





|
STUDENT DIGITAL NEWSLETTER ALAGAPPA INSTITUTIONS |

|
Laxmi S. Mehta, MD, FACC
Indicate the laxative drug belonging to osmotic laxatives: a) Docusate sodium b) Bisacodyl c) Phenolphthalein d) Sodium phosphate 030 bacteria growth experiment order bactrim 960 mg on line. The mechanism of stimulant purgatives is: a) Increasing the volume of non-absorbable solid residue b) Increasing motility and secretion c) Altering the consistency of the feces d) Increasing the water content 031 antibiotics for sinus infection types buy cheap bactrim 480mg online. Choose the drug irritating the gut and causing increased peristalsis: a) Phenolphthalein b) Methyl cellulose c) Proserine d) Mineral oil 032 antibiotics for uti macrodantin cheap 480mg bactrim visa. Tick the stimulant of bile production of vegetable origin: a) Oxaphenamide b) Papaverine c) Cholenzyme d) Cholosas 034 antimicrobial use and resistance in animals buy generic bactrim 480mg. Select the drug which inhibits peristalsis: a) Castor oil b) Bisacodyl c) Loperamide d) Sorbitol 035 antibiotics for dogs chest infection bactrim 960mg discount. Choose the drug depressing erythrogenesis: a) Radioactive phosphorus 32 b) Ferrous sulfate c) Molgramostim d) Folic acid 003 antibiotics japan purchase bactrim 960mg visa. Iron deficiency anemia leads to pallor, fatigue, dizziness, exertional dyspnea and other symptoms of tissue ischemia. Tick the drug for parenteral iron therapy: a) Ferrous sulfate b) Fercoven c) Ferrous lactate d) Ferrous fumarate 007. Indicate the drug which increases absorption of iron from intestine: a) Cyanocobalamin b) Folic acid c) Ascorbic acid d) Erythropoetin 008. Pernicious anemia is developed due to deficiency of: a) Erythropoetin b) Vitamin B12 c) Iron d) Vitamin B6 010. Select the drug used for pernicious anemia: a) Ferrous lactate b) Cyanocobalamin c) Iron dextran d) Ferrous gluconate 011. An adverse effect of oral iron therapy is: a) Anemia b) Thrombocytopenia c) Headache d) Constipation 012. Choose the drug which contains cobalt atom: 74 a) Folic acid b) Iron dextran c) Cyanocobalamine d) Ferrous gluconate 013. Tick the drug used in aplastic anemia: a) Fercoven b) Cyanocobalamine c) Epoetin alpha d) Folic acid 014. Which of the following substances is synthesized within vessel walls and inhibits thrombogenesis Pick out the drug belonging to anticoagulants of direct action: a) Aspirin b) Heparin c) Dicumarol d) Phenprocoumon 005. Indicate the drug belonging to antagonists of heparin: a) Aspirin b) Dicumarol c) Dalteparin d) Protamine sulfate 007. Tick the drug used as an oral anticoagulant: a) Heparin b) Daltreparin c) Dicumarol d) Enoxaparin 008. Indicate the drug belonging to fibrinoliytic inhibitors: a) Aminocapronic acid b) Ticlopidine c) Streptokinase d) Vitamin K 021. Aminocapronic acid is a drug of choice for treatment of: a) Acute myocardial infarction b) Bleeding from fibrinolytic therapy c) Heart failure d) Multiple pulmonary emboli 022. The non-glycoside positive inotropic drug is: a) Digoxin b) Strophantin K c) Dobutamine d) Digitoxin 006. Sugar molecules in the structure of glycosides influence: a) Cardiotonic action b) Pharmacokinetic properties c) Toxic properties d) All of the above 007. Aglycone is essential for: a) Plasma protein binding b) Half-life c) Cardiotonic action d) Metabolism 008. Choose the derivative of the plant Foxglove (Digitalis): a) Digoxin b) Strophantin K c) Dobutamine d) Amrinone 009. Digoxin is thought to increase intracellular concentrations of calcium in myocardial cells by indirectly slowing the action of the sodium-calcium exchanger. Compare the half-life of digoxin and the half-life of digitoxin: a) Digoxin is greater than digitoxin b) Digitoxin is greater than digoxin 013. The most cardiac manifestation of glycosides intoxication is: a) Atrioventricular junctional rhythm b) Second-degree atrioventricular blockade c) Ventricular tachycardia d) All the above 016. The manifestations of glycosides intoxication are: a) Visual changes b) Ventricular tachyarrhythmias c) Gastrointestinal disturbances d) All the above 017. For digitalis-induced arrhythmias the following drug is favored: a) Verapamil b) Amiodarone c) Lidocaine d) Propanolol 018. In very severe digitalis intoxication the best choice is to use: a) Lidocaine b) Digibind (Digoxin immune fab) c) Oral potassium supplementation d) Reducing the dose of the drug 019. This drug is a selective beta-1 agonist: a) Digoxin b) Dobutamine c) Amrinone d) Dopamine 021. Tolerance to this inotropic drug develops after a few days: a) Amrinone b) Amiodarone c) Dobutamine d) Adenosine 022. This drug is useful for treating heart failure because it increases the inotropic state and reduces afterload: a) Amiodarone b) Amrinone c) Propanolol d) Enalapril 024. Drugs most commonly used in chronic heart failure are: a) Cardiac glycosides b) Diuretics c) Angiotensin-converting enzyme inhibitors d) All the above 028. This drug prolongs repolarization: a) Flecainide b) Sotalol c) Lidocaine d) Verapamil 007. This drug is used in treating supraventricular tachycardias: a) Digoxin b) Dobutamine c) Amrinone d) Dopamine 009. This drug has beta-adrenergic blocking activity: a) Flecainide b) Sotalol c) Lidocaine d) Verapamil 011. This drug is useful in terminating atrial but not ventricular tachycardias: a) Flecainide b) Sotalol c) Lidocaine d) Verapamil 012. This is a drug of choice for acute treatment of ventricular tachycardias: a) Flecainide b) Sotalol c) Lidocaine d) Verapamil 013. The calcium channel blockers have direct negative inotropic effects because they reduce the inward movement of calcium during the action potential. This drug is contraindicated in patients with moderate to severe heart failure: a) Nifedipine b) Verapamil c) Both of the above d) None of the above 017. This drug is an effective bronchodilator: a) Nifedipine b) Verapamil c) Both of the above. This drug is used intravenously to terminate supraventricular tachycardias: a) Nifedipine b) Verapamil c) Both of the above d) None of the above 019. This drug has a little or no direct effect on chronotropy and dromotropy at normal doses a) Nifedipine b) Diltiazem c) Verapamil d) All of the above 020. Angina pectoris is: a) Severe constricting chest pain, often radiating from the precordium to the left shoulder and down the arm, due to insufficient blood supply to the heart that is usually caused by coronary disease b) An often fatal form of arrhythmia characterized by rapid, irregular fibrillar twitching of the ventricles of the heart instead of normal contractions, resulting in a loss of pulse c) the cardiovascular condition in which the heart ability to pump blood weakens d) All of the above 002. This drug group useful in angina decreases myocardial oxygen requirement (by decreasing the determinations of oxygen demand) and does not increase myocardial oxygen delivery (by reversing coronary arterial spasm): a) Nitrates and nitrite drugs (Nitroglycerin, Isosorbide dinitrate) b) Myotropic coronary dilators (Dipyridamole) c) Potassium channel openers (Minoxidil) d) Beta-adrenoceptor-blocking drugs (Atenolol, Mtoprolol) 004. This drug group useful in angina increase myocardial oxygen delivery (by reversing coronary arterial spasm) and does not decrease myocardial oxygen requirement (by decreasing the determinations of oxygen demand): a) Beta-adrenoceptor-blocking drugs (Atenolol, Metoprolol): b) Myotropic coronary dilators (Dipyridamole) c) Calcium channel blockers (Nifedipine, Nimodipine) d) Potassium channel openers (Minoxidil) 005. Which of the following nitrates and nitrite drugs is used for