





|
STUDENT DIGITAL NEWSLETTER ALAGAPPA INSTITUTIONS |

|
SHALENDER BHASIN, MD
An obstructive defect is present in 20% of patients heart attack the alias radio remix demi lovato heart attack remixes 20 avalide 162.5 mg without prescription, most of whom are current or past smokers blood pressure vitamin d cheap avalide 162.5 mg free shipping. Chest radiography reveals bilateral diffuse alveolar opacities with normal lung volumes pulse pressure locations order avalide 162.5 mg without a prescription. Infiltrates may be peripheral blood pressure chart based on age purchase avalide 162.5mg line, as seen in chronic eosinophilic pneumonia, or migratory. In selected instances the diagnosis can be made by transbronchial biopsy, but thoracoscopic or open lung biopsy is usually required to confirm this diagnosis. Corticosteroid therapy is the most common treatment and results in recovery in two thirds of patients. Clinical improvement is rapid (days to a few weeks) in some individuals, but relapse may occur when steroids are withdrawn; retreatment is often successful. It must be differentiated from other lymphocytic infiltrations of the lung, including primary lymphomas and lymphomatoid granulomatosis. Corticosteroid therapy is successful in approximately 50% of patients, although some patients progress to end-stage lung disease or lymphoma. Histiocytosis X is a term that encompasses three systemic diseases (eosinophilic granuloma, Letterer-Siwe disease, and Hand-Schuller-Christian disease) that have in common an abnormal proliferation of a mononuclear cell, the Langerhans cell. Pleuritic chest pain and acute dyspnea secondary to spontaneous pneumothorax occur in 25% of patients. Cystic bone lesions (skull, ribs, pelvis) accompany the pulmonary disease in 10% of cases. Pulmonary function studies demonstrate a mixed obstructive and restrictive pattern. Morphologically, a granulomatous reaction develops in a bronchocentric distribution but also involves the walls of blood vessels and the interstitium. The clinical course of histiocytosis X is variable; spontaneous remission, stabilization, and disease progression may all occur. Lymphangioleiomyomatosis is a rare disorder occurring only in women of child-bearing age. It is characterized by smooth muscle cells proliferating in the lymphatic, peribronchial, perivascular, and interstitial tissues of the lung. Very little inflammation is present, but in most cases, the alveolar walls are eventually destroyed. Patients present with dyspnea, chylous pleural effusions (secondary to obstruction of the pleural lymphatics), and recurrent pneumothorax (due to rupture of emphysematous cysts). Coarse reticular infiltrates with areas of cystic dilation are noted on chest radiography. Numerous thin-walled cysts are distributed diffusely without a predilection for specific regions or lobes. Nodules, interstitial fibrosis, and irregular lung pleural interfaces, features that are observed in other chronic interstitial lung diseases, are absent. Pleural effusions or recurrent pneumothoraces may be the sole radiographic manifestation. Hormonal influences are thought to be important in the pathogenesis because lymphangioleiomyomatosis occurs predominantly in premenopausal women and is accelerated during pregnancy, the postpartum period, and exogenous estrogen therapy. Lung transplantation has been successful in patients with lymphangioleiomyomatosis. Associated pleural rubs may be heard, and clubbing occurs in as many as 75% of cases. The presence of rheumatoid nodules, pleural fibrosis, and adhesions is also helpful diagnostically. Progressive bronchiolitis obliterans is also associated with rheumatoid arthritis. Clinical manifestations include the abrupt onset of dyspnea and dry cough associated with rales and midinspiratory squeaks, occurring particularly in middle-aged women with seropositive rheumatoid arthritis. Pulmonary function studies reveal airflow obstruction, arterial hypoxemia, and respiratory alkalosis. The predominant lesion is bronchiolitis with lymphoplasmacytic infiltration of the small airway walls and obliteration of the bronchiolar airspace with granulation