotomy. Even in these cases, a pathologic diagnosis should be established if at all possible before treatment is started. Once diagnosis and staging have been performed, the information must be integrated into an optimal treatment plan. For patients with apparently localized cancers, multidisciplinary input is important, because a combined-modality approach may be indicated. For many tumor types, histopathologic features such as grade of tumor cell differentiation are important, with a less differentiated or undifferentiated phenotype indicating a more aggressive neoplasm. For some sites, other biologic factors are of greater value than histologic grade. By contrast, almost all patients with diffuse large cell (intermediate- or high-grade) lymphoma should be treated aggressively with curative intent, irrespective of stage, unless they are very elderly and have other major medical problems. If cure is not an option, one must consider whether palliation with prolongation of survival (and relief of symptoms) can be achieved. For old and infirm patients, a palliative approach may be preferable, particularly if there is significant morbidity associated with the treatment approach under consideration. On the other hand, some forms of cancer therapy are very effective and well tolerated even with advanced age. A fourth modality, biologic therapy (cytokines, antibodies, vaccines), is beginning to add another dimension to treatment programs. Surgery is a simple and safe means to remove solid tumors when the tumor is confined to a specific anatomic site of origin. However, in the case of some solid tumors, most patients already have metastatic disease at the time of presentation. Additionally, the technical complexity of the surgical procedure, the type of anesthesia needed, and the experience of the personnel must also be considered. With advances in both radiation and chemotherapy, the need for radical surgery has diminished. For testicular cancer, even in the presence of limited metastatic disease, regional lymphadenectomy after radical orchiectomy can be curative and eliminate the need for chemotherapy in some patients who have metastases only to retroperitoneal lymph nodes. For many other sites, surgical resection of regional lymph nodes is performed for diagnostic rather than therapeutic purposes. For example, in breast cancer, the presence or absence of axillary lymph node involvement is the single most important factor in evaluating the likelihood of distant recurrence, and this information is currently not obtainable by non-surgical means. Similarly, surgical staging of nodal involvement in colorectal cancer plays an important role in deciding whether adjuvant systemic chemotherapy is indicated. Initial cancer therapy often requires a multimodal approach to maximize the chance of cure while simultaneously reducing the extent of surgery required. Multimodal approaches require close communication among the involved physicians before surgery. Early communication is improved by obtaining histopathologic diagnosis by needle biopsy or local excision of the primary cancer before more extensive therapy. Two examples are of note in this regard: (1) the management of osteogenic sarcoma with limb salvage surgery, irradiation, and adjuvant chemotherapy and (2) the management of early breast cancer with lumpectomy, axillary staging followed by primary irradiation, and adjuvant systemic administration of cytotoxic or endocrine agents. In both instances, the combined approach yields a better cosmetic and functional outcome. Screening mammography can establish a diagnosis of breast cancer when the tumor is less extensive and when likelihood of cure is greater. Improved plastic surgical techniques have also made breast reconstruction possible for women who either require or prefer mastectomy rather than lumpectomy followed by radiation therapy. In addition to its use in diagnosis, staging, and primary therapy, cancer surgery also plays an important role in the management of some patients with more extensive cancer. In ovarian cancer, when the gynecologic oncologist "debulks" peritoneal and omental spread and leaves the patient with minimal residual disease, patients become better candidates for systemic chemotherapy and have a better survival. Additionally, early resection of pulmonary metastases of soft tissue sarcomas or of solitary brain metastases in melanoma, colon, or breast cancer may provide marked palliation and improved survival, albeit with only occasional cures. Radiation Therapy Radiation therapy has made major strides in instrumentation, physics, radiobiology, treatment planning, and applications to curative and palliative cancer therapy. In general, the term radiation refers to ionizing radiation that is either electromagnetic or particulate. Compared with surgery, radiation therapy has distinct advantages in the locoregional treatment of cancer. Radiation causes less acute morbidity and can be curative for some specific sites while preserving organ or tissue structure and function. An example is the use of radiation for the curative treatment of early-stage laryngeal cancer wherein vocal function can be preserved. The basic unit of ionizing irradiation is the gray (Gy), which has superseded the rad (1 Gy = 100 rads = 100 cGy) (see Chapter 19). Large tumors frequently have poorly perfused, hypoxic zones in which radiation often fails to induce needed reactive intermediaries. For example, electron-beam irradiation deposits most of its energy in the skin and soft tissues and can be useful for superficial therapy of skin neoplasms such as mycosis fungoides. Low-energy (kilovoltage) x-rays expend most of their effects on the overlying tissues above a deep-seated tumor and therefore cause considerable normal tissue damage. By contrast, higher-energy x-rays (megavoltage) or x-irradiation from a cobalt-60 source spare the skin, deposit their energy at greater depth, and provide a better approach to treating deep-seated neoplasms. The use of multiple irradiation fields reduces the dose to normal tissue while increasing the dose to the tumor. The use of fractionated doses causes less cumulative damage to normal tissues than to the tumor, because the normal tissues are often able to repair sublethal damage more quickly. Additionally, as a tumor shrinks with therapy, its oxygenation can improve and render it more radiosensitive. The selection of treatment is based on the relative radiosensitivity of the tumor and of the normal organs and tissues within the radiation field (Table 198-1). Although the major uses of radiation therapy involve local irradiation of sites of tumor involvement, total-body irradiation or total lymphoid irradiation is a valuable part of a preparative regimen for allogeneic or autologous bone marrow transplantation for leukemia or lymphoma (see Chapter 182). Irradiation can also cause sufficient cytoreduction of tumor in bone to permit healing of osteolytic lesions and thereby prevent pathologic fractures of weight-bearing bones. Other examples include tumor shrinkage to relieve postobstructive infection in lung cancer and to suppress bronchial or gastric bleeding secondary to cancer. Although modern radiation therapy with megavoltage equipment has proved to be extremely useful, even higher energy radiation approaches are currently in development. Additionally, several classes of compounds are under study as radiosensitizers to enhance the cytotoxic effects of radiation on tumor cells.
Buy celexa 40 mg. Inspirational Quotes - Life Never Ends Quotes | Magical Words.