prevention of angina attack Duration of nitroglycerin action (sublingual) is: a) 10-30 minutes b) 6-8 hours c) 3-5 minutes d) 1. Which of the following cardiovascular system effects refers to a calcium channel blocker Main clinical use of calcium channel blockers is: a) Angina pectoris b) Hypertension c) Supraventricular tachyarrhythmias d) All of the above 016. Which of the following antianginal agents is a myotropic coronary dilator: a) Dipyridamole b) Validol c) Atenolol d) Alinidine 017. Which of the following antianginal agents is a beta-adrenoceptor-blocking drug: a) Dipyridamole b) Validol 82 c) Atenolol d) Alinidine 018. Which of the following antianginal agents refers to reflex coronary dilators: a) Dipyridamole b) Validol c) Atenolol d) Alinidine 021. Which of the following statements concerning Validol is true: a) Validol has a moderate reflex and vascular dilative action caused by the stimulation of sensitive nerve endings b) At sublingual administration the effect is produced in five minutes and 70 % of the preparation is released in 3 minutes c) It is used in cases of angina pectoris, motion sickness, nausea, vomiting when seasick or airsick and headaches due to taking nitrates d) All of the above 022. Which of the following antianginal agents is the specific bradycardic drug: a) Dipyridamole b) Validol c) Atenolol d) Alinidine 023. Which of the following antianginal agents is a potassium channel opener: a) Dipyridamole b) Validol c) Atenolol d) Minoxidil 026. A ganglioblocking drug for hypertension treatment is: a) Hydralazine b) Tubocurarine c) Trimethaphan d) Metoprolol 004. Pick out the sympatholythic drug: a) Labetalol b) Prazosin c) Guanethidine d) Clonidine 005. Tick the drug with nonselective beta-adrenoblocking activity: a) Atenolol b) Propranolol c) Metoprolol d) Nebivolol 006. Choose the selective blocker of beta-1 adrenoreceptors: a) Labetalol b) Prazosin c) Atenolol d) Propranolol 007. This drug inhibits the angiotensin-converting enzyme: a) Captopril b) Enalapril c) Ramipril d) All of the above 009. This drug is a directly acting vasodilator: a) Labetalol b) Clonidine c) Enalapril d) Nifedipine 010. Pick out the diuretic agent for hypertension treatment: a) Losartan b) Dichlothiazide c) Captopril d) Prazosin 011. This drug blocks alpha-1 adrenergic receptors: a) Prazosin b) Clonidine c) Enalapril d) Nifedipine 012. This drug activates alpha-2 adrenergic receptors: a) Labetalol b) Phentolamine c) Clonidine d) Enalapril 84 013. This drug is an inhibitor of renin synthesis: a) Propranolol b) Enalapril c) Diazoxide d) Losartan 014. This drug is a potassium channel activator: a) Nifedipine b) Saralasin c) Diazoxide d) Losartan 016. This drug is contraindicated in patients with bronchial asthma: a) Propranolol b) Clonidine c) Enalapril d) Nifedipine 018. This drug is converted to an active metabolite after absorption: a) Labetalol b) Clonidine c) Enalapril d) Nifedipine 019. This drug routinely produces some tachycardia: a) Propranolol b) Clonidine c) Enalapril d) Nifedipine 020. The reason of beta-blockers administration for hypertension treatment is: a) Peripheral vasodilatation b) Diminishing of blood volume c) Decreasing of heart work d) Depression of vasomotor center 024. Choose the group of antihypertensive drugs which diminishes the metabolism of bradykinin: 85 a) Ganglioblockers b) Alfa-adrenoblockers c) Angiotensin-converting enzyme inhibitors d) Diuretics 026. Hydralazine (a vasodilator) can produce: a) Seizures, extrapyramidal disturbances b) Tachycardia, lupus erhythromatosis c) Acute hepatitis d) Aplastic anemia 027. The reason of diuretics administration for hypertension treatment is: a) Block the adrenergic transmission b) Diminishing of blood volume and amount of Na+ ions in the vessels endothelium c) Depression of rennin-angiotensin-aldosterone system d) Depression of the vasomotor center 029. The main principle of shock treatment is: a) To increase the arterial pressure b) To increase the peripheral vascular resistance c) To increase the cardiac output d) To improve the peripheral blood flow 002. Pick out the drug which increases cardiac output: a) Noradrenalin b) Methyldopa c) Phenylephrine d) Angiotensinamide 003. Tick the synthetic vasoconstrictor having an adrenomimic effect: a) Noradrenalin b) Adrenalin c) Phenylephrine d) Angiotensinamide 004. Indicate the vasoconstrictor of endogenous origin: a) Ephedrine b) Phenylephrine c) Xylomethazoline d) Angiotensinamide 005. General unwanted effects of vasoconstrictors is: a) Increase of arterial pressure b) Increase of cardiac output c) Decrease of peripheral blood flow d) Increase of blood volume 86 007. For increasing blood pressure in case of low cardiac output the following agents must be used: a) Ganglioblockers b) Vasoconstrictors c) Positive inotropic drugs d) Diuretics 008. Tick the positive inotropic drug of glycoside structure: a) Dopamine b) Digoxin c) Dobutamine d) Adrenalin 009. Tick the positive inotropic drug of non-glycoside structure: a) Digitoxin b) Digoxin c) Dobutamine d) Strophanthin 010. Dopamine at low doses influences mainly: a) Alfa-adrenoreceptors (leads to peripheral vasoconstriction) b) Dopamine receptors (leads to vasodilation of renal and mesenterial vessels) c) Beta-1 adrenoreceptors (leads to enhanced cardiac output) d) All of the above 011. Dopamine at medium doses influences mainly: a) Alfa-adrenoreceptors (leads to peripheral vasoconstriction) b) Dopamine receptors (leads to vasodilation of renal and mesenterial vessels) c) Beta-1 adrenoreceptors (leads to enhanced cardiac output) d) All of the above 012. Tick the group of drugs for treatment of shock with hypovolaemia (reduced circulating blood volume): a) Positive inotropic drugs b) Vasoconstrictors c) Plasmoexpanders d) Analeptics and tonics 014. Tick the group of drugs for chronic hypotension treatment: a) Positive inotropic drugs b) Vasoconstrictors c) Plasmoexpanders d) Analeptics and tonics 015. Tick the drug influencing the blood flow which is related to antiplatelet agents: a) Heparin b) Aspirin c) Pyracetam d) Tanakan 017. Which of the following drugs is related to anticoagulants and may be useful in disorders of cerebral circulation Indicate the drugs which are Ca-channel blockers influencing the brain blood flow: a) Aminalon, Picamilon b) Nimodipine, Cinnarizine c) Heparin, Warfarin d) Vinpocetine, Nicergoline 019. Indicate the drug - Vinca minor alcaloid: a) Nicergoline b) Warfarin c) Cinnarizine d) Vinpocetine 021. Indicate the nootropic agent useful in disorders of brain circulation: a) Aspirin b) Pyracetam c) Warfarin d) All the above 023. Antiaggregants are used in disorders of brain circulation for: a) Stimulation of the metabolic processes in neurons b) Dilation of cerebral vessels c) Improving the microcirculation in cerebral tissue d) All the above 026. Migraine is a disorder connected with: a) Thrombosis of cerebral vessels b) Brain hemorrhage c) Dysfunction of regulation of cerebral vessel tonus d) Malignant growth in brain 027. The following Indol derivative is used for treatment of acute migraine attack: a) Paracetamol b) Sumatriptan c) Ergotamine d) Metoclopramide 029. The following Ergot derivative is used for treatment of acute migraine attack: a) Paracetamol b) Sumatriptan c) Ergotamine d) Metoclopramide 030. Hormones are: a) Products of endocrine gland secretion b) Mediators of inflammatory process c) By-products of tissue metabolism d) Product of exocrine gland secretion 002. Select an endocrine drug which is an amino acid derivative: a) Insulin b) Hydrocortisone c) Calcitonin d) Thyroxine 003.