tissue. Acute lupus pneumonitis is characterized by the acute or subacute onset of tachypnea, tachycardia, dyspnea, cough, and cyanosis. High doses of corticosteroids are indicated in severely ill patients with acute pneumonitis; azathioprine can be added for refractory cases. Clinical manifestations include dyspnea, initially with exertion and later at rest, but this symptom may be denied because of marked limitation of physical activity. Primary pulmonary hypertension may occur in the absence of pulmonary fibrosis and is often the cause of cor pulmonale. In general, correlation between the severity of pulmonary and cutaneous manifestations in scleroderma is poor. Pulmonary function abnormalities have significant prognostic implications: patients with normal function have a greater than 90% 5-year survival, whereas those with restrictive spirometry have a 58% 5-year survival. D-Penicillamine may diminish the rate of visceral disease, but no data show improvement in lung function. A significant association exists between the development of bronchogenic carcinoma and chronic pulmonary fibrosis in scleroderma. The majority of bronchogenic carcinomas are either bronchoalveolar cell or adenocarcinoma. The clinical presentation includes progressive dyspnea on exertion, nonproductive cough, and basilar rales, but a rapidly progressive syndrome (Hamman-Rich) may occur. Lung disease may precede muscle complaints by months to years or be superimposed on established muscular disease. Corticosteroids have stabilized and improved symptoms and physiologic abnormalities in up to 40% of patients. Corticosteroids and immunosuppressive drugs are used in patients with extraglandular 417 involvement. Evidence of pulmonary dysfunction has been reported in as many as 80% of patients with mixed connective tissue disease. A proliferative vasculopathy with intimal thickening and medial muscular hypertrophy affects pulmonary arteries and arterioles and is usually more prominent than the associated interstitial fibrosis. Upper lobe fibrobullous disease, the most common pulmonary manifestation of ankylosing spondylitis, is found in patients with advanced disease. The disease is usually bilateral, and the chest radiograph commonly shows diffuse reticulonodular infiltrates in the upper lung zones with cyst formation as a result of parenchymal destruction. Patients with ankylosing spondylitis appear to be predisposed to typical and atypical tuberculosis. Additionally, aspergillomas are a late complication of colonization of the apical fibrobullous cavities. A diffuse reticulonodular infiltrate, perhaps accompanied by a pleural effusion, is noted on the chest radiograph. Pulmonary function studies reveal a restrictive defect, and arterial blood gas analysis reveals hypoxemia and hypocarbia. The infiltrate may be asymmetrical; a pleural effusion (usually unilateral) is present in one-third of patients. Dyspnea and nonproductive cough begin 6 months to several years after initiating therapy. A diffuse interstitial process with lower zone predominance is noted on chest radiograph. Corticosteroid therapy can be used if no improvement occurs after 2 months, but data regarding its use are scanty. Methotrexate causes granulomatous pneumonitis in 5% of patients on low-dose methotrexate for rheumatoid arthritis or other chronic inflammatory conditions. Hilar lymphadenopathy is seen in 10 to 15% of patients, and pleural effusion is present in 10%. When methotrexate is used in low doses, granulomatous pneumonitis is usually noted after administration of approximately 10 mg/week for an average of 80 weeks. Most patients respond favorably to discontinuing methotrexate; corticosteroids may also be helpful, but deaths have been associated with this pneumonitis. Risk factors include maintenance doses greater than 400 mg/day and previous pulmonary disease. The combination of amiodarone with general anesthesia, cardiopulmonary bypass, or pulmonary angiography is synergistic for development of acute lung injury. The most common presentation includes the insidious development of dyspnea, cough, fever, and malaise accompanied by weight loss.
Because of their long duration of action heart attack 2013 film order avalide 162.5 mg visa, acid hypersecretion can be controlled in all patients with once- or twice-a-day dosing pulse pressure 12 discount avalide 162.5mg fast delivery. Long-term therapy appears safe arrhythmia young age discount avalide 162.5 mg on line, with patients treated with omeprazole for up to 9 years without loss of efficacy but with decreasing vitamin B12 levels after prolonged treatment arrhythmia from clonidine purchase 162.5 mg avalide with visa. Total gastrectomy is now performed only for patients who cannot or will not take oral antisecretory medications. Selective vagotomy effectively reduces acid secretion, but many patients continue to require a low dose of drug. Small duodenal gastrinomas (<1 cm) are frequently not detected by any imaging modality but can be found at surgery if routine duodenotomy is performed. Surgical resection decreases the metastatic rate and results in a 5-year cure rate of 30%. Patients with metastatic gastrinoma in the liver have a poor prognosis with a 5-year survival rate of 30%. If the metastatic disease is increasing in size or is symptomatic, chemotherapeutic agents (streptozotocin, 5-fluorouracil, doxorubicin) are usually the first treatment. Treatment with interferon alfa or octreotide is reported to be effective in a small percentage of patients if chemotherapy fails. Liver transplantation is occasionally used in the rare patient with metastases limited to the liver. The characteristic rash is usually found at intertriginous and periorificial sites, especially in the groin and buttocks. It is initially erythematous and becomes raised with central bullae that erode and become crusty. Glucagonomas are generally large when discovered (mean size, 5-10 cm), most frequently in the pancreatic tail (>50%); liver metastases are usually present at diagnosis (45-80%). The etiology of the rash is unclear, but it may be related to zinc deficiency in some patients. The hypoaminoacidemia is thought secondary to the effect of glucagon on amino acid metabolism by altering gluconeogenesis. The diagnosis is established by demonstrating elevation of plasma glucagon levels. Normal levels are 150 to 200 pg/mL; in patients with glucagonomas, levels usually (>90%) are more than 1000 pg/mL. However, in some recent studies up to 40% of patients had plasma glucagon values of 500 to 1000 pg/mL. Increased plasma glucagon levels are reported in renal insufficiency, acute pancreatitis, hypercortisolism, hepatic diseases, severe stress (trauma, exercise, diabetic ketoacidosis), prolonged fasting, and familial hyperglucagonemia. In these conditions the level does not usually exceed 500 pg/mL except in patients with hepatic diseases such as cirrhosis or familial hyperglucagonemia. Subcutaneous administration of the synthetic long-acting somatostatin analogue octreotide controls the rash in 80% of patients and improves weight loss, diarrhea, and hypoaminoacidemia but usually does not improve the diabetes mellitus. Zinc supplementation or infusion of amino acids can diminish the severity of the rash. After tumor localization, surgical resection is preferred, and even debulking the tumor may be of benefit. For residual disease, chemotherapy with dacarbazine or streptozotocin and doxorubicin, hepatic embolization, or chemoembolization may help control symptoms. The cardinal clinical feature is severe, large-volume, watery diarrhea (>1 L/day) (100%), which is secretory and occurs during fasting. Hypokalemia (80-100%) and dehydration (83%) commonly occur because of the volume of the diarrhea. Achlorhydria was originally reported, but hypochlorhydria is more usually found (54-76%). Flushing occurs in 20% of patients, hyperglycemia in 25 to 50%, and hypercalcemia in 25 to 50%. The normal value in most laboratories is less than 190 pg/mL, and elevated levels are present in 90 to 100% of patients in various series. Tumor localization studies with somatostatin receptor scintigraphy and surgical resection are preferred if possible; chemotherapy with streptozotocin and doxorubicin, hepatic chemoembolization, or hepatic embolization may benefit patients with unresectable or residual tumor. These symptoms occur three to four times more commonly (80-95% of all cases) in patients with pancreatic than in patients with intestinal somatostatinomas. Although these von Recklinghausen tumors are commonly called somatostatinomas because of the immunocytochemical finding of somatostatin in the tumor, the plasma somatostatin level is not usually elevated, and they are not clinical somatostatinomas. Sixty per cent of somatostatinomas occur in the pancreas and 40% occur in the duodenum/jejunum. Pancreatic somatostatinomas occur in the pancreatic head in 60 to 80% of cases, 70 to 92% have metastasized at diagnosis, and they are usually large (mean, 5 cm), solitary tumors. In the gastrointestinal tract, somatostatin