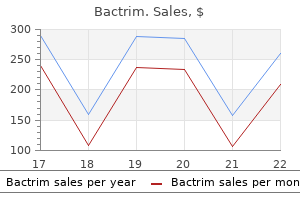
Hypoventilation is usually more prominent at night but can occur during the day in severe cases antibiotic list of names cheap bactrim 960mg without a prescription. These patients typically present in the first hours of life with cyanosis and increased hypercapnia during sleep herbal antibiotics for sinus infection generic 480mg bactrim amex. They have an impairment of ventilatory and arousal responses to both hypercapnia and hypoxemia antibiotics for uti planned parenthood cheap 480 mg bactrim fast delivery. Children present with classic symptoms of primary adrenal insufficiency antimicrobial jacket buy bactrim 480mg low price, including hypoglycemic seizures and shock virus jokes biology discount bactrim 960 mg otc. Less frequently antibiotic 6340 cheap bactrim 480 mg overnight delivery, they present with recurrent vomiting, dysphagia, and failure to thrive or ocular symptoms associated with alacrima. At presentation, review of systems may also be positive for crying without tears, hyperpigmentation, developmental delay, seizures, hypernasal speech, and symptoms related to orthostatic hypotension. More variable features include hypotonia, gait abnormalities, anisocoria, and visual or hearing deficits. Correlates of functional disability in patients with postural tachycardia syndrome: preliminary cross-sectional findings. Childhood obesity and autonomic dysfunction: risk for cardiac morbidity and mortality. Autonomic dysfunction: a possible pathophysiological pathway underlying the association between sleep and obesity in children at-risk for obesity. Metabolic syndrome burden in apparently healthy adolescents is adversely associated with cardiac autonomic modulation-Penn State Children Cohort. An evaluation of autonomic nervous system function in patients with PraderWilli syndrome. Rapid-onset obesity with hypothalamic dysfunction, hypoventilation, and autonomic dysregulation presenting in childhood. Reversibility of cardiac abnormalities in adolescents with anorexia nervosa after weight recovery. Alterations in the autonomic control of heart rate variability in patients with anorexia or bulimia nervosa: correlations between sympathovagal activity, clinical features, and leptin levels. Evaluation of electrocardiographic parameters for early diagnosis of autonomic dysfunction in children and adolescents with type-1 diabetes mellitus. On the Union of Cranial Autonomic (Visceral) Fibres with the Nerve Cells of the Superior Cervical Ganglion. Symptoms and signs of syncope: a review of the link between physiology and clinical clues. Hyperdopaminergic crises in familial dysautonomia: a randomized trial of carbidopa. Lower urinary tract function in childhood; normal development and common functional disturbances. Usefulness of tilt-induced heart rate changes in the differential diagnosis of vasovagal syncope and chronic autonomic failure. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Midodrine in neurally mediated syncope: a double-blind, randomized, crossover study. Cardiac pacing does not improve orthostatic tolerance in patients with vasovagal syncope. Structural and functional small fiber abnormalities in the neuropathic postural tachycardia syndrome. A systematic review of the management of autonomic dysreflexia after spinal cord injury. Carbidopa: A Novel Approach to Treating Paroxysmal Hypertension in Afferent Baroreflex Failure. Pheochromocytoma and paraganglioma in children: a review of medical and surgical management at a tertiary care center. Autonomic ganglia, acetylcholine receptor antibodies, and autoimmune ganglionopathy. Autonomic dysfunction in the Lambert-Eaton myasthenic syndrome: serologic and clinical correlates. The trk protooncogene product: a signal transducing receptor for nerve growth factor. Norepinephrine deficiency with normal blood pressure control in congenital insensitivity to pain with anhidrosis. Case/control family study of autonomic nervous system dysfunction in idiopathic congenital central hypoventilation syndrome. Autonomic dysfunction in adult-onset alexander disease: a case report and review of the literature. Cardiovascular and neuroendocrine features of Panayiotopoulos syndrome in three siblings. Endogenous restoration of noradrenaline by precursor therapy in dopamine-beta-hydroxylase deficiency. Clinical and biochemical features of aromatic L-amino acid decarboxylase deficiency. L-threo-dihydroxyphenylserine corrects neurochemical abnormalities in a Menkes disease mouse model. Re-use, re-processing, or re-sterilization may compromise the structural integrity of the implant and the intended function of the device which could result in patient injury. When preparing the disc space, remove anterior or posterior osteophytes as needed, taking care to minimize bone removal. Avoid excessive bone removal as this may weaken the vertebral endplates or vertebral body. Correct positioning of the rail punch is critical prior to performing the rail preparation step. Ensure proper alignment and placement of device components as misalignment may cause excessive wear and/or early failure of the device. Patients should be instructed in postoperative care procedures and should be advised of the importance of adhering to these procedures for successful treatment with the device. Patients should be advised to avoid any activities that require repeated bending, lifting, and twisting, such as athletic activities. Some of the most common adverse events experienced by study patients were: neck and/or arm pain, dysesthesia, back and/or leg pain, musculoskeletal events (excluding spinal events), and difficulty swallowing. In addition to the risks listed below, there is also the risk that surgery may not be effective in relieving symptoms, or may cause worsening of symptoms. Risks associated with anterior cervical spine surgery include: dysphagia; dysphonia; hoarseness; vocal cord paralysis; laryngeal palsy; sore throat; recurring aspirations; tracheal, esophageal, or pharyngeal perforation; airway obstruction; warmth or tingling in the extremities; neurologic complications including damage to nerve roots, other nerves, or the spinal cord possibly resulting in weakness, pain or even paralysis; dural tears or leaks; cerebrospinal fistula; discitis, arachnoiditis, and other types of inflammation; loss of disc height; loss of anatomic sagittal plane curvature or vertebral listhesis; scarring, herniation or degeneration of adjacent discs; surrounding soft tissue damage, spinal stenosis; spondylolysis; fistula; vascular damage and/or rupture; and headache. Clinical Inclusion and Exclusion Criteria To qualify for enrollment in the study, subjects met all of the following inclusion criteria and none of the following exclusion criteria. Postoperative Care the recommended post-operative care included avoidance of overhead lifting, heavy lifting, repetitive bending, and high-impact exercise or athletic activity for 60 days postoperatively. Post-operative bracing requirements were left to the discretion of the investigators and included the option for use of a soft collar as needed. The use of electrical bone growth stimulators was not recommended during the 24month follow-up period. However, in a few cases where an electrical bone growth stimulator was utilized due to specific patient presentation, they were considered a supplemental form of therapy for spinal fusion surgery, and deemed failures included in the "Supplemental Fixation" Adverse Event category. Complications and adverse events were evaluated over the course of the clinical trial. At each evaluation timepoint, the primary and secondary clinical and radiographic outcome parameters were evaluated. Success was determined from data collected during the initial 24 months of follow-up. An improvement (reduction) of at least 15 points from the baseline Neck Disability Index score; 2. No severe adverse event classified as implant-associated, surgical procedure-associated, or implant/surgical procedure-associated; and 5. The demographic and preoperative characteristics of the subjects who declined to participate in this study were comparable to the patients included in this study. However, none of the deaths were believed to be in any way related to the study treatment. The demographics of the study population are consistent with the demographics reported for prior cervical artificial disc studies conducted in the U. The investigational and control treatment groups were very similar demographically, and there were no statistically significant differences (p<0. However, tobacco use was established through use of patient questionnaires which utilized a binary response. Therefore, it is not possible to definitively ascertain whether there were any substantial confounding effects from tobacco use on patient outcomes. Table 4: Study Patient Demographics and Baseline Characteristics Variables Age (years) Height (inches) Weight (lbs. There were statistically significant differences in baseline motor neurologic status (38. However, after propensity score adjustments, the variables appeared balanced between groups. Thus, differences in baseline symptoms were adjusted for in the analysis and are therefore unlikely to have led to significant bias in the reported results. If a subject has both an arm pain score 20 and a neck pain score 20, then this subject is considered as having "Arm and Neck Pain"; if a subject has a neck pain score 20 and an arm pain score < 20, then this subject is considered as having "Neck Pain Only"; if a subject has an arm pain score 20 and a neck pain score < 20, then this subject is considered as having "Arm Pain Only". Since neck pain score 20 is an inclusion criteria, there are no subjects with "Arm Pain Only". No patients were included into the study with neck pain without any other symptoms. Additionally, investigational subjects were found to have similar estimated blood loss to the control group subjects (50. The percentage of subjects with adverse events was not statistically different between the two groups for all levels except for C5-C6; however, this difference was not clinically meaningful. Adverse event rates are based on the number of patients having at least one occurrence of an adverse event, divided by the number of patients in that treatment group. Subjects experiencing adverse events in more than one category are represented in each category in which they experienced an adverse event. However, when comparing device-related adverse events, the rates are comparable (see Table 10b below). There were a total of three deaths in the investigational group and five deaths in the control group, of which two deaths occurred in the control group prior to 24 months (at the 12-month time point) and none in the investigational group prior to 24 months. Deaths were evaluated based upon available information and none of the deaths were believed to be in any way related to the study treatment. Revisions, removals, and supplemental fixations were considered second surgery failures in the clinical study. Excluding the 5 subjects only using external bone stimulators, the supplemental fixation rates are comparable between the two treatment groups. Please note that since this additional device was used, and included as a supplemental fixation, these patients were considered failures in the Primary Endpoint. Additionally, the patient had removal due to the same diagnosis at 215 days as referenced above. Neurologic success was defined as maintenance or improvement in neurologic status at 24 months compared to baseline. Additional secondary endpoints include radiographic success, indicators of pain relief, general health status, and doctor and subject perceptions of outcomes. Study success was expressed as the number of individual subjects categorized as a success divided by the total number of subjects evaluated. Table 16 describes the observed success rates and Bayesian analyses for individual outcome parameters and overall success. Posterior means for each group can be interpreted as the average chance of success at 24 months, and the posterior mean of the difference can be interpreted as the average difference in the chance of success at 24 months. Given the results of the trial, there is a 95% probability that the chance of success ranges from 74. Given the results of the trial, there is a 95% probability that the chance of success ranges from 61. All success probabilities were for the 24-month outcomes, and posterior probabilities of success were calculated using Bayesian statistical methods and are presented in Table 16. Given the results of the trial, there is a 95% probability that the chance of success ranges from 62. Thus it can be stated that the investigational device is statistically non-inferior to the control procedure as the posterior probability of noninferiority is 99. This histogram uses values obtained by rounding the recorded range of motion for each subject to the nearest integer. Disc height success is achieved when the change in the six-week post-operative height from the post-operative height is greater than or equals -2mm in either the anterior or posterior measurements. Disc height success was similar between the two treatment groups with greater than 90% of the patients in both groups achieving success at each time point.