inhibits basal and stimulated gastric acid secretion, pancreatic secretion, intestinal absorption of amino acids, gallbladder contractility, and release of numerous hormones, including cholecystokinin and gastrin. Somatostatinomas are usually found by accident, particularly at exploratory laparotomy 687 for cholecystectomy, during endoscopy, or on imaging studies. The diagnosis requires the demonstration of increased plasma and tumor concentrations of somatostatin-like immunoreactivity, which is also found with endocrine tumors outside the pancreas or intestine, including small cell lung cancer, medullary thyroid carcinoma, pheochromocytomas, and paraganglioma. Somatostatinomas can be imaged using somatostatin receptor scintigraphy or, if needed, other conventional imaging studies to assess tumor location and extent. Surgery, if possible, or chemotherapy, hepatic chemoembolization, or hepatic embolization may be of value. The symptoms and signs are due to the tumor per se and include abdominal pain, hepatosplenomegaly, cachexia, and jaundice. Frequently secreted, non-functional peptides include chromogranin A (100%), chromogranin B (100%), pancreatic polypeptide (60%), and the alpha-subunit (40%) and beta-subunit of human chorionic gonadotropin. Immunocytochemically, the tumors contain these peptides as well as insulin (50%), glucagon (30%), and somatostatin (13%). Non-functional pancreatic endocrine tumors are frequently diagnosed only late in the disease course after the patient presents with symptoms or signs of metastatic disease, and a liver biopsy reveals a metastatic neuroendocrine tumor. Any patients with a long survival (>5 years) after a diagnosis of metastatic pancreatic adenocarcinoma should be suspected of having a non-functional pancreatic endocrine tumor. An elevated plasma chromogranin A or pancreatic polypeptide level or positive somatostatin receptor scintigraphy are strong evidence that a pancreatic mass is a pancreatic endocrine tumor. Tumor localization, surgical resection, and chemotherapy with streptozotocin and doxorubicin, hepatic embolization, or chemoembolization are useful, as described earlier. Occasional cases benefit from the use of octreotide, but prognosis is poor even with chemotherapy. Paraneoplastic hypercalcemia can result from a pancreatic endocrine tumor that releases parathormone-related peptide or an unknown hypercalcemic substance. Octreotide may help control the hypercalcemia, but surgery, chemotherapy, hepatic embolization, or chemoembolization are the mainstays of therapy. Talley In clinical practice, the majority of patients who present with chronic or recurrent gastrointestinal symptoms do not have a structural or biochemical explanation identified by routine diagnostic tests. Functional does not imply a psychiatric disturbance or absence of disease but rather a known or suspected underlying disorder of gut function. Based on clinical and epidemiologic studies, the functional gastrointestinal disorders have been classified according to the presumed anatomic site of the disorder (Table 131-1). The most widely recognized functional gastrointestinal disorders are the irritable bowel syndrome, functional (or non-ulcer) dyspepsia, and functional (or non-cardiac) chest pain. In the past, most patients with unexplained abdominal pain or bowel dysfunction were labeled as having irritable bowel syndrome, but irritable bowel syndrome is now considered to be characterized by chronic or recurrent abdominal pain and an erratic disturbance of defecation. Symptoms consistent with irritable bowel syndrome are reported by one in six Americans, and similar prevalence rates have been found in Europe, Australia, and Asia. The prevalence is greater in women but is similar in whites and blacks; it is lower in people older than age 60 years. Approximately 30% of persons with irritable bowel syndrome become asymptomatic over time. Only about one third of persons with irritable bowel syndrome consult a physician, but the condition still accounts for about 12% of primary care visits. Those who seek care for irritable bowel syndrome tend to have more severe abdominal pain, a greater frequency and severity of non-gastrointestinal symptoms, such as headache, fatigue, or menstrual pain, and greater psychological distress. Irritable bowel syndrome is associated with a generalized disorder of smooth muscle function; the colon, small bowel, and upper gastrointestinal tract as well as the gallbladder and urinary tract may be affected. Basal colonic motility is normal in irritable bowel syndrome, but these patients tend to have an abnormally responsive colon to meals, drugs, gut hormones. The motility of the distal colon after meals (the gastrocolonic response) is augmented in patients with irritable bowel syndrome and may explain why postprandial cramps or discomfort is common.
Buy cheap avalide 162.5mg line. Divya Mukta Vati for Hypertension or High Blood pressure.