Choose the characteristics of vancomicin: a) It is a glycopeptide infection kpc buy bactrim 960mg on line, inhibits cell wall synthesis active only against Gram-negative bacteria b) It is a glycopeptide antimicrobial hand soap discount 960 mg bactrim otc, that alters permeability of cell membrane and is active against anaerobic bacteria c) It is a beta-lactam antibiotic bacteria in space generic bactrim 480 mg without a prescription, inhibits cell wall synthesis active only against Pseudomonas aeruginosa d) It is a glycopeptide virus facebook buy bactrim 960 mg low cost, inhibits cell wall synthesis and is active only against Gram-positive bacteria antibiotic 4th generation buy 480mg bactrim fast delivery. Vancomicin has the following unwanted effects: a) Pseudomembranous colitis b) Hepatotoxicity c) "Red neck" syndrome virus 20 deviantart 960 mg bactrim, phlebitis d) All of the above 045. Which of the following drugs is used for systemic and deep mycotic infections treatment: a) Co-trimoxazol b) Griseofulvin c) Amphotericin B d) Nitrofungin 046. Which of the following drugs is used for dermatomycosis treatment: a) Nystatin b) Griseofulvin c) Amphotericin B d) Vancomycin 047. Which of the following drugs is used for candidiasis treatment: a) Griseofulvin b) Nitrofungin c) Myconazol d) Streptomycin 048. Which of the following drugs alters permeability of Candida cell membranes: a) Amphotericin B b) Ketoconazole c) Nystatin d) Terbinafine 052. Amfotericin B has the following unwanted effects: a) Psychosis b) Renal impairment, anemia c) Hypertension, cardiac arrhythmia d) Bone marrow toxicity 053. Tick the drug belonging to antibiotics having a polyene structure: a) Nystatin b) Ketoconazole c) Griseofulvin d) All of the above 129 054. Characteristics of polyenes are following, except: a) Alter the structure and functions of cell membranes b) Broad-spectrum c) Fungicidal effect d) Nephrotoxicity, hepatotoxicity 056. Sulfonamides are effective against: a) Bacteria and Chlamidia b) Actinomyces c) Protozoa d) All of the above 002. Combination of sulfonamides with trimethoprim: a) Decreases the unwanted effects of sulfonamides b) Increases the antimicrobial activity c) Decreases the antimicrobial activity d) Increases the elimination of sulfonamides 004. The following measures are necessary for prevention of sulfonamide precipitation and crystalluria: a) Taking of drinks with acid pH b) Taking of drinks with alkaline pH c) Taking of saline drinks d) Restriction of drinking 006. Resorptive sulfonamides have the following unwanted effects on blood system: a) Hemolytic anemia b) Thrombocytopenia c) Granulocytopenia d) All of the above 007. Sulfonamides have the following unwanted effects: a) Hematopoietic disturbances b) Crystalluria c) Nausea, vomiting and diarrhea d) All of the above 009. Tick the drug, which is effective against mycobacteria only: a) Isoniazid b) Streptomycin c) Rifampin 130 d) Kanamycin 010. Rifampin has the following unwanted effect: a) Dizziness, headache b) Loss of hair c) Flu-like syndrome, tubular necrosis d) Hepatotoxicity 019. Isoniazid has following unwanted effect: a) Cardiotoxicity b) Hepatotoxicity, peripheral neuropathy c) Loss of hair d) Immunotoxicity 020. Ethambutol has the following unwanted effect: a) Cardiotoxicity b) Immunetoxicity c) Retrobulbar neuritis with red-green color blindness d) Hepatotoxicity 021. Streptomycin has the following unwanted effect: a) Cardiotoxicity b) Hepatotoxicity c) Retrobulbar neuritis with red-green color blindness d) Ototoxicity, nephrotoxicity 131 022. Combined chemotherapy of tuberculosis is used to: a) Decrease mycobacterium drug-resistance b) Increase mycobacterium drug-resistance c) Decrease the antimicrobal activity d) Decrease the onset of antimycobacterial drugs biotransformation: 026. Tick the indications for nitrofuranes: a) Infections of respiratory tract b) Infections of urinary and gastro-intestinal tracts c) Syphilis d) Tuberculosis 031. Tick the unwanted effects of nitrofuranes: a) Nausea, vomiting b) Allergic reactions c) Hemolytic anemia d) All of the above 032. Tick the indications for Metronidazole: a) Intra-abdominal infections, vaginitis, enterocolitis b) Pneumonia c) As a disinfectant d) Influenza 033. Tick the unwanted effects of Metronidazole: a) Nausea, vomiting, diarrhea, stomatitis b) Hypertension c) Disturbances of peripheral blood circulation d) All of the above 034. Fluoroquinolones are active against: a) Gram negative microorganisms only b) Mycoplasmas and Chlamidiae only c) Gram positive microorganisms only d) Variety of Gram-negative and positive microorganisms, including Mycoplasmas and Chlamidiae 036. Tick the unwanted effects of fluoroquinolones: a) Hallucinations b) Headache, dizziness, insomnia c) Hypertension d) Immunetoxicity 037. Tick the indications for fluoroquinolones: a) Infections of the urinary tract b) Bacterial diarrhea c) Infections of the urinary and respiratory tract, bacterial diarrhea d) Respiratory tract infections 038. Tick the drug used for malaria chemoprophylaxis and treatment: a) Chloroquine b) Quinidine c) Quinine d) Sulfonamides 002. Tick the drug used for amoebiasis treatment: a) Nitrofurantoin b) Iodoquinol c) Pyrazinamide d) Mefloquine 003. Tick the drug used for trichomoniasis treatment: a) Metronidazole b) Suramin c) Pyrimethamine d) Tetracycline 004. Tick the drug used for toxoplasmosis treatment: a) Chloroquine b) Tetracyclin c) Suramin d) Pyrimethamine 005. Tick the drug used for balantidiasis treatment:: a) Azitromycin b) Tetracycline c) Quinine d) Trimethoprim 006. Tick the drug used for leishmaniasis treatment: a) Pyrimethamine b) Albendazole c) Sodium stibogluconate d) Tinidazole 007. Tick the antimalarial drug belonging to 8-aminoquinoline derivatives: a) Doxycycline b) Quinidine c) Primaquine d) Chloroquine 133 008. Tick the antimalarial drug belonging to pyrimidine derivatives: a) Mefloquine b) Pyrimethamine c) Quinidine d) Chloroquine 010. Tick the drug used for trypanosomosis treatment: a) Melarsoprol b) Metronidazole c) Tetracyclin d) Quinidine 011. Tick the antimalarial drug having a gametocidal effect: a) Mefloquine b) Primaquine c) Doxycycline d) Sulfonamides 012. Tick the antimalarial drug influencing tissue schisonts: a) Mefloquine b) Chloroquine c) Quinidine d) Primaquine 014. Tick the group of antibiotics having an antimalarial effect: a) Aminoglycosides b) Tetracyclins c) Carbapenems d) Penicillins 015. Tick the amebecide drug for the treatment of an asymptomatic intestinal form of amebiasis: a) Chloroquine b) Diloxanide c) Emetine d) Doxycycline 016. Tick the drugs for the treatment of an intestinal form of amebiasis: a) Metronidazole and diloxanide b) Diloxanide and streptomycin c) Diloxanide and Iodoquinol d) Emetine and metronidazole 017. Tick the drug for the treatment of a hepatic form of amebiasis: a) Diloxanide or iodoquinol b) Tetracycline or doxycycline c) Metronidazole or emetine d) Erythromycin or azitromycin 018. Tick the luminal amebecide drug: a) Metronidazole b) Emetine c) Doxycycline d) Diloxanide 019. Tick the drug of choice for the treatment of extraluminal amebiasis: a) Iodoquinol b) Metronidazole c) Diloxanide d) Tetracycline 020. Tick the drug, blocking acetylcholine transmission at the myoneural junction of helminthes: 134 a) Levamisole b) Mebendazole c) Piperazine d) Niclosamide 021. Tick niclosamide mechanism of action: a) Increasing cell membrane permeability for calcium, resulting in paralysis, dislodgement and death of helminthes b) Blocking acetylcholine transmission at the myoneural junction and paralysis of helminthes c) Inhibiting microtubule synthesis in helminthes and irreversible impairment of glucose uptake d) Inhibiting oxidative