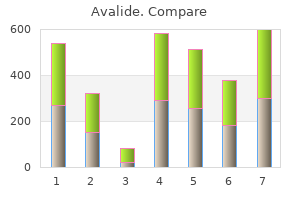
Larger left ventricular diastolic dimension is a robust predictor of worse outcome at every stage of heart failure arrhythmia and palpitation purchase 162.5mg avalide amex. Decrease in left ventricular ejection fraction and/or increase in dimensions over time are ominous blood pressure z score calculator generic avalide 162.5 mg on line. Serum sodium and peak oxygen consumption with exercise are useful prognostic factors blood pressure negative feedback loop discount avalide 162.5 mg with mastercard. Elevated serum norepinephrine and other neuroendocrine abnormalities have been used experimentally but are less often measured clinically blood pressure kiosk discount avalide 162.5mg overnight delivery. Patients considered to have a recent active process with some potential for improvement, such as postviral or peripartum cardiomyopathy, are often advised to avoid vigorous exercise for the next 3 to 6 months. This proscription is derived weakly from data that 343 swimming enhanced mortality in the murine model of acute viral myocarditis and from anecdotal human experience. Patients should be advised, however, to remain mobile, continue regular walking, and avoid daytime bed rest, which leads to deconditioning and depression. When no cause dictates specific therapy, it is important to rule out contributing factors, such as thyroid disease or rapid atrial fibrillation, which could be treated. If there are no such factors, the therapy for cardiomyopathy is as described for various stages of heart failure (see Chapter 48), with prescription of angiotensin-converting enzyme inhibitors in almost all patients, digitalis glycosides in many, and diuretics and additional vasodilators as dictated by the hemodynamic profile. When symptoms of congestion or dyspnea on minimal exertion persist despite empiric therapy with angiotensin-converting enzyme inhibitors, diuretics, and digoxin, compensation can frequently be restored and maintained on a regimen tailored to hemodynamic goals, which include near-normal filling pressures. For patients who are truly refractory to medical therapy but have no other conditions that would compromise long-term survival, cardiac transplantation may be considered (see Chapter 71). Left ventricular reduction surgery (Batista procedure) is associated with up to a 30% need for acute mechanical devices or transplantation, and the benefits for other patients remain to be defined. Although characterized primarily by decreased distensibility ("diastolic dysfunction"), the restrictive cardiomyopathies are frequently accompanied by some degree of depressed contractility and ejection fraction ("systolic dysfunction"). Hemodynamically, end-diastolic pressures and consequently atrial pressures are elevated initially, with relative preservation of cardiac output until disease is advanced. Although classically considered to be "non-dilated" with normal ventricular dimensions, many restrictive cardiomyopathies are associated with some global or focal ventricular dilation, although less than for equivalent degrees of congestive symptoms in the primary dilated cardiomyopathies. The atria, however, frequently become very enlarged after chronic exposure to high filling pressures. The initial challenge is to distinguish restrictive cardiomyopathy from dilated cardiomyopathy or pericardial disease (see Chapter 65). Echocardiography in restrictive disease usually shows left ventricular diastolic dimension less than 6 to 6. Symptomatic congestion, the major clinical feature of restrictive cardiomyopathy, rarely occurs in primary dilated cardiomyopathy until after the ejection fraction is below 30%. Echocardiographic profiles of abnormal relaxation and diastolic filling are helpful in confirming physiologic impairment in patients with near-normal ejection fraction but are less helpful in distinguishing restrictive from other cardiomyopathy, in which the degree of volume overload determines filling pattern. The difficult distinction between primary restrictive disease and extrinsic pericardial disease often requires comparison of right and left ventricular filling during invasive hemodynamic measurement and pericardial imaging by computed tomography or magnetic resonance imaging, particularly in patients with a history of mediastinal radiation, which can cause both myocardial and pericardial disease. Most restrictive cardiomyopathies result from deposition of abnormal substances in the myocardium (Table 64-4). These are commonly divided into "infiltrative" diseases, in which the abnormal substance is largely between the myocytes, and "storage" diseases, in which abnormal substances accumulate within myocytes. Infiltrative Disease Amyloidosis (see Chapter 297) is the most common cause of infiltrative cardiomyopathy. Instead of an immunoglobulin, however, amyloid deposits in familial amyloidosis contain an abnormal prealbumin (transthyretin) associated with different specific point mutations, many