phosphorylation in some species of helminthes 022. Tick praziquantel mechanism of action: a) Blocking acetylcholine transmission at the myoneural junction and paralysis of helminthes b) Inhibiting microtubule synthesis in helminthes and irreversible impairment of glucose uptake c) Increasing cell membrane permeability for calcium, resulting in paralysis, dislodgement and death of helminthes d) Inhibiting oxidative phosphorylation in some species of helminthes 023. Tick piperazine mechanism of action: a) Inhibiting microtubule synthesis in helminthes and irreversible impairment of glucose uptake b) Blocking acetylcholine transmission at the myoneural junction and paralysis of helminthes c) Inhibiting oxidative phosphorylation in some species of helminthes d) Increasing cell membrane permeability for calcium, resulting in paralysis, dislodgement and death of helminthes 024. Tick the drug, a salicylamide derivative: a) Praziquantel b) Piperazine c) Mebendazole d) Niclosamide 025. Tick mebendazole mechanism of action: a) Inhibiting oxidative phosphorylation in some species of helminthes b) Increasing cell membrane permeability for calcium, resulting in paralysis, dislodgement and death of helminthes c) Inhibiting microtubule synthesis in helminthes and irreversible impairment of glucose uptake d) Blocking acetylcholine transmission at the myoneural junction and paralysis of helminthes 026. Tick the drug, inhibiting oxidative phosphorylation in some species of helminthes: a) Niclosamide b) Piperazine c) Praziquantel d) Mebendazole 027. Tick the drug for neurocysticercosis treatment: a) Praziquantel b) Pyrantel c) Piperazine d) Bithionol 028. Tick the drug for nematodosis (roundworm invasion) treatment: a) Niclosamide b) Praziquantel c) Bithionol d) Pyrantel 029. Tick the drug for cestodosis (tapeworm invasion) treatment: a) Piperazine b) Praziquantel c) Pyrantel d) Ivermectin 030. Tick the drug for trematodosis (fluke invasion) treatment: a) Bithionol b) Ivermectin c) Pyrantel d) Metronidazole 031. Tick the drug, a benzimidazole derivative: a) Praziquantel b) Mebendazole c) Suramin d) Pyrantel 032. Tick the broad spectrum drug for cestodosis, trematodosis and cycticercosis treatment: 135 a) Piperazine b) Ivermectine c) Praziquantel d) Pyrantel 033. Tick the drug for ascaridosis and enterobiosis treatment: a) Bithionol b) Pyrantel c) Praziquantel d) Suramin 034. Tick the drug for strongiloidosis treatment: a) Niclosamide b) Praziquantel c) Bithionol d) Ivermectin 035. Tick the drug, a derivative of adamantane: a) Didanozine b) Rimantadine c) Gancyclovir d) Foscarnet 003. Tick the drug, a derivative of pyrophosphate: a) Foscarnet b) Zidovudine c) Vidarabine d) Acyclovir 004. Tick the drug, inhibiting viral reverse transcriptase: a) Zidovudine b) Vidarabine c) Rimantadine d) Gancyclovir 007. Tick the drug, inhibiting viral proteases: a) Rimantadine b) Acyclovir c) Saquinavir d) Zalcitabine 008. Tick the drug of choice for herpes and cytomegalovirus infection treatment: a) Saquinavir b) Interferon alfa c) Didanozine d) Acyclovir 136 009. Tick the drug which belongs to nonnucleoside reverse transcriptase inhibitors: a) Zidovudine b) Vidarabine c) Nevirapine d) Gancyclovir 010. Tick the drug used for influenza A prevention: a) Acyclovir b) Rimantadine c) Saquinavir d) Foscarnet 012. Tick the antiviral drug which belongs to endogenous proteins: a) Amantadine b) Saquinavir c) Interferon alfa d) Pencyclovir 014. Tick the drug which belongs to nucleoside reverse transcriptase inhibitors: a) Didanosine b) Gancyclovir c) Nevirapine d) Vidarabine 015. Tick the unwanted effects of zidovudine: a) Hallucinations, dizziness b) Anemia, neutropenia, nausea, insomnia c) Hypertension, vomiting d) Peripheral neuropathy 017. Tick the unwanted effects of intravenous acyclovir infusion: a) Renal insufficiency, tremors, delerium b) Rash, diarrhea, nausea c) Neuropathy, abdominal pain d) Anemia, neutropenia, nausea, insomnia 018. Tick the drug that can induce peripheral neuropathy and oral ulceration: a) Acyclovire b) Zalcitabine c) Zidovudine d) Saquinavir 019. Tick the unwanted effects of didanozine: a) Hallucinations, dizziness, insomnia b) Anemia, neutropenia, nausea c) Hypertension, vomiting, diarrhea d) Peripheral neuropathy, pancreatitis, diarrhea, hyperuricemia 020. Tick the unwanted effects of indinavir: a) Hypotension, vomiting, dizziness b) Nephrolithiasis, nausea, hepatotoxicity c) Peripheral neuropathy, pancreatitis, hyperuricemia d) Anemia, neutropenia, nausea 021. Tick the drug that can induce nausea, diarrhea, abdominal pain and rhinitis: 137 a) Acyclovire b) Zalcitabine c) Zidovudine d) Saquinavir 022. Rational combination of anticancer drugs is used to: a) Provide synergism resulting from the use of anticancer drugs with different mechanisms combination b) Provide synergism resulting from the use of anticancer drugs with the same mechanisms combination c) Provide stimulation of immune system d) Provide stimulation of cell proliferation 024. Tick the anticancer alkylating drug, a derivative of chloroethylamine: a) Methotrexate b) Cisplatin c) Cyclophosphamide d) Carmustine 025. Tick the anticancer alkylating drug, a derivative of ethylenimine: a) Mercaptopurine b) Thiotepa c) Chlorambucil d) Procarbazine 026. Tick the group of hormonal drugs used for cancer treatment: a) Mineralocorticoids and glucocorticoids b) Glucocorticoids and gonadal hormones c) Gonadal hormones and somatotropin d) Insulin 027. Tick the anticancer alkylating drug, a derivative of alkylsulfonate: a) Fluorouracil b) Carboplatin c) Vinblastine d) Busulfan 028. Tick the anticancer drug of plant origin: a) Dactinomycin b) Vincristine c) Methotrexate d) Procarbazine 029. Tick the anticancer drug, a pyrimidine antagonist: a) Fluorouracil b) Mercaptopurine c) Thioguanine d) Methotrexate 031. Methotrexate is: a) A purine antagonist b) A folic acid antagonist c) An antibiotic d) An alkylating agent 032. Tick the antibiotic for cancer chemotherapy: a) Cytarabine b) Doxorubicin c) Gentamycin d) Etoposide 033. Fluorouracil belongs to: a) Antibiotics 138 b) Antimetabolites c) Plant alkaloids d) Bone marrow growth factor 034. General contraindications for anticancer drugs are: a) Depression of bone marrow b) Acute infections c) Severe hepatic and/or renal insufficiency d) All of the above 036. Action mechanism of methotrexate is: a) Inhibition of dihydrofolate reductase b) Activation of cell differentiation c) Catabolic depletion of serum asparagine d) All of the above 037. Tick the anticancer drug belonging to inorganic metal complexes: a) Dacarbazine b) Cisplatin c) Methotrexate d) Vincristine 038. Tick the indication for estrogens in oncological practice: a) Leukemia b) Cancer of prostate c) Endometrial cancer d) Brain tumors 039. Tick the group of drugs used as subsidiary medicines in cancer treatment: a) Cytoprotectors b) Bone marrow growth factors c) Antimetastatic agents d) All of the above 042. Tick the estrogen inhibitor: a) Leuprolide b) Tamoxifen c) Flutamide d) Anastrozole 043. Tick the antiandrogen drug: a) Flutamide b) Aminoglutethimide c) Tamoxifen d) Testosterone 044. Tick the drug belonging to aromatase inhibitors: a) Octreotide b) Anastrozole c) Flutamide d) Tamoxifen 045. Tick the drug belonging to gonadotropin-releasing hormone agonists: a) Leuprolide b) Tamoxifen 139 c) Flutamide d) Anastrozole. Navigational Note: Leukocytosis >100,000/mm3 Clinical manifestations of leucostasis; urgent intervention indicated Definition: A disorder characterized by laboratory test results that indicate an increased number of white blood cells in the blood. Navigational Note: Thrombotic Laboratory findings with thrombocytopenic purpura clinical consequences.
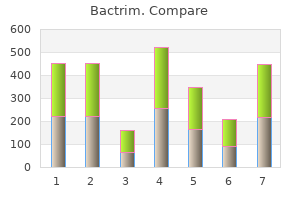
Thus virus 20 order 480 mg bactrim amex, our data indicate that it would be safe to delay colposcopic evaluation of women negative for p16/Ki-67 and await further testing antibiotic used for uti 960 mg bactrim sale. These findings support that p16/Ki-67 can be a viable option for cytology triage infection in bone discount 960mg bactrim with mastercard, if proven cost-effective antibiotic resistance diagnostics order bactrim 480mg without prescription. We were not able to measure p16/Ki-67 in the referral cytology specimen to simulate a reflex triage approach bacteria proteus mirabilis safe 480 mg bactrim. Overall antimicrobial susceptibility test 7 2 purchase bactrim 960 mg line, the specificity estimates in our population were comparable, albeit slightly lower than what has been reported in 2 studies sponsored by the manufacturer of the p16/Ki-67 double-stain assay (9, 10). We had excellent disease ascertainment because an extended biopsy protocol was used with up to 4 targeted biopsies. Thus, we were able to distinguish true-positive from falsepositive test results better than in studies where disease is missed because of insensitive colposcopic biopsy protocols. Our assays were conducted from the same specimen type (residual PreservCyt material), run in the same laboratory and evaluated according to the same criteria as the previous studies. The major promise of the p16/Ki-67 double-stain assay is that is does not require adjunct morphologic interpretation of positive cells and vastly simplifies the evaluation process compared with p16 staining alone. We sought to evaluate the assay according to this premise, without extensive review and adjudication of the slides. Currently, the test is considered positive when at least one cell exhibits p16/Ki-67 costaining. While this approach obviously has a high sensitivity, increasing the threshold may lead to a better overall tradeoff between sensitivity and specificity. With the performance characteristics observed in our study, p16/Ki-67 could safely reduce colposcopy referral by almost half in the overall population, with a higher reduction seen in women 30 years and older. If cytologic immunostains such as p16/Ki-67 or other biomarkers are to be widely accepted, automated evaluation strategies will be important. We have previously shown that automated evaluation of p16 staining on cytologic slides is feasible (21) and will continue to adapt the algorithms to p16/Ki-67 staining. In summary, in a large colposcopy population with excellent disease ascertainment due to an aggressive colposcopic biopsy protocol, we show that p16/Ki-67 cytology has a high sensitivity and specificity for detecting cervical precancer that may warrant use of p16/Ki-67 testing to reduce colposcopy referral. Walker Acquisition of data (provided animals, acquired and managed patients, provided facilities, etc. Walker Grant Support the study was supported by the Intramural Research Program of the National Cancer Institute. The costs of publication of this article were defrayed in part by the payment of page charges. This article must therefore be hereby marked advertisement in accordance with 18 U. Received January 25, 2012; revised May 24, 2012; accepted May 29, 2012; published OnlineFirst June 6, 2012. Long term predictive values of cytology and human papillomavirus testing in cervical cancer screening: joint European cohort study. Human papillomavirus and cervical cancer: biomarkers for improved prevention efforts. Tsoumpou I, Arbyn M, Kyrgiou M, Wentzensen N, Koliopoulos G, Martin-Hirsch P, et al. Human papillomavirus cofactors by disease progression and human papillomavirus types in the study to understand cervical cancer early endpoints and determinants. Human papillomavirus type distribution in 30,848 invasive cervical cancers worldwide: variation by geographical region, histological type and year of publication. Persistence of type-specific human papillomavirus infection and increased long-term risk of cervical cancer. The absolute risk of cervical abnormalities in high-risk human papillomavirus-positive, cytologically normal women over a 10-year period. A long-term prospective study of type-specific human papillomavirus infection and risk of cervical neoplasia among 20,000 women in the Portland Kaiser Cohort Study. Natural history of cervical neoplasia and risk of invasive cancer in women with cervical intraepithelial neoplasia 3: a retrospective cohort study. A virtual microscopy system to scan, evaluate and archive biomarker enhanced cervical cytology slides. Updated version Supplementary Material Access the most recent version of this article at: doi:10. To request permission to re-use all or part of this article, use this link clincancerres. Ultrasound is a practical and economic imaging modality in local staging of cervical cancer [24]. It is important for 2185 the clinicians to plan the individual treatment of a patient [27]. The patients with early stage cervical cancer planned for primary surgery and the patients with locally advanced cervical cancer arranged for surgery after neoadjuvant treatment. Histological examination showed parametrial infiltration in four patients; these were detected during ultrasound examination. Transvaginall ultrasound image gray scale and color Doppler shows a longitudinal section of the uterus with cervical cancer of the female aged 68-year-old. A prospective multicenter study involved preoperative prediction of lymph node metastasis and deep stromal invasion in women with cervical cancer by using two-dimensional (2D) and 3D ultrasound indices [30]. The results showed that 3D vascular indices were ineffective in speculating advanced stages of the disease [30]. Postoperative treatment was significantly more prevalent in patients with profuse vascularization [35]. The level of p53 and transvaginal color Doppler ultrasound could provide valuable clinical information for the treatment and monitoring of cervical cancer [36]. Ultrasound findings as prognostic factors Furthermore, angiogenesis, the formation of new vessels in a specific area, is required for tumor growth and progression [32]. Table 2 showed studies involving ultrasound findings as prognostic factors of cervical cancer patients. Ultrasound findings as prognostic factors of cervical cancer patients Ultrasound Imaging modality Transvaginal color Doppler ultrasound Transvaginal color Doppler ultrasound Number of patients evaluated 27 patients early stage invasive cervical cancer Performance Reference Prediction of treatment response Several studies have evaluated the role of ultrasound for predicting the response to varied treatment in women with cervical cancer. After 2weeks of neoadjuvant treatment, patients with partial response had significantly greater tumor volume than those with complete response (P=0. Color Doppler findings associated with risk factors was reported by a study involving neoangiogenesis measured in early cervical cancer cases [35]. The risk factors (depth stromal invasion, parametrial and vaginal margin involvement, positive lymph nodes, lymph-vascular space involvement) were recorded. The power Doppler vascularity index could be useful to predict the response to neoadjuvant chemotherapy in cervical cancer [38]. Transvaginal Color Doppler sonography used to predict the response to chemotherapy in patients with advanced cervical cancer was reported [40]. A decrease in peak systolic velocity and a significant increase in resistance and pulsatility index values were noted in ten patients who responded to chemotherapy. Doppler parameters could be clinically useful in the assessment of the response to neoadjuvant chemotherapy [40]. Among 34 patients with squamous cell carcinoma, Serum markers detected local disease with 20. The evaluation of radiotherapy response of cervical cancer by suing gray scale and color Doppler ultrasonography was report [45]. There was a significant difference between increased resistive indices and complete response to the treatment (P=0. Prediction of response to neoadjuvant chemoradiation the residual tumor in locally advanced cervical cancer patients receiving chemoradiation and radical surgery was assessed by 3D power Doppler, 2D ultrasound parameters, or contrast-enhanced indices [42]. The results showed that grayscale and color Doppler ultrasound have low levels of diagnostic performances of detecting residual disease after neoadjuvant chemoradiation for locally advanced cervical cancer patients [42]. The echogenicity, homogeneity and heterogeneity of tumors were calculated in reference of six ultrasonic histogram parameters [47]. The peak intensity value of the histogram increased rapidly since the first week after therapy initiation; the width of the low-intensity and the high-intensity and the area under high intensity portions of the curve changed significantly at the second week. Imaging during the primary diagnostic work-up is essential for accurately assessment of tumor extent and selecting the best therapeutic option for cervical cancer patients. Ultrasound may be a useful modality to evaluate local extent of disease in cervical cancer. Tumor vascularization by Doppler ultrasound could be useful for monitoring and predict response to therapy. Application of ultrasound in intraoperative guidance the role of intraoperative ultrasound guidance in intracavitary brachytherapy of cervical cancer was investigated in a recent retrospectively study [48]. Ultrasound guidance was performed for tandem selection and appropriate application. Intracavitary brachytherapy was done under ultrasound guidance for 412 insertions in 113 patients with cervical cancer. The