of which involve the kidney or liver without cardiac compromise. Secondary amyloidosis and senile amyloidosis rarely cause clinical cardiac involvement. Amyloid infiltration of the interstitium stiffens the ventricles and also replaces some contractile elements. Although it is also found in the atria, it is not extensive enough to prevent atrial dilation. When amyloid also surrounds the arterioles, it may compromise the microcirculation, further impairing systolic and diastolic function and leading to anginal chest pain in some patients. Some patients may present with orthostatic hypotension due to amyloid autonomic neuropathy. Evidence of involvement elsewhere such as carpal tunnel syndrome, skin friability, or nephrotic syndrome may also suggest the diagnosis of amyloidosis. Electrocardiograms characteristically show markedly decreased voltage despite increased wall thickness on echocardiography. Specific diagnosis in some cases can be made from a characteristic sparkling refractile pattern on echocardiography. Up to 80% of patients have a monoclonal protein identified from either serum or urine. Endomyocardial biopsy, which carries a higher risk of perforation in the amyloid-infiltrated heart, reveals infiltration in the interstitium and around the coronary vasculature with deposits that are pale pink on hematoxylin-eosin stain and are birefringent with the specific Congo red stain. Once amyloidosis has been associated with heart failure, the median survival is less than 1 year, with less than 5% five-year survival. Patients with familial amyloidosis may have a slower course than those with a monoclonal gammopathy. Making the diagnosis is important to exclude potential candidates for cardiac transplantation, after which amyloidosis can recur rapidly. Vasodilator therapy is less effective than in dilated cardiomyopathy, owing to less pronounced systolic dysfunction, greater reliance on high filling pressures, and the frequently accompanying autonomic neuropathy, which predisposes to postural hypotension. Digoxin has not been associated with clear benefit and may carry increased toxicity, particularly through aggravating conduction block. Therapy with colchicine or the combination of melphalan and prednisone for patients with associated monoclonal gammopathy has yielded response rates of only 20 to 30%. Sarcoidosis (see Chapter 81) of the heart can cause a picture of reduced left ventricular ejection fraction with variable degrees of ventricular dilation. It can present as either restrictive or dilated cardiomyopathy (discussed earlier under Granulomatous Disease). Storage Diseases Although amyloidosis and sarcoidosis are seen around myocytes, compromise from the storage diseases results primarily from intracellular accumulation. Hemochromatosis is the most common example in adults, frequently arising from an autosomal recessive disorder in the gene that regulates iron absorption. In the absence of the genetic defect in iron regulation, hemochromatosis can result from iron overload due to hemolytic anemia and transfusions. Disrupted cellular architecture and mitochondrial function lead to cell death and replacement fibrosis. The degree of left ventricular dilation is variable, leading to both dilated and restrictive pictures, with the restrictive aspects dominating earlier in the course. Dilation is generally to left ventricular diastolic dimensions of less than 60 mm, but ejection fractions in severe cases are often less than 30%, unlike the other restrictive diseases. The diagnosis is generally made from the clinical picture, serum iron studies, and genetic testing but may be confirmed by endomyocardial biopsy tissue stained for iron. Early diagnosis is important, because phlebotomy and iron chelation therapy may improve cardiac function before cell injury has become irreversible. Deaths from hemochromatosis result more from cirrhosis and liver carcinoma than from cardiac disease. Specific metabolic enzyme deficiencies can lead to abnormal metabolites accumulating in the myocardium, causing increased ventricular mass and restrictive cardiomyopathy. Mortality from this X-linked disorder in men results from multiple organ involvement in the fourth or fifth decade. Glycogen storage disease (see Chapter 203) results from enzyme deficiencies that lead to excessive deposition of normal glycogen in myocardium, skeletal muscle, and liver. Fibrotic Restrictive Cardiomyopathy Restrictive myocardial disease can occur with diffuse fibrotic changes in the absence of abnormal substance accumulation. Radiation for thoracic malignancy (see Chapter 19) can produce restrictive cardiomyopathy, usually presenting within several years, although occasionally up to 15 years later. This consequence of radiation is less common, however, than pericardial disease, from which it must be distinguished. Fibrosis in the scleroderma heart (see Chapter 290) accumulates in the interstitium but may also result from small vessel ischemia with microinfarction.