authors concluded that intraoperative sonographic guidance provided effectiveness for intracavitary brachytherapy of cervical cancer and decreased rates of perforations [48]. The previous study, involving intraoperative ultrasound guidance while intracavitary brachytherapy applicator placement for cervical cancer patients, also showed the same results [49]. Intraoperative ultrasound guidance increased the rate of successful applicator placement [49]. In a recent systematic review and meta-analysis, a decrease of uterine perforations by using ultrasound image-guided applicator insertion for cervical carcinoma patients underwent intracavitary brachytherapy was revealed [50]. The investigators claimed that it was helpful in accurate placements of needles resulted in avoiding the injury to normal pelvic structures [51]. A multi-variate analysis of prognostic variables in the Gynecologic Oncology Group. What Is the Role of Imaging at Primary Diagnostic Work-Up in Uterine Cervical Cancer Sonographic characteristics of squamous cell cancer and adenocarcinoma of the uterine cervix. Three-dimensional power Doppler ultrasound for the study of cervical cancer and precancerous lesions. Transvaginal color doppler sonography combined with colposcopy for diagnosis of early stage cervical cancer and precancerous lesions. Accuracy of three-dimensional ultrasonography in volume estimation of cervical carcinoma. Three-dimensional transvaginal sonography in local staging of cervical carcinoma: description of a novel technique and preliminary results. Early-stage cervical cancer: tumor delineation by magnetic resonance imaging and ultrasound - a European multicenter trial. Agreement of two-dimensional and three-dimensional transvaginal ultrasound with magnetic resonance imaging in assessment of parametrial infiltration in cervical cancer. Three-Dimensional Transvaginal Sonography and Magnetic Resonance Imaging for Local Staging of Cervical Cancer: An Agreement Study. Transrectal ultrasound in the evaluation of cervical carcinoma and comparison with spiral computed tomography and magnetic resonance imaging. Three-dimensional transvaginal ultrasonography for locally advanced cervical cancer. Ultrasound scanning of the pelvis and abdomen for staging of gynecological tumors: a review. Transvaginal ultrasonography and magnetic resonance imaging for assessment of presence, size and extent of invasive cervical cancer. Early-stage cervical cancer: agreement between ultrasound and histopathological findings with regard to tumor size and extent of local disease. Preoperative prediction of lymph node metastasis and deep stromal invasion in women with invasive cervical cancer: prospective multicenter study using 2D and 3D ultrasound. Transrectal ultrasound and magnetic resonance imaging in staging of early cervical cancer. Neoangiogenesis in early cervical cancer: correlation between color Doppler findings and risk factors. Correlations of p53 expression with transvaginal color Doppler ultrasound findings of cervical cancer after radiotherapy. Power Doppler vascularity index for predicting the response of neoadjuvant chemotherapy in cervical carcinoma. Transrectal ultrasound and magnetic resonance imaging in the evaluation of tumor size following neoadjuvant chemotherapy for locally advanced cervical cancer. Transvaginal color Doppler sonography in predicting the response to chemotherapy in advanced cervical cancer. The Role of 2D/3D Ultrasound to Assess the Response to Neoadjuvant Chemotherapy in Locally Advanced Cervical Cancer. Transvaginal color Doppler for predicting pathological response to preoperative chemoradiation in locally advanced cervical carcinoma: a preliminary study. Three-dimensional power Doppler ultrasound in cervical carcinoma: monitoring treatment response to radiotherapy. Evaluation of radiotherapy response of cervical carcinoma with gray scale and color Doppler ultrasonography: 2189 resistive index correlation with magnetic resonance findings. Transvaginal color Doppler sonography for predicting response to concurrent chemoradiotherapy for locally advanced cervical carcinoma. Ultrasonic histogram assessment of early response to concurrent chemo-radiotherapy in patients with locally advanced cervical cancer: a feasibility study. Intraoperative sonographic guidance for intracavitary brachytherapy of cervical cancer. Intraoperative ultrasound guidance during intracavitary brachytherapy applicator placement in cervical cancer: the University of Alabama at Birmingham experience. Decrease in uterine perforations with ultrasound image-guided applicator insertion in intracavitary brachytherapy for cervical cancer: A systematic review and meta-analysis. Use of transrectal ultrasound for high dose rate interstitial brachytherapy for patients of carcinoma of uterine cervix. Monovalent, bivalent and quadrivalent vaccines have been tested in randomized, controlled trials and have shown remarkably consistent results in providing protection against the types included in the vaccines.
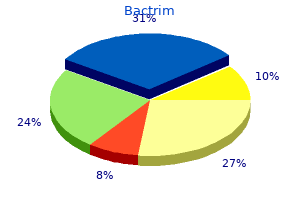
Other motorized vehicles antibiotics pharmacology buy discount bactrim 480 mg, such as motorcycles antibiotic 7146 order bactrim 480 mg free shipping, personal watercraft infection 3 months after surgery 960mg bactrim mastercard, all terrain vehicle (four wheel) antibiotic in spanish cheap bactrim 960mg with mastercard, and boats may pose less of a threat to a person with epilepsy than does flying virus 09 960 mg bactrim otc. If the person with epilepsy operating the vehicle has a prolonged and consistent aura infection humanitys last gasp generic bactrim 480 mg visa, it may allow that person the opportunity to stop and protect ones self. However, other factors should be considered by a person with epilepsy when contemplating engaging in some of these activities. The use Chapter 94: Driving and Social Issues in Epilepsy 1055 of a personal flotation device at all times when operating or riding in any watercraft should be considered. When operating off-road vehicles, safety equipment should also be considered, especially the use of boots, shoulder pads, protective clothing, and helmets. Although a person operating such a vehicle does not require a license, specific training courses are available and are highly recommended. In contrast, organized motor sports generally require some form of medical clearance before participation (39). Each series requires approval from a qualified health care professional before driving, and therefore specific rules should be reviewed. The Person with Epilepsy and Athletics the decision to participate in individual. The extent to which a person with epilepsy wishes to pursue athletics is an individual decision that should be based on individual circumstances. Each team or individual sport presents different challenges that may affect a person with epilepsy in different ways. For example, the potential injury a person with epilepsy might sustain during golf, tennis, or running track is likely to be low, whereas a seizure sustained during boxing, hang gliding, ski flying, or waterskiing would pose a much higher risk. Football could be dangerous if a player is unable to protect him- or herself during a play, whereas basketball is less likely to be dangerous. Noncommercial scuba diving is also not regulated from a medical standpoint, but good judgment is required on the part of the participant. Hyperventilation techniques and the high concentration of inspired oxygen used during scuba diving have the potential to provoke seizures. The person with epilepsy should also inform his or her dive buddy, instructor, and dive master of the potential risk should a seizure occur during diving. A review of drowning deaths found that 40% of seizure-related drownings occurred during recreational activities (42). A study by Gotze found no increase in seizure occurrence during strenuous swimming (43). The available data on such seizures are limited, suggesting that sports participation does not provoke seizure recurrence (44), and in some cases may even reduce seizure occurrence (43). Recent opinion has encouraged sports participation for the person with epilepsy despite the potential risks (45,46). The decision regarding person with epilepsy participation in sporting activities must be made on an individual basis. For example, zonisamide reduces sweating in children and could potentially lead to heat-related injury in hot climates. Tremor associated with the use of valproic acid could be dangerous when shooting target pistols. Phenytoin-induced ataxia could potentially be deadly while riding a motorbike (47). Individualizing the specific drug side-effect profile, patient characteristics, and particular recreational activity generally should all be considered when advising the person with epilepsy about participation in recreational and sporting activities. In addition to the usual concerns persons with epilepsy have about seizure control and medication effects, social issues play an important role in their everyday lives. Consensus conference on driver licensing and epilepsy: American Academy of Neurology, American Epilepsy Society, and Epilepsy Foundation of America. To drive or not to drive: the 3-month seizure-free interval for people with epilepsy [editorial]. Counselling for driving restrictions in epilepsy and other causes of temporary impairment of consciousness: how are we doing Epilepsy and motor vehicle driving-a symposium held in Quebec City, November 1998. Reporting epileptic drivers to licensing authorities is unnecessary and counterproductive. Factors associated with the employment problems of people with established epilepsy. Socioeconomic prognosis