Obstruction at the tracheal level is unlikely if less than 10 cm H2 O of positive airway pressure is required to cause a leak of air around the endotracheal tube when the tube cuff is deflated hypertension diagnosis code buy generic avalide 162.5 mg. Obstruction is also unlikely if the patient can breathe around the tube when the cuff is deflated and the proximal end of the tube is blocked blood pressure is low avalide 162.5mg without prescription. Direct or indirect laryngoscopy may be helpful in evaluating potential obstruction at the pharyngeal level prehypertension headaches buy 162.5 mg avalide visa. A strategy incorporating low tidal volume breaths with a level of positive end-expiratory pressure associated with high respiratory system compliance improved outcome blood pressure 220 order 162.5 mg avalide free shipping. Antonelli M, Conti G, Rocco M, et al: A comparison of noninvasive positive-pressure ventilation and conventional mechanical ventilation in patients with acute respiratory failure. Noninvasive ventilation, which has been shown to be effective in patients with acute respiratory failure due to airflow obstruction, also is effective in some patients with parenchymal lung disease. Reviews the indications for kinds of complications from and discontinuation of mechanical ventilatory support. The ratio of respiratory frequency to tidal volume proved to be a helpful indication of the need for mechanical ventilation in this study. Parrillo Shock is a very serious medical condition that results from a profound and widespread reduction in effective tissue perfusion leading to cellular dysfunction and organ failure. Unless it is promptly corrected, this circulatory insufficiency will become irreversible. The most common clinical manifestations of shock are hypotension and evidence of inadequate tissue perfusion. A number of diseases can result in shock, and the specific clinical characteristics of these diseases usually accompany the shock syndrome. To understand the definition of shock, it is important to comprehend the meaning of effective tissue perfusion (Table 94-1). Certain forms of shock result from a global reduction in systemic perfusion (low cardiac output), whereas other forms produce shock due to a maldistribution of blood flow or a defect of substrate utilization at the subcellular level. These latter forms of shock have normal or high global flow to tissues, but this perfusion is not effective due to abnormalities at the microvascular or subcellular levels. Hypovolemic shock results from blood and/or fluid loss and is due to a decreased circulating blood volume leading to reduced diastolic filling pressures and volumes. Cardiogenic shock is caused by a severe reduction in cardiac function due to direct myocardial damage or a mechanical abnormality of the heart; the cardiac output and blood pressure are reduced. Extracardiac obstructive shock results from obstruction to flow in the cardiovascular circuit, leading to inadequate diastolic filling or decreased systolic function due to increased afterload; this form of shock results in inadequate cardiac output and hypotension. The cardiovascular abnormality of distributive shock is more complex than the other shock categories. The most characteristic pattern is decreased vascular resistance, normal or elevated cardiac output, and hypotension. Distributive shock, which results from mediator effects at the microvascular and cellular levels, may produce inadequate blood pressure and multiple organ system dysfunction without a decrease in cardiac output. Although many patients develop pure forms of shock as classified above, others may manifest characteristics of several forms of shock, termed mixed shock. For example, septic shock is considered to be a distributive form of shock; however, prior to resuscitation with fluids, a substantial hypovolemic component may exist due to venodilatation. Also, septic shock patients have a cardiogenic component due to myocardial depression. Patients with severe hemorrhage, classified as hypovolemic shock, may manifest significant myocardial depression. Control of Arterial Pressure One excellent physiologic and clinical measure of perfusion is arterial pressure, which is determined by cardiac output and vascular resistance and can be defined by the following equation: Because the mean arterial pressure and cardiac output can be measured directly, these two variables are used to describe tissue perfusion, although systemic vascular resistance can be calculated as a ratio of mean arterial pressure minus central venous pressure divided by cardiac output. The arterial pressure is regulated by changes in cardiac output and/or systemic vascular resistance. These regulatory mechanisms consist of neural and hormonal reflexes and local factors. Blood flow to the heart and brain is carefully regulated and maintained over a wide range of blood pressure (from a mean arterial pressure of 50 to 150 mm Hg); this autoregulation results from reflexes in the local vasculature and ensures the perfusion of these especially vital organs. Failure to maintain the minimal arterial pressure required for autoregulation during shock indicates a severe abnormality that may produce inadequate coronary perfusion and a further reduction in cardiac function due to myocardial ischemia. The stroke volume is determined by preload, afterload, and contractility, whereas preload is dependent on adequate venous return (see Chapter 40). Vascular Performance Effective perfusion requires appropriate resistance to blood flow to maintain arterial pressure. Therefore, the cross-sectional area of a vessel is by far the most important determinant of resistance to flow. In the systemic vasculature, the major (>80%) site of resistance is at the arteriolar sphincter, and regulation of this arteriolar tone constitutes the major determinant of vascular resistance. The extrinsic factors consist of sympathetic nervous system innervation of arterioles, which are largely regulated by arterial and cardiopulmonary baroreceptors. Circulating epinephrine and norepinephrine are released into the circulation by stimulation of the adrenal medulla. The intrinsic mechanisms include a vascular smooth muscle (myogenic) response in which blood vessels relax or constrict in response to changes in transmural vessel pressure to maintain vessel blood flow at a constant level despite changes in perfusion pressure. Other intrinsic mechanisms are a metabolic response that results from release of vasodilators in response to increased metabolic activity and an oxygen tension response that results in vasodilatation with low oxygen tensions. Vasodilators released locally and systemically include nitric oxide (formerly known as endothelial-derived relaxing factor), prostacyclin, eicosanoids, kinins, and adenosine. In addition to vascular tone, the microvasculature also affects perfusion by obstruction to microvascular flow. In shock, this obstruction can be caused by adhesion of leukocytes or platelets to the endothelium, with sludging and occlusion of microvessels. Activation of the coagulation system with fibrin deposition and microthrombi may contribute to this process. Decreased red or white cell deformability may also aggravate this microvascular dysfunction. Microvascular permeability to fluids or other substances may also be altered by vasoactive mediators, activated leukocytes, and damaged endothelial cells. Because intravascular and extravascular fluid is determined by a balance between hydrostatic pressure and colloid osmotic pressure, damage to the endothelium may cause increased extravasation of fluid into the interstitial space and result in tissue edema. Cellular Function At the cellular level, a number of factors regulate the unloading of oxygen and other substrates to cells. Shock produces cellular dysfunction through three major mechanisms: cellular ischemia, inflammatory mediators, and free radical injury. Cellular ischemia is probably the major cause of cell damage in shock with a low cardiac output. Intracellular acidosis occurs, and anaerobic glycolysis leads to accumulation of lactate. Lack of adequate energy leads to failure of energy-dependent ion transport pumps and the inability to maintain normal transmembrane gradients of potassium, chloride, and calcium; the result is mitochondrial dysfunction, abnormal carbohydrate metabolism, and failure of many energy-dependent enzyme reactions. One important but controversial hypothesis regarding cellular ischemia in shock is the role of oxygen supply dependency. In normal humans, oxygen delivery to tissues (cardiac output נoxygen content of arterial blood) is maintained at a high level so that tissue oxygen consumption [cardiac output נ(oxygen content of arterial blood oxygen content of mixed venous blood)] is not altered or dependent on changes in oxygen delivery. However, if systemic flow drops below a critical value of oxygen delivery, tissues must switch from aerobic metabolism to the less efficient anaerobic metabolism. This deficiency of energy production may lead to multiple organ system dysfunction and death. Below this critical value (estimated at 8 to 10 mL of oxygen/min/kg in anesthetized humans), oxygen consumption is dependent on oxygen delivery (or supply), a relationship termed physiologic oxygen supply dependency. This process is believed to be an important mechanism of cellular damage in forms of shock that are characterized by low oxygen delivery due to inadequate cardiac output, low oxygen saturation, or decreased hemoglobin concentration. These patients have oxygen delivery in the normal or elevated range but manifest lactate production and organ dysfunction. Some animal and human studies suggest the presence of a pathologic oxygen supply dependency because they demonstrate an increase in oxygen consumption with increases in oxygen delivery even at elevated levels of oxygen delivery. This suggests dependency of consumption on delivery over a wide range of delivery values.