after a newly diagnosed unprovoked epileptic seizure in adults: a populationbased case-control study. Effect of physical exercise on seizure threshold (investigated by electroencephalographic telemetry). It must be emphasized that each patient has individual characteristics requiring knowledge of the specific activity in which the person with epilepsy wishes to participate. The first seizure in adult life: value of clinical features, electroencephalography, and computerised tomographic scanning in prediction of seizure recurrence. National Highway Traffic Safety Administration, National Center for Statistics and Analysis. Seizure-related motor vehicle crashes in Arizona before and after reducing the driving restriction from 12 to 3 months. Accident experience and notification rates in people with recent seizures, epilepsy or undiagnosed episodes of loss of consciousness. Physicians traditionally are trained to evaluate seizure semiology, and look for electrophysiologic and structural brain abnormalities to support a diagnosis of epilepsy. For example, a recent study found that the average neurology outpatient visit for epilepsy in the community setting lasted 12 minutes (1). Such a short clinical interaction requires exquisite organization to render optimal care. This chapter reviews available data from clinical outcomes studies that support specific strategies to improve the results of outpatient care for epilepsy. The initial steps toward optimal outpatient epilepsy care require that five questions be answered, which will be explored in the following sections: 1. Nonepileptic, psychogenic seizures are estimated to be up to 10% of all cases of epilepsy and 20% to 30% of pharmacoresistant cases (13,14). Interestingly, time to first seizure did not correlate with self-reported seizure rate in the most recent outpatient clinic visit. There was no significant difference in time to diagnostic event between the very low seizure rate patients and those with more frequent self-reported seizures. Although the reasons for this finding are not clear, inaccuracy of self-reported rates may be a major factor. A very large majority of patients with self-reported seizure rates of 1 per month will have a diagnostic event recorded within 6 days. For example, juvenile myoclonic epilepsy is estimated to be 10% of all epilepsy cases, but is frequently misdiagnosed for years after initial presentation. A left-sided seizure onset, but not temporal or frontal lobe localization, was associated with documentation failure. Based on this innovative study, the authors concluded that "patient seizure counts do not provide valid information. The authors concluded that "the outcome of this project underscores the unsatisfactory status of antiepileptic therapy with the medications currently available. Most patients whose epilepsy is reasonably controlled must tolerate some side effects. Self-reported seizure rate, with supplemental input from family and friends, is the standard outcome measure for both clinical care and research. However, available data that have been replicated in adults and children indicate that patient or family reporting is highly inaccurate. A particularly problematic finding was that the patients with the lowest seizures rates reported in outpatient visits had the greatest proportion of seizures that were not identified by them in monitoring unit. After more than 10 years of absence of publications on this important aspect of epilepsy care, Hoppe et al. It contains 19 items that are brief descriptions of a subjective experience of a toxic medication effect. The instructions ask the person to rank the frequency of each adverse effect on a 1 to 4 Likert-like scale during the past 4 weeks. This study demonstrated the importance of systematic screening in clinical epilepsy care, and also of value of the quantification of medication toxicity in health outcomes research in epilepsy. Although by definition, epilepsy is a condition characterized by brief paroxysmal disturbances of brain function, the supposition that between seizures every person with epilepsy reverts to a condition without epilepsy is obviously too optimistic. Symptomatic epilepsies are a comorbidity, with disorders affecting the brain and, as indicated by the label cryptogenic, probably many more epilepsies than those diagnosed as symptomatic fall into that category. The primary brain disorder itself may determine to a great extent the condition of the person with epilepsy in the interictal period. Accurate recording of the effects of comorbidity should not be limited to routine neurologic, psychological, and psychiatric examination, but should include a measure of quantification (6). Similar to epilepsy, depression may be a term used for a variety of disorders with differing etiologies and complex interactions with social, vocational, and neuropsychological functioning. Depression is recognized as a common comorbid condition in persons with epilepsy, especially in tertiary care samples (27,28) and more recently in population (29,30) and community-based studies (31). Although interpretation of the literature on depression in epilepsy is complicated by varying ascertainment methods, definitions of depression, and sample characteristics, available estimates indicate that the prevalence of clinically relevant depression is 30% to 50% in persons with refractory epilepsy and 10% to 30% in controlled epilepsy. Additional support for the significance of depression in epilepsy includes the observation that suicide rates are significantly higher than the general population (32,33). The etiology of depression in epilepsy is not fully understood and is very likely multifactorial, even on an individual level (7,34). However, specific psychological and neurologic factors have been associated with depression in epilepsy. Less information is available regarding the neurobiology of anxiety symptoms and epilepsy (41,42). Furthermore, depression is associated with increased health care utilization and costs in persons with epilepsy (25). The optimal approaches to treatment of depression and anxiety in epilepsy have received relatively little attention compared to its impact on the epilepsy community. Several important issues must be considered, such as efficacy of antidepressant medications in the setting of epileptic brain dysfunction, additional adverse effects of antidepressants, and the unique social and vocational disabilities in epilepsy that may make cognitive and behavioral therapies particularly valuable (7). In 1985, Robertson and Trimble described the results of a randomized, double-blind comparison of amitriptyline, nomifesine, and placebo in 42 patients with depression and epilepsy (43). Although the mean scores of the Hamilton Depression Rating Scale and the Beck Depression Inventory scores improved by 50% after treatment, similar improvement in the placebo group resulted in no significant difference in outcome between any group at 6 weeks. A second 6-week treatment phase without placebo control compared higher doses of each drug (150 mg), and found that the nomifesine group had significantly better Hamilton Depression Rating Scale but not Beck Depression Inventory scores. The authors concluded "our results suggest that, in patients with depression and epilepsy, immediate prescription with antidepressants may not be indicated" (43). Although each of the drugs was associated with significant reduction in depression symptoms at the 24- to 30-week assessment, mirtazapine had a higher dropout rate due to unacceptable side effects. Similar to another study using sertraline (45), no significant increase in seizure was observed (44). Nonpharmacologic treatments for depression have not received adequate systematic evaluations to draw conclusions about efficacy in persons with epilepsy. Additional research is needed to provide the necessary evidence to guide optimal care of persons with epilepsy and comorbid depression and anxiety. Identification of surgical candidates early in the course of their pharmacoresistance seems mandatory for optimal care. This complexity creates challenges for the clinician in the outpatient clinic setting, especially considering common time and resource constraints. Utilization of available reliable and valid screening tools and implementation of existing practice guidelines can support delivery of the most effective care for persons suffering the multifactorial disability of epilepsy. Conversations between community-based neurologists and patients with epilepsy: results of an observational linguistic study Epilepsy Behav. Systematic screening allows reduction of adverse antiepileptic drug effects: a randomized trial. Chapter 95: Achieving Health in Epilepsy: Strategies for Optimal Evaluation and Treatment 4. Depression but not seizure frequency predicts quality of life in treatment-resistant epilepsy. Quality of life of epilepsy surgery patients as compared with outpatients with hypertension, diabetes, heart disease, and/or depressive symptoms. Self-reported seizure frequency and time to first event in the seizure monitoring unit. Seizure frequency in children with epilepsy: factors influencing accuracy and parental awareness. Quality of life outcomes of immediate or delayed treatment of early epilepsy and single seizures. The impact of comorbid depression on health resource utilization in a community sample of people with epilepsy. Clinical assessment of axis I psychiatric morbidity in chronic epilepsy: a multicenter investigation. Depression in epilepsy: prevalence, clinical semiology, pathogenic mechanisms, and treatment.
Generic bactrim 480 mg overnight delivery. Wound Healing Clinic Video.
References